Ultimate Resource On Long COVID or (PASC)
Some people with COVID-19 continue to have lingering symptoms for weeks or months after they begin to recover. Ultimate Resource On Long COVID or (PASC)
You might know this as “long COVID.” Experts have coined a new term for it: post-acute sequelae SARS-CoV-2 infection (PASC).
Research says about 10% of people with COVID-19 get long COVID. But it can happen to anyone whether you’re young, old, healthy, or have chronic illness. You can get it even if your early COVID-19 symptoms were mild to moderate, or regardless of whether or not you went to the hospital for them.
Experts Don’t Know Why People Get Long COVID. Research Continues On That, As Well As:
* Treatment And Prevention
* How Long It Can Take To Recover From It
* Whether Long Covid Can Make Heart And Brain Problems More Likely
* How Someone Can Build Immunity After They Have Covid-19
* What Role Vaccines Play
In the meantime, if your doctor diagnoses you with long COVID, they may order blood tests to see if you have any underlying issues that might cause it. They’ll also take a look at your medical history.
Related:
Harvard Chemical Biology Department Chair Accused Of Selling Covid19 To Wuhan University
Paying Off Unfunded Pension Liabilities Will Be A Low Priority After COVID-19
US Says China Backed Hackers Who Targeted COVID-19 Vaccine Research
Ultimate Resource For Covid-19 Vaccine Passports
Companies Plan Firings For Anti-Vaxers And Giveaways For Covid-19 Vaccine Recipients
Four Stories Of How People Traveled During Covid
How To Travel Luxuriously Post- Covid-19, From Private Jets To Hotel Buyouts
‘I Cry Every Day’: Olympic Athletes Slam Food, COVID Tests And Conditions In Beijing
Lessons Of The Great Depression: Preserving Wealth Amid The Covid-19 Crisis
Cyber Attack Hits Health And Human Services Department Amid Covid-19 Outbreak
Symptoms
Long COVID appears to affect each person differently. You might feel a wide range of things that could linger for a long time. Common symptoms include:
* Fatigue
* Brain Fog
* Loss Of Smell And Taste
* Shortness Of Breath
* Cough
* Joint Pain
* Chest Pain
You Might Also Have:
* Sleep Issues
* Anxiety
* Gut Problems
* Fever
* Muscle Pain
* Depression
* Headache
* Rapid Heartbeat
In Rare Cases, Long Covid Can Affect Your Organs. You May Get:
* Inflammation Of Your Heart Muscle
* Lung-Related Issues
* Kidney Problems
* Hair Loss
* Skin Rashes
* Sleep Issues
* A Hard Time With Concentration And Memory
* Depression, Anxiety, Or Mood Changes
If you have any of these, tell your doctor about it right away.
What You Can Do
The best way to avoid long COVID is to prevent COVID-19 infection.
You should wear a mask and maintain at least 6 feet of distance between yourself and other people when you’re in public. Wash your hands with soap or use alcohol-based sanitizer as often as you can and avoid going to crowded places.
When a COVID-19 vaccine becomes available to you, you should take it. If you have questions or concerns about the vaccine, talk with your doctor about it.
Why Impact of ‘Long Covid’ Could Outlast The Pandemic
Millions of people who have gotten Covid-19 and survived are finding that a full recovery can be frustratingly elusive. Weeks and months after seemingly recovering from even a mild case, many patients confront a wide range of health problems.
As researchers try to measure the durability and depth of what’s being called “long Covid,” a burgeoning number of specialized post–Covid clinics are opening to handle the patients. The scale of the pandemic means that Covid’s disabling effects — as well as economic pain and drain on health resources — could persist well after the contagion ends.
1. What Are The Ailments?
Data are emerging on the scope, frequency and duration of ailments — ranging from mildly annoying to incapacitating — that emerge or linger four weeks or more after a SARS-CoV-2 infection. Fatigue, shortness of breath, chest pain, cognitive disturbances including “brain fog,” and joint aches are commonly reported problems, often bad enough to affect quality of life.
Specific organ dysfunction also has been reported involving primarily the heart, lungs, and brain, even among those who had no noticeable symptoms during the acute phase. Most long Covid symptoms don’t seem to be life-threatening.
But a study of 1,250 patients in Michigan — who had been sick enough to be hospitalized — found 6.7% died within 60 days of discharge and 15.1% required re-admission, suggesting the effects can be serious for some.
2. How Prevalent Is It?
We don’t know yet because Covid-19 is a new disease. Risks may vary between hospitalized and non-hospitalized patients and be influenced by the severity of illness, age, gender, race, income, and underlying medical conditions.
Researchers haven’t studied enough patients over a long enough period of time to gauge the full range of long-term effects — what doctors call the post-acute sequelae, or PASC — what proportion of patients will suffer from them, or for how long. Early findings and the demand for specialized clinics to help survivors deal with scarred lungs, chronic heart damage, post-viral fatigue and other debilitating conditions indicate a significant prevalence.
3. What Are The Estimates?
The U.K.’s Office of National Statistics estimated in December that, among people who have tested positive for Covid-19, about 1 in 5 exhibit symptoms for five weeks or longer, and about 1 in 10 have symptoms for 12 weeks or longer.
As of November, before England experienced a severe winter surge, some 186,000 Covid survivors were living with symptoms that had persisted for 5 to 12 weeks, out of over 1 million known cases.
A small study from the University of Washington reported persistent symptoms for as long as nine months after an acute bout of Covid-19. A much larger study involving almost 240,000 Covid-19 patients found one in three received a neurological or psychiatric diagnosis within six months of infection.
4. Is Covid-19 Definitely To Blame For These Symptoms?
Not necessarily. One difficulty is figuring out which conditions are directly related to a past infection with SARS-CoV-2 and what might occur by chance or be triggered by pandemic-induced stress and anxiety.
A study of health-care workers at a Swedish hospital compared persistent symptoms among those who had recovered from mild Covid-19 at least 8 months before, and those who never caught the coronavirus.
Among those who’d been infected, 8% reported lingering symptoms causing moderate-to-marked disruptions of their work life, compared with 4% in the non-infected group.
Uncertainties about post-Covid illness have sometimes led to what so-called long haulers describe as medical gaslighting by health professionals who don’t take their complaints seriously, especially if the patient is a woman.
5. What Are The Broader Implications?
Some researchers say the pandemic may spur a raft of long-term problems, such chronic fatigue syndrome, also called myalgic encephalomyelitis or ME, dementia, Parkinson’s disease, diabetes and kidney impairment.
The reduced work hours reported in 68.9% of long-Covid patients indicate the pandemic is crimping labor productivity.
With 136 million Covid cases worldwide, even a small share with long-term debility could have enormous social and economic consequences. And these will be be magnified if people end up enduring years or decades of coronavirus-related disability.
6. Do Other Viruses Cause Prolonged Illness?
Yes. Post-viral syndromes occur after many viral infections, including the common cold, influenza, HIV, infectious mononucleosis, measles and hepatitis B.
Diabetes and other long-term consequences were observed in survivors of severe acute respiratory syndrome (SARS), which is caused by a related coronavirus.
A Canadian study found 21 health-care workers from Toronto had post-viral symptoms for as long as three years after catching SARS in 2003, and were unable to return to their usual work.
Some people who were hospitalized with SARS in Hong Kong still had impaired lung function two years later, a study of 55 patients published in 2010 found. Still, it’s not known yet whether the lessons of SARS are applicable to Covid-19.
7. What’s Being Done?
In the U.S., Congress is providing $1.15 billion in funding over four years for the National Institutes of Health to support research into the long-term effects of Covid-19. The series of studies hopes to answer key questions, such as:
* What Does The Spectrum Of Recovery Look Like Across All Age Groups, And What Proportion Experience Long-Term Problems?
* What Is The Underlying Biological Cause Of These Prolonged Symptoms, And How Might They Be Treated And Prevented?
* What Makes Certain People Vulnerable, While Others Recover Fully And Quickly?
* Does Sars-Cov-2 Infection Trigger Changes In The Body That Increase The Risk Of Chronic Disorders Affecting The Heart, Brain Or Other Organs?
How Long Do Covid-19 Vaccines Provide Immunity?
Pfizer, Moderna and Johnson & Johnson vaccines provide good protection against the virus that causes Covid. But how long does that last? Will you need a booster shot? Here’s what we know.
How long does protection from Covid vaccines last? It’s a question that’s becoming more important as some of the first people to be vaccinated approach four months post-inoculation.
The short answer is: We don’t fully know yet. But more data is coming in that provides clues. Here’s what we know so far.
How Long Are We Protected From Getting Covid-19? Does The Efficacy Decline Over Time?
Recent data from Pfizer, the manufacturer of one of the three vaccines available in the U.S., indicates that protection lasts at least six months. The results showed minimal antibody decline.
Recipients of the Moderna vaccine also had robust levels of antibodies more than six months later, according to a recent study published in NEJM.
Some people have incorrectly concluded that means that those vaccines offer only six months of protection, says Scott Hensley, a professor of microbiology at the University of Pennsylvania.
“That’s false,” says Dr. Hensley. “We only have six months of data…Six months from now it’s likely we’ll learn we have one year of protection.”
How Does Protection Provided By These Vaccines Work?
The vaccines will likely provide at least some degree of protection for a long time because there are so many layers of immunity, says Deepta Bhattacharya, an associate professor of immunobiology at the University of Arizona in Tucson.
The first shots of the two-shot Pfizer and Moderna vaccines provide reasonable protection. Then the second shot bumps up the level of antibodies and T cells produced by the body, he says.
T cells are white blood cells that destroy cells infected by viruses. There’s “a lot of room to decline and still be protected,” he says.
Will The Protection Provided By The Johnson & Johnson Vaccine Last As Long As Pfizer And Moderna’s?
Johnson & Johnson uses a different platform for its vaccine, and hasn’t been around long enough to have data out as far.
The level of antibodies in people who receive the Johnson & Johnson vaccine appears to keep increasing between two weeks and 70 days post-vaccination. So even though J&J’s reported efficacy is lower than Pfizer and Moderna’s, Dr. Bhattacharya says it may be similar at a later point in time.
Could The Vaccines Provide Lifelong Immunity?
It’s possible some level of protection could last for years or even decades, some scientists say, but we don’t know.
A 2020 Nature study found that patients who got SARS—a similar coronavirus to the one that causes Covid-19—still had T cell immunity 17 years later, says Monica Gandhi, an infectious disease physician and professor of medicine at the University of California, San Francisco.
Dr. Gandhi notes that even if antibody levels wane, there is evidence from a new preprint that memory B cells are generated by the Pfizer vaccine seven weeks after vaccination. Memory B cells are white blood cells that can be stimulated to produce new antibodies decades later.
A 2008 Nature study found that survivors of the 1918 influenza pandemic were able to produce antibodies from memory B cells when exposed to the same influenza strain nine decades later.
Will Emerging Variants Affect How Long Protection From Vaccines Lasts?
It’s hard to predict.
So far, the vaccines appear to provide good protection against most of the known variants. But as the virus continues to mutate, more problematic variants may emerge that are better able to skirt vaccine-induced defenses.
Such variants might already exist but just haven’t been sequenced and discovered, says Dr. Bhattacharya. “If they exist already, there will be selective pressure for these variants to increase in prevalence as we get closer to herd immunity,” he notes.
This is where antibody levels become very important, says Dr. Hensley. The mRNA vaccines elicit antibody levels that are generally higher than a natural infection.
Even if a variant prevents some antibodies from binding to the virus, the vaccines create so many antibodies that they should still offer some protection, says Dr. Hensley. But we don’t know how much, and for how long.
What Happens If A Variant Makes A Vaccine Less Effective?
The immune system is not all or nothing, notes Ann Sheehy, an immunologist and virologist at College of the Holy Cross in Worcester, Mass. It’s possible for a variant to reduce a vaccine’s protection but not entirely eliminate it.
If someone does get Covid-19 despite being vaccinated, the illness would likely be less severe. “The immune system is very clever. The second time you see something you often do better with it,” says Dr. Sheehy.
What About Boosters?
Drug companies are scrambling to test booster shots for some of the new variants.
Boosters will likely be needed for at least a few years “out of an abundance of caution, knowing that immunity does wane in some individuals more than others,” says David Topham, a professor of microbiology and immunology at the University of Rochester Medical Center.
Some experts say boosters may continue to be needed for longer, particularly if the virus changes a lot.
One big difference between the coronavirus that causes Covid-19 and the other seasonal coronaviruses like the one that causes the common cold is that the Covid-19 virus can replicate anywhere in the body.
The seasonal coronaviruses generally replicate only in the respiratory tract, says Dr. Topham. It’s unclear whether the Covid-19 virus may eventually become like the other common coronaviruses that cause only mild illness, or whether it will retain its ability to cause severe disease without annual booster doses.
I Had No Side Effects From My Second Vaccine. My Husband Did. Does That Mean He Has More Protection Than Me?
No. In general, scientists say side effects are a good thing. They are a signal that your immune system is at work, says Dr. Sheehy.
“Your immune system has been driven to know that you got exposed to something foreign,” says Dr. Sheehy. “If someone feels very ill they’ve generated a robust immune response.”
The converse is not true, however. “Just because you don’t feel sick does not mean you didn’t generate a robust immune response,” she says.
What About Protection From A Natural Infection?
The Centers for Disease Control and Prevention recommend getting the Covid-19 vaccine even if you’ve already had an infection. Evidence suggests that protection via natural infection can be strong but differs by person.
A Lancet Microbe study found that the immune response was variable with some people losing antibodies within three months and others having very high levels eight months later.
“I think in reality it’s going to vary from person to person,” says Dr. Topham. “Making a good initial immune response is key.”
Updated: 7-13-2021
Wellness Resorts Eye Long Covid Treatments As New Moneymaker
From colonic cleanses to brain modulation to nutrient-rich IV drips, spas are coming up with all sorts of (costly) ways to treat symptoms of long Covid.
To beat long Covid, the version of the virus where symptoms persist for more than 12 weeks, you can employ the same tried-and-true tactics that help overcome the flu: Stay well-rested, guzzle clear fluids, and hope for the best.
Or you can channel your inner Gwyneth Paltrow and pay $3,500 to have a therapist cake a paste of turmeric, galangal, and kaffir lime on your chest, cover it with an alcohol-doused towel, and set it all on fire.
The latter technique—a traditional Ya-Pao detoxification therapy used for centuries in Thailand—is believed to balance the wind, water, and fire elements in the body. According to the practitioners who prescribe it, it’s also a great way to alleviate long Covid symptoms such as inflammations and coughs.
Ya-Pao is just one of the treatments offered as part of the new Covid-19 Health Rejuvenating program at RAKxa, a medical spa resort just outside Bangkok with jungle-shrouded pool villas on an island in the Chao Phraya River.
And RAKxa is just one of at least a half-dozen acclaimed wellness resorts around the world aiming to capitalize on the medical aftermath of Covid.
Their addressable market is surprisingly large. While in-depth research on the prevalence of long Covid is still in its early stages, a recent study by the U.K.’s Office of National Statistics found that 13.7% of its 20,000 respondents, all of whom had tested positive for Covid-19, still felt symptoms after three months.
If this percentage is an indicator of the numbers elsewhere, more than 23 million people could be experiencing long Covid worldwide.
“We’re learning more about long Covid every day,” says Dr. Kristin Englund, an infectious disease specialist leading the long Covid recovery center at the Cleveland Clinic in Ohio. As the virus can affect almost every organ in the human body, she says, long Covid can present in many different ways.
Almost all of Englund’s patients experience fatigue, but other common symptoms include shortness of breath with exertion, dizziness, concentration difficulties, constipation, and intolerance to heat and cold.
More serious issues such as diabetes and kidney damage may, in some cases, prove deadly even months after the initial infection.
With long Covid manifesting itself in such a variety of forms, treating it is still a clinical conundrum. “If there is one consensus, it’s that there is no ‘magic pill’ for these patients,” Englund says.
“There is no supplement or antibiotic or treatment that will cure all symptoms. The best treatments are still to be determined.”
But the very absence of clear guidance from physicians has opened the opportunity for medical spas and wellness resorts to offer their own options, often with locally inspired or high-tech modalities that are either unproven in clinical settings or otherwise overlooked by Western medicine.
The question is less whether it’s worth trying these approaches and more whether people will shell out for it—many require weeklong commitments and hopping a flight halfway around the globe.
A Holistic Approach
At RAKxa, Medical Director Narinthorn Surasinthon—a regenerative medicine physician at Bangkok’s Bumrungrad Hospital—focuses on the respiratory system.
Over the three-day program, he and his team have patients inhale concentrated oxygen in a hyperbaric chamber, take intravenous blood ozone infusions, and practice chest muscle-strengthening exercises in an Olympic-grade medical gym. The goal is to restore lung capacity.
“Respiratory issues are some of the most common manifestations of long Covid,” Surasinthon explains, adding that “many people end up with scarring in their lungs.” Following the clinic’s holistic approach, he also includes Pranayama breathing exercises, acupuncture, and Thai traditional medicine—such as the fiery Ya-Pao therapy—to aid blood circulation and relieve discomfort.
The resort can tailor its therapies if patients have symptoms of a totally different nature and can draw on medical expertise from a partner hospital. “Pulmonologists, cardiologists, nephrologists, and rehabilitation doctors, we can all work together as a team,” Surasinthon says.
But other resorts are taking completely different approaches.
Perched on a hill on the Spanish coast between Málaga and Valencia, the SHA Wellness Clinic unveiled a seven-day Post-Covid program in May. After an initial assessment that includes a stress test, carotid ultrasound, and bloodwork, guests receive a program tailored to their ailments.
Those with musculoskeletal issues can get a combination of Watsu therapy (think underwater shiatsu massage) and reflexology. Those with psychological effects may receive a “brain photobiomodulation” session that claims to stimulate and regenerate brain cells with low-level lasers and coaching in Pranayama breathing.
And those with respiratory problems may try nebulization sessions (which are similar to asthma treatments) and traditional Chinese medicine. All of it is done within the plush confines of a sleek, white-on-white resort where the infinity pool faces a row of towering cliffs and the suites overlook the Balearic Sea.
Rates start at around $3,000, with required add-on treatment packages ranging from $650 to $1,300; accommodations are roughly an additional $400 a night.
“We’ve already seen a great deal of interest, both in definitive bookings and enquiries for more information,” says Juan Antonio García, SHA’s clinical director. Like the other resorts in this story, it didn’t offer numbers on how many people have booked.
Lanserhof Tegernsee, in the rolling Bavarian Alps just south of Munich, is a go-to spot for oligarchs and top models looking to detox, destress, or shed some pounds. Now its team of doctors and dieticians look at the gut for a possible long Covid cure.
Guests of its seven-day $10,000 Covid-19 Program will receive individual treatment schedules based on their symptoms (these could include bowel cleansing, energy therapy, lymphatic drainage treatments, and cryotherapy).
Every program is based on the strict diet plan of the late Austrian physician Dr. Franz Xaver Mayr, who’s famous for drawing attention to the importance of gut health. Using a combination of intermittent fasting, colonics, Epsom salts, and small portions of alkaline-rich food, the program aims to rid the gut of old debris to revitalize the immune system.
“Long Covid is a silent inflammation reaction,” says Dr. Benedetto-Reisch Lanserhof’s medical director. “Fasting has a regulating effect on those processes.”
Similar is the Post Covid program (seven days, from $7,000) at VIVAMayr, a small village of wooden chalets on the shore of Austria’s Lake Altaussee. It uses blood tests and applied kinesiology (muscle testing) to diagnose imbalances around the body and inform a personalized diet and treatment program.
But there the menu gets complemented by nutrient-rich IV drips, electrolysis foot baths, and breathing exercises to promote cell regeneration and increase the number of energy-producing mitochondria in patients’ cells.
A Proven Market
Although long Covid is a novel phenomenon, the isolated symptoms are not. Treatments for brain fog and respiratory problems have been a mainstay in wellness brochures for decades; they run the gamut from Ayurvedic methodologies to science-backed technical approaches.
This allowed wellness resorts to launch their Covid recovery programs relatively swiftly, without the need for new specialists or equipment. Lanserhof’s Covid recovery program made its debut in May 2020—even before “long Covid” was added to the dictionary.
That also means the resorts aren’t losing much by offering the programs, even if bookings are slim. But the demand exists, says Frances Geoghegan, founder and managing director of the London-based wellness travel agency Healing Holidays.
Since February, she says, she’s received as many as 50 weekly enquiries from people trying to address issues that have arisen as a result of Covid.
“They can’t get the help they need from their GP. [In the U.K.] it’s near impossible to get an appointment during the pandemic, and there are huge waitlists in place for treatments.” As a result, she explains, “Many have decided to take charge of their health and look for programs abroad.”
The combination of alternative and conventional medicine at wellness resorts is especially attractive to these consumers, Geoghegan says. “It’s a mixed bag of problems, and our clients are choosing to treat it in different ways.”
“It’s not just the medical treatments people are after,” says RAKxa’s Surasinthon, echoing Geoghegan’s sentiment. “They’re looking for a combination of everything. Healthy food, personal care, and exercise programs to aid rehabilitation—you won’t find that in a regular hospital.”
Are Latent Viruses Causing Long Covid-19 Symptoms? Patient Groups Push For Testing
A new theory that reactivated older viruses are driving some of the coronavirus’s debilitating symptoms is gaining traction among some patient advocates.
More long Covid-19 patients are pushing to investigate what they believe is fueling some of their debilitating long-term symptoms: dormant viruses that have been reactivated by the coronavirus.
An estimated 10% to 30% of all Covid-19 patients suffer from symptoms weeks and months after first getting the illness, including many young, previously healthy people whose initial Covid-19 cases were mild. Symptoms can include brain fog, fatigue, shortness of breath, racing heart beat and an inability to tolerate physical or mental exertion.
Public health officials around the world are trying to figure out exactly what is causing the symptoms; the National Institutes of Health earlier this year unveiled a major initiative to study long Covid-19, backed by $1.15 billion in funding. Yet scientists still know very little about the causes of the condition, and have even fewer treatments to offer.
Most people—whether they have had Covid-19 or not—have dormant, normally harmless viruses in their body that they contracted years earlier.
Among the most common are the herpes family of viruses. That includes the Epstein-Barr virus (EBV), which causes mononucleosis, as well as human herpesvirus 6 (HHV-6), which causes the common childhood illness sixth disease, the herpes simplex viruses, and herpes zoster, a reactivation of the chickenpox virus that can cause shingles.
Such viruses can be reactivated at times by stress, including infections.
Some long Covid-19 patients and advocacy groups are urging doctors to test more regularly for reactivated viruses. With so few treatment options for long Covid-19, they say, it makes sense to see if a herpes antiviral drug might relieve symptoms.
Some doctors say it is worth more testing and further study. Others say the tests are difficult to interpret—and that even if a latent virus does reactivate, it is unclear whether that is causing long Covid-19 symptoms.
In June, a study published in the medical journal Pathogens suggested a possible association between Epstein-Barr reactivations and long Covid-19. In a set of 30 long Covid-19 patients, about 67% were positive for EBV reactivation, researchers found.
That compared with about 10% of the control group, who had contracted Covid-19 but didn’t experience long-term symptoms. The researchers tested for reactivation based on the levels of two antibodies they say are associated with active or reactivated EBV infection.
David Hurley, a molecular microbiologist who studies EBV reactivation and was a co-author on the study, says latent EBV can be reactivated by stress.
Some people experience fatigue, brain fog and other symptoms that are also commonly reported by long Covid patients, says Dr. Hurley. For some people, symptoms last only a few days, but for others they can last months or longer, he adds.
A normal, healthy immune system can keep latent viruses under control. But a Covid-19 infection “provides an opportunity to lose that control,” says Amy Proal, a microbiologist at PolyBio Research Foundation, who was first author in a recent review article in the journal Frontiers in Microbiology examining how reactivated viruses might be contributing to long Covid-19 symptoms.
Doctors aren’t routinely testing for reactivated herpes viruses in long Covid-19 patients. Commercially available lab tests covered by insurance and available to most patients aren’t as sophisticated as the ones researchers use to test for viral DNA, so they aren’t likely to pick up as many reactivations, says Susan Levine, a doctor at the Center for Solutions for ME/CFS at Columbia University’s Mailman School of Public Health and the Cornell Center for Enervating NeuroImmune Disease.
Dr. Levine says she treats about 200 long Covid-19 patients and does test for reactivated viruses, but often uses additional tests to confirm a diagnosis. She says about 80% have evidence of reactivated EBV, with a smaller percentage also testing positive for a reactivated case of HHV-6.
Dr. Levine says it is difficult to determine how much the reactivation of viruses is contributing to long Covid-19 patients’ continuing symptoms, but she believes they are playing a significant role.
Lauren Nichols is a 33-year-old Boston resident and volunteer executive board member of Body Politic, which has a Covid-19 support group on Slack with more than 17,000 members. The group is pushing for more aggressive testing of reactivated viruses.
Mrs. Nichols got Covid-19 in March 2020 and says she has experienced long-term symptoms, including fatigue and brain fog. In September, lab tests showed high levels of EBV, she says, and she started taking an antiviral medication commonly used to treat herpes infections. She believes it has helped relieve her fatigue and brain fog.
“There’s no treatment for long Covid, but there are treatments for these viral diseases that are being reactivated in some of us,” says Mrs. Nichols. “Right now it’s really about symptom management to allow us to be more functional.”
The potential role of reactivated viruses is worth studying, says Timothy Henrich, an associate professor of medicine at the University of California San Francisco who is part of a study following long Covid-19 patients there. “We’re planning on incorporating this into our study,” says Dr. Henrich.
That latent viruses are reactivated by a Covid-19 infection isn’t surprising, says Dr. Henrich. The question is whether that reactivation is causing long Covid-19 symptoms, he says.
Reactivated viruses in immunocompromised patients can cause symptoms and disease that can be treated, says Dr. Henrich. But many people may have transient but detectable levels of human herpes virus that don’t cause symptoms.
The role of EBV in myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) has been a continuing debate in the medical community. Some studies have shown EBV reactivation in such patients, but that doesn’t necessarily prove the reactivation is causing the symptoms, notes Dr. Henrich.
Benjamin Abramoff, an assistant professor of physical medicine and rehabilitation at the University of Pennsylvania who sees patients at the Post-Covid Assessment and Recovery Clinic there, says that while patient groups and patients sometimes bring up the reactivation issue, they don’t test patients for it.
“Given that these are seen in other disease processes, we do not think this is likely the driver of long-term symptoms,” says Dr. Abramoff.
Patrick Smith, a 37-year-old investment consultant in Denver, tested positive for Covid-19 in April this year. He was hospitalized with severe pneumonia for four days. He has continued to experience longer-term symptoms, including brain fog and fatigue.
He has been to three long Covid-19 clinics at hospitals, and saw an integrated-medicine doctor in Boulder. That doctor, Pierre Brunschwig, tested him for reactivated EBV and HHV-6, and says the tests indicated reactivation.
Dr. Brunschwig says he is testing all the long Covid-19 patients he sees for reactivated herpes viruses. “The immune system is depleted and distracted. It’s a window of opportunity to reactivate,” he says.
He treats patients with supplements, such as high-dose vitamin C and zinc, as well as antivirals but says the antivirals don’t always work. “Is that because we don’t have the treatment right, or it’s not an important contribution to the patient’s suffering?” he says. “It’s always a possibility that the labs are not definitive.”
Mr. Smith recently started taking the antiviral used to treat herpes infections, which he thinks has helped his fatigue and brain fog. “It’s a night and day difference,” he says.
Updated: 7-25-2021
What The U.S. Can Learn From The U.K.’s Response To Long Covid
Fragmented data is key hurdle for scientists studying illness.
While the U.K. races ahead treating patients suffering from the long-term effects of Covid-19, the U.S. is falling behind as a result of its decentralized health care system.
“Long Covid” — which surfaced after the first wave in spring 2020 — is estimated to afflict nearly a quarter of all patients, with symptoms such as chronic fatigue, muscle aches and brain fog persisting for weeks or even months.
Absent national oversight, U.S. scientists studying and treating the post-viral syndrome have been operating in silos. Hospital systems, clinics and insurers have inconsistent patient records, which poses a daunting task for those trying to find data on long Covid, much less draw conclusions from it.
Clinicians have developed treatments largely in isolation, and while 42 states have at least one long Covid clinic, those are primarily concentrated in urban areas.
Not until June did the U.S. Centers for Disease Control and Prevention issue guidance on long Covid, and though national studies are finally underway, standardized treatment won’t come soon.
The U.K., meanwhile, has been collecting data and standardizing treatment since late 2020, setting up 83 long Covid clinics that use the same guidelines for care.
Building on the country’s previous efforts, which include prevalence estimates and studies targeting hospitalizations after acute Covid, the U.K.’s National Institute for Health Research said Sunday that $27.5 million will go to 15 studies analyzing the causes and physical and mental impacts of the syndrome.
Though the U.S. has dramatically decreased the rate of acute infections, the country’s total case count — the world’s highest at more than 34 million infections reported — means millions are likely to have suffered or to still be suffering from long Covid.
As the delta variant spreads and pockets of the U.S. resist vaccination, the death rate and number of long Covid cases are lagging indicators of the nation’s record fighting the pandemic.
“We’re worried right now about the acute phase, and we figure we’ll deal with the chronic thing later,” said Michael Kinch, associate vice chancellor at Washington University in St. Louis, who as a scientist himself helped develop drugs. “But how many people could potentially be losing out because we’re taking this approach?”
Messy Data
An estimated 3.2 million people in the U.K., or 6.2% of its adult population, are experiencing long Covid symptoms that are adversely affecting their daily life, according to the latest self-reported survey from the nation’s Office of National Statistics.
No such prevalence estimates have been released in the U.S., where data collection and resource distribution is far more fragmented.
Clinics each have their own systems for collecting patient information, so some researchers are relying on insurance databases to find facts on so-called Covid long-haulers. Even that’s not a perfect fix: Without a billing code specifically for long Covid, researchers have to wade through records in search of relevant data.
“Our clinic collects certain information which somewhat overlaps with other clinics, but everyone does things a little differently, which makes combining the data more challenging,” said John Baratta, co-director of the long Covid clinic at the University of North Carolina at Chapel Hill.
Charlotte Summers, chief investigator of the U.K.’s national HEAL-COVID clinical trial, works directly with the hospital system and the Institute for Health Research to study and treat patients experiencing severe symptoms in the weeks after Covid-related hospitalizations. She said the U.K.’s linked health care and research infrastructures have been critical to progress.
“It’s been absolutely key to delivering vaccine trials, therapy trials and everything else,” she said. “They’ve diverted resources and made sure barriers go away.”
Efforts to standardize Covid patient data in the U.S. and beyond are underway. The World Health Organization is working to launch an ICD-10 diagnostic code for long Covid in October, which will make it easier for researchers to study health records.
Last September, the U.S.’s National Institutes of Health launched the National Covid Cohort Collaborative, or N3C, which is now one of the biggest repositories for Covid records in the world. Still, it falls on N3C’s technicians to standardize data.
Christopher Chute, co-lead of the N3C at Johns Hopkins Bloomberg School of Public Health in Baltimore, said that machine learning has helped find about 1,000 patients who they are confident have long Covid — out of 6.5 million in the data.
He said that while the U.K. has many more patient records available, most are less detailed than the information that N3C collects.
“They can’t do the integrated work we’re doing in N3C,” he said. “We have a much smaller patient population, but their data on average is much more shallow.”
Prioritizing Treatment
Alba Azola, co-director of physical medicine and rehabilitation at Johns Hopkins’s post-acute Covid clinic, has been treating long-haulers since April 2020.
Last month, her colleagues on the Covid research team approached her and the other directors about creating a long Covid clinic. They were unaware that one already existed.
“It was really awkward, actually,” she said. “Communication between institutions, and even within the same institution, has been very fragmented.”
In order to stay informed on the latest research, Azola has weekly meetings with her long Covid clinic team, as well as autonomic dysfunction experts to discuss recent national and international findings.
Twice a month, she spends her evenings in video calls with members of the Academy of Physical Medicine and Rehabilitation, talking about assessing and managing long Covid symptoms.
She also said that monitoring “long Covid Twitter” helps find studies as they’re published.
“I’m exhausted just thinking about it,” she said. “It’s scary if you’re a family doctor in the middle of a rural area — you’re not in a position to attend all these meetings and read all these papers to stay on top of it.”
National studies on long Covid are now underway in the U.S., using $1.15 billion in funding that Congress earmarked for the research in December 2020. In May, the National Institutes of Health selected three institutions to lead trials, involving dozens of researchers across the country and some 20,000 participants.
Andrea Troxel, co-principal investigator of the New York University Langone Health team that the agency selected, said the initiative will be critical for finding markers of long Covid, which are difficult to identify.
“That has to be done really intentionally, because we live in a system that doesn’t automatically support it,” she said.
Still, Troxel said, it could be another year before the first round of findings. The second phase of the studies will focus on finding therapies.
U.K. researcher Summers said treating the hundreds of thousands patients affected should take precedence.
“You can either wait and decide that you know absolutely everything about it, and let thousands of more people potentially be harmed, or say, we think we know enough now and there’s equipoise around certain therapies, so we should start randomizing people,” she said.
Updated: 10-21-2021
Sniffing Essential Oils Can Help Covid Patients Regain Their Sense Of Smell
RICHMOND, Va. — A new study reveals those who sniff essential oils are more likely to get their sense of smell and taste back after contracting COVID-19, especially if they’re under 40 years-old. According to researchers, the common COVID symptom usually lasts up to six months for four out of every five patients.
The study also shows that younger coronavirus patients are more likely to recover these senses than older people. In an ongoing COVID smell and taste loss survey, collecting data from 798 survivors, researchers from the Virginia Commonwealth University (VCU) found that participants younger than 40 recovered their senses at a higher rate than older adults.
“With our cohort, we did see about an 80% recovery rate in a six-month period or longer. However, 20% is still a lot of people, given the millions that have been afflicted with COVID-19,” says Professor Evan Reiter, the medical director of the Smell and Taste Disorders Center at VCU Health and one of the co-investigators of the study, in a university release.
Pre-Existing Conditions Can Make Things Worse
The professor, who works in the Department of Otolaryngology-Head and Neck Surgery at the VCU School of Medicine, adds that understanding the different types of symptoms and whether the patients suffer from any pre-existing medical conditions can provide critical insights into their recovery prognosis.
Those with a history of head injuries were less likely to recover their sense of smell. Additionally, those who experienced shortness of breath while combating the virus were even less likely to recover their senses quickly.
However, those dealing with nasal congestion were more likely to regain their sense of smell.
“Increased likelihood of recovering smell in subjects with nasal congestion stands to reason simply because you can lose your sense of smell because you’re badly congested and odors can’t get into your nose.
Certainly, a subset of those people who are congested might have just lost their sense of smell because they were badly congested, rather than because of nerve damage due to the virus, as in other cases,” Prof. Reiter explains.
According to the World Health Organization, there have been more than 230 million cases of COVID-19 worldwide. If the survey reflects populations worldwide, more than 20 million people could suffer from a lingering loss of smell or taste after their COVID diagnosis.
Since April 2020, when reports of patients losing their senses of taste and smell started becoming common, researchers at VCU have been working hard to determine how long the symptoms would last in order to identify treatments for those who have lost the use of their senses.
Losing The Sense Of Smell Lowers Quality Of Life
To date, nearly 3,000 people across the U.S. have participated in the survey, which works by tracking symptoms over time. Results have proved that sensory loss can be devastating for those who experience it.
In a previous survey published in April 2021, 43 percent of participants reported that they felt depressed and 56 percent had decreased enjoyment in life while experiencing a loss of smell or taste.
Unsurprisingly, those who had lost their sense of smell or taste found it difficult to enjoy food, with 87 percent of participants indicating that cooking and eating had become a quality-of-life concern.
The inability to smell smoke ranked as the most common safety risk, with nearly half of all patients reporting this problem.
“An inability to smell smoke was the most common safety risk, reported by 45% of those surveyed. Loss of appetite [present in 55% of sufferers] and unintentional weight loss [in 37%] continue to pose challenges for patients.
The more we learn from those who’ve been affected, the better we can advise their health care providers and even individuals themselves on how to manage those symptoms.
Through this study, we continue to gain a clearer picture of the risks COVID-19 poses to quality of life, safety, and long-term health and well-being while seeking answers on treatment,” says Dr. Daniel Coelho, the study’s lead author.
How Can Essential Oils Help?
According to scientists, smell training using potent essential oils may help recover the lost senses.
“I continue to recommend that to my patients. It’s low cost and low risk,” Prof. Reiter says.
The Clinical Olfactory Working Group, made up of an international group of physicians with a strong research interest in the sense of smell, recommended essential oils as a treatment option earlier this year.
The group found that when a person loses their sense of smell (olfactory dysfunction), smelling essential oils could help foster the recovery of the damaged nerves.
“I’d also say potentially it may get people a little bit more tuned into whatever level of function they have left so it might make them more sensitive and better able to use the remaining sensors and neurons that are working,” Reiter adds.
For those who may be concerned about losing their senses, Prof. Reiter confirmed that the best possible prevention method would be to start sniffing essential oils.
“What the CDC and WHO have been saying — get vaccinated, wear a mask, hand hygiene — all of the seemingly simple things that are readily available at least here in the United States, fortunately, are important.
To prevent these long-term consequences, you really need to minimize your chances of getting the disease in the first place because, once it hits, we just right now don’t really have a way to affect its course or affect its severity. Prevention is worth a thousand pounds of cure, in this case, because the cure isn’t there,” the professor concludes.
Can An Implant Restore Your Ability To Smell?
However, there is even more hope, as Dr. Coelho, along with his colleague from the study, Dr. Richard Costanzo, a Professor in the Department of Physiology and Biophysics at VCU, has been developing an implant device to restore people’s sense of smell.
The pair are optimistic that when it’s operational, it could be a source of hope for those living with a lasting loss of smell.
The findings appear in the American Journal of Otolaryngology.
Updated: 1-17-2022
Genetic Risk Factor Found For Covid-19 Smell And Taste Loss, Researchers Say
Six months after contracting Covid, as many as 1.6 million people in the U.S. are still unable to smell or have experienced changes in their ability to smell.
Scientists are piecing together why some people lose their sense of smell after contracting Covid-19.
A study published Monday in the journal Nature Genetics identified a genetic risk factor associated with the loss of smell after a Covid infection, a discovery that brings experts closer to understanding the perplexing pattern and may point the way toward much-needed treatments.
Six months after contracting Covid, as many as 1.6 million people in the United States are still unable to smell or have experienced a change in their ability to smell.
The precise cause of sensory loss related to Covid is not known, but scientists do think it stems from damage to infected cells in a part of the nose called the olfactory epithelium. These cells protect olfactory neurons, which help humans smell.
“How we get from infection to smell loss remains unclear,” said Dr. Justin Turner, an associate professor of otolaryngology at Vanderbilt University who was not a part of the study.
“Early data suggests that supporting cells of the olfactory epithelium are the ones mostly being infected by the virus, and presumably this leads to the death of the neurons themselves,” he said. “But we don’t really, really know why and when that happens, and why it seems to preferentially happen in certain individuals.”
A genetic locus near two olfactory genes is associated with Covid-induced loss of smell and taste, according to the study. A locus is the fixed position of a gene on a chromosome.
This genetic risk factor increases the likelihood a person infected with SARS-CoV-2 will experience a loss of smell or taste by 11 percent. While some estimates suggest 4 out of 5 Covid patients regain these senses, research suggests the persistent inability or reduced ability to smell and taste impacts relationships, physical health and psychological well-being.
Researchers at the genomics and biotechnology company 23andMe conducted the study as part of a larger Covid project. All participants live in the U.S. or the United Kingdom.
Within a group of 69,841 individuals who self-reported receiving a positive Covid test, 68 percent reported a loss of smell or taste as a symptom. The loss of smell and taste were combined as a single survey question; this grouping and the use of self-reported data are limitations of the study.
After comparing the genetic differences between those who lost their sense of smell and those who reported that they did not suffer this effect, the study team found a region of the genome associated with this split that’s situated near two genes, UGT2A1 and UGT2A2.
Both of these genes are expressed within tissue inside the nose involved in smell and play a role in metabolizing odorants.
“It was this really beautiful example of science where, starting with a large body of activated research participants who have done this 23andMe test, we were able to very quickly gain some biological insights into this disease that would otherwise be very, very difficult to do,” said Adam Auton, vice president of human genetics at 23andMe and the lead author of the study.
How UGT2A1 and UGT2A2 are involved in this process is unclear, though he and his colleagues hypothesize the genes “may play a role in the physiology of infected cells” and the resulting impairment that leads to smell loss.
To use these findings, scientists need to learn more about how these genes are expressed and what their functions are in olfactory signaling, Turner said.
Certain trends also emerged among the participants who reported the loss of smell and taste: Women, for example, were 11 percent more likely than men to experience this. Meanwhile, adults between the ages of 26 and 35 made up 73 percent of this group.
The study team also found people of “East Asian or African American ancestry were significantly less likely to report loss of smell or taste.” The cause of this observation is not yet known, but Auton said it’s likely not explained by the genetic variants of this specific locus.
The team also notes the study is biased toward people of European ancestry because of limited reference data.
These findings can help patients in two ways, said Danielle Reed, associate director of the Monell Chemical Senses Center. She studies person-to-person differences in the loss of smell and taste due to Covid and was not a part of the new paper.
First, “it helps answer the question of ‘why me’ when it comes to taste and smell loss with Covid-19,” she said. “Some people have it and some do not. Inborn genetics may partially explain why.”
The study may also help scientists find treatments. Earlier research suggests the loss of these senses is related to a “failure to protect the sensory cells of the nose and tongue from viral infection,” Reed said.
“This study suggests a different direction,” she said. “The pathways that break down the chemicals that cause taste and smell in the first place might be over or underactive, reducing or distorting the ability to taste and smell.”
For most of the coronavirus pandemic, the loss of smell and taste have been known as signature symptoms. Early research suggests loss of smell and taste is rarer with the omicron variant, but not entirely unlikely: In a study of 81 omicron cases in Norway, 12 percent reported reduced smell and 23 reported reduced taste.
Updated: 1-26-2022
Scientists Identify Factors That Appear Linked To Long Covid
Scientists seeking to find out which patients are most at risk of developing long Covid offered partial answers in a study.
People who have circulating fragments of the coronavirus, specific antibodies directed against their own tissues or organs — known as auto-antibodies — and a resurgence of the Epstein-Barr virus appear more at risk, researchers said in an article in the scientific journal Cell.
Scientists are racing to better understand and predict long Covid, in which patients still confront a wide range of health problems months after recovery.
The team of more than 50 researchers found some markers that could be identified early and appeared to correlate with lasting symptoms, regardless of whether the initial infection was severe.
The researchers followed 309 Covid patients from initial diagnosis to convalescence two or three months later and compared them to healthy control subjects. They analyzed blood samples and nasal swabs, integrating the data with patients’ health records and self-reported symptoms.
After three months, more than half of patients reported fatigue and a quarter reported a lingering cough. Others suffered gastro-intestinal symptoms.
The study results were complex, with different profiles associated with different symptoms. Overall, the scientists pointed to a reactivation of the Epstein-Barr virus — which usually remains dormant in the body — and circulating fragments of SARS-CoV-2 at diagnosis as factors that could anticipate long Covid.
So did a handful of auto-antibodies, including some associated with lupus. They also found that patients with respiratory symptoms had low levels of the hormone cortisol.
The researchers found a correlation between type 2 diabetes and cough; that women tended to suffer neurological symptoms; and that patients with heart disease or pre-existing cough tended to experience loss of smell or taste.
The authors said their findings pointed to potential treatment strategies that include antiviral medicines, since they have an effect on viral load, and cortisol-replacement therapy, for patients who are deficient.
Updated: 1-28-2022
Lung Abnormalities Found In Long Covid Patients With Breathing Issues
Researchers have discovered abnormalities in the lungs of long Covid patients who have breathlessness which cannot be detected with routine tests.
The Explain study uses xenon, an odourless, colourless, tasteless and chemically non-reactive gas, to investigate possible lung damage in the patients who have not been admitted to hospital, but continue to experience the symptom.
The initial results of the study suggest there is significantly impaired gas transfer from the lungs to the bloodstream in the long Covid patients despite other tests – including CT scans – coming back as normal.
The study’s chief investigator, Fergus Gleeson, professor of radiology at the University of Oxford and consultant radiologist at Oxford University Hospitals NHS Foundation Trust, said: “We knew from our post-hospital Covid study that xenon could detect abnormalities when the CT scan and other lung function tests are normal.”
“What we’ve found now is that, even though their CT scans are normal, the xenon MRI scans have detected similar abnormalities in patients with long Covid.”
“These patients have never been in hospital and did not have an acute severe illness when they had their Covid-19 infection.”
“Some of them have been experiencing their symptoms for a year after contracting Covid-19.”
“There are now important questions to answer. Such as, how many patients with long Covid will have abnormal scans, the significance of the abnormality we’ve detected, the cause of the abnormality, and its longer-term consequences.”
“Once we understand the mechanisms driving these symptoms, we will be better placed to develop more effective treatments.”
In the study, the patients were required to lie in an MRI scanner and breathe in one litre of the gas that has been tweaked so that it can be seen using MRI.
Because xenon, which is safe to inhale, behaves in a very similar way to oxygen, radiologists can observe how it moves from the lungs into the bloodstream.
The scan takes just a few minutes and, as it does not require radiation exposure, can be repeated over time to see changes to the lungs.
While the full Explain study will recruit about 400 participants, the initial pilot had 36 participants making up three groups.
This included those diagnosed with long Covid who had been to long Covid clinics and who had normal CT scans, and people who had been in hospital with coronavirus and discharged more than three months ago, who had normal or nearly normal CT scans and who were not experiencing long Covid.
The third group was an age and gender-matched control group who did not have long Covid symptoms and were not admitted to hospital with the virus.
Dr Emily Fraser, respiratory consultant who leads the Oxford Post-Covid Assessment Clinic, said: “These are interesting results and may indicate that the changes observed within the lungs of some patients with long Covid contribute to breathlessness.
“However, these are early findings and further work to understand the clinical significance is key.”
Asked what people suffering from the symptom can take from the findings, she added: “I think that the message should be that we are actively researching what is driving long Covid.”
But Dr Fraser also said people should not give up on the current exercises and rehab they are working on, as this is also helpful.
The method and clinical applications were developed by Professor Jim Wild and the Pulmonary, Lung and Respiratory Imaging Sheffield (Polaris) research group at the University of Sheffield.
Prof Wild said: “Xenon follows the pathway of oxygen when it is taken up by the lungs and can tell us where the abnormality lies between the airways, gas exchange membranes and capillaries in the lungs.”
The study, which received Government funding, is supported by the NIHR Oxford Biomedical Research Centre (BRC).
The findings, which have not been peer-reviewed, were posted on the bioRxiv pre-print server.
Updated: 1-30-2022
Fears Mount Of Coming Wave Of Long Covid From Omicron Infections
More than a year after a bout with COVID-19, Rebekah Hogan still suffers from severe brain fog, pain and fatigue that leave her unable to do her nursing job or handle household activities.
Long COVID has her questioning her worth as a wife and mother.
“Is this permanent? Is this the new norm?’’ said the 41 -year-old Latham, New York, woman, whose three children and husband also have signs of the condition. “I want my life back.’’
More than a third of COVID-19 survivors by some estimates will develop such lingering problems. Now, with omicron sweeping across the globe, scientists are racing to pinpoint the cause of the bedeviling condition and find treatments before a potential explosion in long COVID cases.
Could it be an autoimmune disorder? That could help explain why long COVID-19 disproportionately affects women, who are more likely than men to develop autoimmune diseases. Could microclots be the cause of symptoms ranging from memory lapses to discolored toes? That could make sense, since abnormal blood clotting can occur in COVID-19.
As these theories and others are tested, there is fresh evidence that vaccination may reduce the chances of developing long COVID.
It’s too soon to know whether people infected with the highly contagious omicron variant will develop the mysterious constellation of symptoms, usually diagnosed many weeks after the initial illness. But some experts think a wave of long COVID is likely and say doctors need to be prepared for it.
With $1 billion from Congress, the National Institutes of Health is funding a vast array of research on the condition. And clinics devoted to studying and treating it are popping up around the world, affiliated with places such as Stanford University in California and University College London.
Why Does It Happen?
Momentum is building around a few key theories.
One is that the infection or remnants of the virus persist past the initial illness, triggering inflammation that leads to long COVID.
Another is that latent viruses in the body, such as the Epstein-Barr virus that causes mononucleosis, are reactivated. A recent study in the journal Cell pointed to Epstein-Barr in the blood as one of four possible risk factors, which also include pre-existing Type 2 diabetes and the levels of coronavirus RNA and certain antibodies in the blood. Those findings must be confirmed with more research.
A third theory is that autoimmune responses develop after acute COVID-19.
In a normal immune response, viral infections activate antibodies that fight invading virus proteins. But sometimes in the aftermath, antibodies remain revved up and mistakenly attack normal cells. That phenomenon is thought to play a role in autoimmune diseases such as lupus and multiple sclerosis.
Justyna Fert-Bober and Dr. Susan Cheng were among researchers at Cedars-Sinai Medical Center in Los Angeles who found that some people who have had COVID-19, including cases without symptoms, have a variety of these elevated “autoantibodies” up to six months after recovering. Some are the same ones found in people with autoimmune diseases.
Another possibility is that tiny clots play a role in long COVID. Many COVID-19 patients develop elevated levels of inflammatory molecules that promote abnormal clotting.
That can lead to blood clots throughout the body that can cause strokes, heart attacks and dangerous blockages in the legs and arms.
In her lab at Stellenbosch University in South Africa, scientist Resia Pretorius has found microclots in blood samples from patients with COVID-19 and in those who later developed long COVID. She also found elevated levels of proteins in blood plasma that prevented the normal breakdown of these clots.
She believes that these clotting abnormalities persist in many patients after an initial coronavirus infection and that they reduce oxygen distribution to cells and tissue throughout the body, leading to most if not all symptoms that have been linked to long COVID.
It Can Hit Nearly Anyone
While there’s no firm list of symptoms that define the condition, the most common include fatigue, problems with memory and thinking, loss of taste and smell, shortness of breath, insomnia, anxiety and depression.
Some of these symptoms may first appear during an initial infection but linger or recur a month or more later. Or new ones may develop, lasting for weeks, months or over a year.
Long COVID affects adults of all ages as well as children. Research shows it is more prevalent among those who were hospitalized, but also strikes a significant portion who weren’t.
Retired flight attendant Jacki Graham’s bout with COVID-19 at the beginning of the pandemic wasn’t bad enough to put her in the hospital. But months later, she experienced breathlessness and a racing heart. She couldn’t taste or smell. Her blood pressure shot up.
In the fall of 2020, she became so fatigued that her morning yoga would send her back to bed.
“I’m an early riser, so I’d get up and push myself, but then I was done for the day,” said Graham, 64, of Studio City, California. “Six months ago, I would have told you COVID has ruined my life.”
Hogan, the New York nurse, also wasn’t hospitalized with COVID-19 but has been debilitated since her diagnosis. Her husband, a disabled veteran, and children ages 9, 13 and 15 fell ill soon after and were sick with fever, stomach pains and weakness for about a month. Then all seemed to get a little better until new symptoms appeared.
Hogan’s doctors think autoimmune abnormalities and a pre-existing connective tissue disorder that causes joint pain may have made her prone to developing the condition.
Potential Answers
There are no treatments specifically approved for long COVID, though some patients get relief from painkillers, drugs used for other conditions, and physical therapy. But more help may be on the horizon.
Immunobiologist Akiko Iwasaki is studying the tantalizing possibility that COVID-19 vaccination might reduce long COVID symptoms.
Her team at Yale University is collaborating with a patient group called Survivor Corps on a study that involves vaccinating previously unvaccinated long COVID patients as a possible treatment.
Iwasaki, who is also an investigator with the Howard Hughes Medical Institute, which supports The Associated Press’ Health and Science Department, said she is doing this study because patient groups have reported improvement in some people’s long COVID symptoms after they got their shots.
Study participant Nancy Rose, 67, of Port Jefferson, New York, said many of her symptoms waned after she got vaccinated, though she still has bouts of fatigue and memory loss.
Two recently released studies, one from the U.S. and one from Israel, offer preliminary evidence that being vaccinated before getting COVID-19 could help prevent the lingering illness or at least reduce its severity. Both were done before omicron emerged.
Neither has been published in a peer-reviewed journal, but outside experts say the results are encouraging.
In the Israeli study, about two-thirds of participants received one or two Pfizer shots; the others were unvaccinated. Those who had received two shots were at least half as likely to report fatigue, headache, muscle weakness or pain and other common long COVID symptoms as the unvaccinated group.
Uncertain Future
With few clear answers yet, the future is murky for patients.
Many, like Graham, see improvement over time. She sought help through a long COVID program at Cedars-Sinai, enrolled in a study there in April 2021, and was vaccinated and boosted.
Today, she said, her blood pressure is normal, and her sense of smell and energy level are getting closer to pre-COVID levels. Still, she wound up retiring early because of her ordeal.
Hogan still struggles with symptoms that include agonizing nerve pain and “spaghetti legs,’’ or limbs that suddenly become limp and unable to bear weight, a condition that also affects her 13-year-old son.
Some scientists worry that long COVID in certain patients might become a form of chronic fatigue syndrome, a poorly understood, long-lasting condition that has no cure or approved treatment.
One thing’s for sure, some experts say: Long COVID will have a huge effect on individuals, health care systems and economies around the world, costing many billions of dollars.
Even with insurance, patients can be out thousands of dollars at a time when they’re too sick to work. Graham, for example, said she paid about $6,000 out of pocket for things like scans, labs, doctor visits and chiropractic care.
Pretorius, the scientist in South Africa, said there is real worry things could get worse.
“So many people are losing their livelihoods, their homes. They can’t work anymore,” she said. “Long COVID will probably have a more severe impact on our economy than acute COVID.”
Updated: 3-16-2022
Long Covid Could Reveal Clues To Alzheimer’s, Lyme Disease
Congress should approve more pandemic money, especially for studying lingering effects. What scientists learn could help millions.
Last week, the U.S. Congress failed to approve $15 billion needed to continue Covid-19 precautions, even though today’s low case counts are likely to rise, as they are in Europe, with the sub-variant called BA.2.
We’ve learned that some expensive mitigation measures, such as deep cleaning, are a waste of money, and could be scrapped, but funding for studying Covid should increase — not just for prevention measures and vaccines, but for research into the long-term consequences of infection.
Some people who got Covid-19 early in the pandemic still haven’t recovered, and what looked like “long Covid” might, for some people, be a permanent condition if no treatment is found. The lingering symptoms are often different from those associated with acute infection.
Patients report changes in memory, trouble thinking clearly or concentrating, mood disorders, sleep disturbances, changes in balance and gastrointestinal problems. Some have a form of fatigue that can get much worse with physical or mental exertion.
The good news is that some of the country’s top medical researchers have jumped on this problem and are gaining momentum. What they learn is likely to apply to other medical problems.
Take the work of Mark Albers, a neurologist at Massachusetts General Hospital who had been uncovering the weird relationship between loss of sense of smell and Alzheimer’s Disease. Now he’s expanded his research to learn about similar changes in Covid-19 patients.
A few years back Albers developed a test of what he calls smell memory, which was connected to the earliest stages of Alzheimer’s disease. Smell, he told me, is the one sense that’s physiologically connected directly to our brain’s memory center, so smell changes are often the first clue something is wrong.
Now he’s also studying patients who have persistent loss of their olfactory sense after a Covid infection — something that can drag on for months or, worse, return in a distorted way so that food smells like rotting fish or garbage.
A recent brain scanning study showed that people who had tested positive showed tiny but statistically significant changes in the brain regions that govern smell, which Albers says suggests that Covid could lead to inflammation of this part of the brain — the same part that’s associated with early Alzheimer’s disease.
In studies in animals, he’s found that viral infection in the nose doesn’t directly infiltrate the brain, but the inflammation caused by a respiratory infection can.
Scientists have already found connections between other infectious agents and Alzheimer’s disease — including herpes simplex virus and the bacteria implicated in gum disease. These might not be the root causes of dementia but they could exacerbate the disease’s progression.
The brain imaging study shouldn’t be interpreted to mean that Covid-19 causes dementia. The changes measured were minuscule and not linked to any lingering symptoms, and there’s a certain expected natural fluctuation in people’s brain images.
Still, Albers said he’d like to see more research into the possibility that an infection could accelerate the progression of early-stage Alzheimer’s.
Bruce Levy, head of pulmonary care at Brigham and Women’s Hospital has also shifted gears and is now leading a clinic and research group studying long Covid.
He told me that because Boston had one of the earliest surges of Covid-19 back in the spring of 2020, he’s seeing patients who haven’t recovered for nearly two years. “We definitely need answers for those patients,” he says.
Some patients have protracted symptoms because they had severe cases that led them to the ICU, and organ damage. But others cases are more mysterious, occurring in people who had only a mild infection. Understanding why this happens is a key step to treating or preventing long Covid.
Most researchers favor the explanation that it’s chronic inflammation, perhaps triggered by an immune response that attacks the body’s own cells and doesn’t shut off properly. Others suspect it could be triggered by virus that hides out somewhere in the body.
Other scientists are trying to figure out how to predict who will completely recover and who won’t. A big collaboration of scientists just published a paper in the journal Cell using a “multi-omics” approach to finding hidden risk factors — that is, examining genes, immune system differences, chronic conditions, other viral infections and other factors that distinguish one patient from another. Levy says this kind of knowledge will be extremely valuable.
Levy says funding research into long Covid could help people who suffer from other maladies. “There’s definitely an urgent need to learn more about long Covid for the hundreds of thousands or millions of people that are experiencing it. I would also say that there is much to learn from long Covid that may translate to other conditions.”
Why not fund a moonshot program for curing long Covid? Ziyad Al-Aly, chief of research and development at the VA Saint Louis Health Care System, would like to see one. He has reason to think that long Covid is intimately connected to other major health problems.
He led a study showing that people who’ve had Covid-19 are more likely to develop heart disease, and another showing that they are more likely to suffer mental health problems including anxiety and depression.
He said there’s been a longstanding neglect of post-viral syndromes — chronic fatigue syndrome, protracted symptoms from Lyme Disease and post-influenza symptoms. Sometimes these were written off as psychosomatic, he said.
Doctors have been slow to accept other instances where infectious agents were involved in chronic diseases — including the link between human papilloma virus and cervical cancer, and between h. pylori bacteria and ulcers. Studying long Covid could help scientists unlock the mysteries of other illnesses, Al-Aly said.
The majority of people who get Covid are fine, but even if only 5 or 6% have long-term symptoms, that still adds up to a lot of people. With tens of millions of people having been infected, that’s many, many people “who are still bearing the wounds and scars from it.”
In principle, with each new wave of Covid we should be getting smarter — about mitigation, vaccines, tests, anti-viral treatments and long Covid. Funding more research is essential for making sure we’re channeling resources toward measures that work.
Updated: 5-9-2022
Think You Have Long Covid Symptoms? Here’s How To Get Help
Finding care can be frustrating for people with long-term Covid-19 symptoms. Take these steps to get the help you need.
You had Covid-19 weeks or months ago, yet you still aren’t back to normal.
You can’t exercise the way you used to. You’re depleted after a day of work. Or you may have unusual sensations, like a racing heartbeat when you stand up and difficulty concentrating at times.
Could it be long Covid? And if so, how can you find out and get the medical care you need?
As many as 23 million Americans are affected by long Covid, a March federal government report estimated, which occurs when people experience persistent and often worsening or new symptoms more than a month after a Covid-19 infection.
Even those who had mild cases with their initial infection can experience symptoms weeks later.
Many people find it difficult to get care, with doctors dismissing symptoms, not knowing what to do or even giving damaging advice, patients and doctors say. For now, there is no cure for long Covid, but finding the right doctors and tests can give you a better chance of improving and learning to manage your symptoms.
Here are care-seeking strategies recommended by long Covid doctors and patients.
It’s Been More Than Four Weeks And I Still Haven’t Fully Recovered From My Covid-19 Infection. Do I Have Long Covid?
Not necessarily. Doctors say some people take longer to fully recover from a viral illness but eventually do without needing any kind of specialized care.
There is no standard definition of long Covid. The Centers for Disease Control and Prevention defines the condition as having new or ongoing health problems four or more weeks after your initial infection. The World Health Organization defines it as occurring within three months of an infection, with symptoms lasting at least two months.
Some doctors say if you’re still feeling sick four to six weeks after Covid-19 you should see your primary-care doctor. You may have symptoms that can be explained by something else, like fatigue from anemia or a thyroid condition, and it helps to rule out other issues.
Common long Covid symptoms can include cognitive issues, a racing heartbeat when you change position and extreme fatigue, particularly after physical or mental exertion.
What If I’m Still Not Feeling Better After Three Months?
This is the time frame when you might want to look for a long Covid clinic or find a doctor who is familiar with long Covid and has treated other patients.
“We typically start to get concerned about folks with persistent symptoms about 12 weeks after their initial acute infection,” says David Putrino, director of rehabilitation innovation at Mount Sinai Health System in New York City.
Long Covid clinics, which some medical systems have set up to coordinate specialized care, have different thresholds for entry. Some, such as Stanford’s, see patients three months after infection. Others, like Cleveland Clinic’s, start seeing patients a month after infection.
Mayo Clinic has a program for patients with symptoms one-to-three months post-infection, and another for those whose symptoms persist beyond three months.
Many long Covid clinics currently have monthslong waits, so it is worthwhile trying to get on wait lists as soon as you can.
What Kind Of Doctor Should I See?
There are more than 60 hospitals and healthcare systems that have started long Covid clinics and programs, according to Becker’s hospital review. Survivor Corps, a long Covid advocacy group, also has a list of centers, as well as “Covid-friendly” doctors.
A good primary-care doctor will refer you to specialists based on your symptoms. You want to find someone with experience in treating postviral illnesses, recommends Lauren Nichols, vice president of Body Politic, a patient-advocacy group.
Another helpful kind of doctor is an immunologist, who can perform more-detailed and granular blood work that primary-care doctors typically aren’t familiar with, she says.
Are There Any Red Flags I Should Be Aware Of When Looking For A Doctor?
Avoid doctors who suggest your symptoms are all the result of depression or anxiety, Dr. Putrino says. If your doctor says your tests are normal and ends the conversation there, that is a bad sign, he says.
Attributing symptoms to deconditioning and encouraging a quick return to exercise should also raise a red flag, because too much physical activity too soon can make your symptoms worse, Dr. Putrino says.
What Tests And Screenings Should I Ask My Doctor To Do?
Most clinics conduct blood work to look at indicators such as blood counts, vitamin levels, virus reactivations and inflammatory markers. Many centers also do pulmonary function tests, echocardiograms and EKGs to look for lung or heart abnormalities.
Physical-therapy evaluations can also be useful. And patients experiencing brain fog can undergo standard neuropsychology or cognitive tests.
A tilt table test, which measures changes in heart rate when you go from lying down to upright, can help diagnose whether you have POTS, or postural orthostatic tachycardia syndrome.
A common diagnosis in long Covid patients, it can cause symptoms such as dizziness, extreme fatigue and big fluctuations in heart rate and blood pressure from small movements or when standing.
Often, long Covid patients find that many tests come back normal, but a good doctor should continue to pursue answers and investigate if you’re still experiencing symptoms.
“That doesn’t mean you’re not suffering and that you’re not having issues,” says Monica Verduzco-Gutierrez, professor and chair of the department of rehabilitation medicine at the University of Texas Health Science Center at San Antonio and director of their Covid Recovery Clinic.
Is There Anything I Should Avoid As A New Long Covid Patient?
Don’t push through it. One of the most common symptoms of long Covid is postexertional malaise, which can make exertion—physical, cognitive, or emotional—exacerbate your symptoms.
Practice energy conservation techniques such as pacing. And if you’re going back to work, take it gradually if you can. Ask for accommodations if you need to. A lot of patients will go back full-time and find they can’t handle it, Dr. Verduzco-Gutierrez says.
“Go back part-time and build up slowly while you’re still recovering,” she suggests.
Is Documentation Important?
Document evidence of a positive Covid-19 test—even an at-home rapid antigen test—and make sure your doctor puts it into your medical chart. This will help you get into a long Covid clinic and can help get approvals for insurance coverage and disability claims.
Documentation like a positive POTS diagnosis from a tilt table test, or a physical therapy or cognitive evaluation, can help with applications for workers’ compensation or disability, says Kristin Englund, an infectious-disease physician at Cleveland Clinic who started the long Covid clinic there last year.
Make sure your doctor specifically and objectively measures the severity of your symptoms using established scales, Dr. Putrino says. Rather than having a subjective note on fatigue they can say, “The patient’s fatigue was objectively scored using the Fatigue Severity Scale.”
When Will I Recover?
There is no hard data on recovery trajectories; patient recovery paths vary. If you’re sick beyond three months, full recoveries aren’t the norm, but some patients report improvements in their symptoms over time.
New symptoms can occur and old ones can come back. Recovery isn’t linear, Mrs. Nichols notes.
“People need to be aware of the roller-coaster effect which you can have with this disease,” Dr. Englund says.
Updated: 5-16-2022
Long Covid Symptoms Often Include Crushing Fatigue. Here’s How To Cope
Trying to push yourself will often make the symptoms worse. Try these strategies instead.
Ken Todd, a 53-year-old in New York City, ran 18 marathons before he got Covid last year. Now, going out to brunch with friends exhausts him.
“I need to plan to basically lie down when I get home for the rest of the day,” says Mr. Todd.
He is among the many long Covid patients suffering from fatigue months after initial infection. Doctors say that many, like Mr. Todd, experience not only tiredness but also a syndrome called post-exertional malaise.
Some long Covid patients try to push through the fatigue, a decision that often backfires and makes the fatigue and other symptoms worse.
With post-exertional malaise, fatigue can worsen after even minor physical activity as well as after emotional or cognitive exertion, such as putting together a presentation for work or socializing.
The deterioration can happen immediately after the activity or a day or two later, and can last days or weeks. It is also associated with another chronic illness, myalgic encephalomyelitis/chronic fatigue syndrome, or ME/CFS.
“This is what destroys people’s lives,” says David Putrino, director of rehabilitation innovation at Mount Sinai Health System in New York City, where he has overseen the care of more than 2,000 long Covid patients. “If they put in one day of work they need two days to recover. If they go to a party they can’t go to work the next day.”
A study last year done by the Patient-Led Research Collaborative, a group of long Covid patient researchers, found that fatigue, post-exertional malaise and cognitive dysfunction were the most frequent symptoms reported by long Covid patients, with more than 80% reporting fatigue and a similar percentage citing post-exertional malaise.
Some long Covid patients describe a level of fatigue where showering is difficult. Doing laundry or going to the grocery store can feel overwhelming. Daily decisions involve choosing between having the energy for a 20-minute conversation with a spouse or going on a short walk.
Doctors disagree on how to treat fatigue and post-exertional malaise, also called PEM. Some say the best approach is a technique called pacing, which requires planning daily activities with rest breaks.
Others say a very gradual and incremental return to some physical activity is a better strategy, combined with pacing and medication, as long as patients are carefully monitored for symptom exacerbation.
Learning To ‘Pace’
Maureen Lyons, medical director of the long Covid clinic at Washington University in St. Louis, says pacing is currently the most effective intervention for managing fatigue in long Covid patients.
With pacing, patients learn to determine how to balance rest and activities to avoid exacerbating symptoms. The approach involves figuring out which times of day they have the most energy, which can be different for physical, cognitive and emotional exertion.
At the clinic, patients work with doctors to create an individualized plan for daily activities, which can take trial and error. Patients start by tracking their symptoms and activity levels, then make schedules that break up tasks into smaller chunks with rest periods in between.
For example, long Covid patients can have difficulty doing something as routine as showering or washing their hair, says Dr. Lyons. Doctors and therapists work with patients on making sure they rest before and after their shower and choosing a time when they have energy.
For laundry, patients may have to break up the task into steps with rest periods, or avoid going up and down the stairs too many times.
Susan Levine, a New York City-based infectious disease physician with an expertise in ME/CFS, now sees hundreds of long Covid patients. She recommends that patients have some sort of routine in their life that includes a little bit of activity, even if it’s just five minutes of walking to start.
A minimum level of activity will help patients slowly rehabilitate, she says. And she says patients should seek strategies for tackling fatigue as soon as possible, within the first year of symptoms.
A Gradual Return To Exercise
David Systrom is an associate physician at Brigham and Women’s Hospital in Boston who studies and treats ME/CFS and long Covid patients at an exercise testing program there.
He says they’ve found that the most effective way to manage and even improve fatigue and post-exertional malaise is to first treat patients with drugs commonly used to treat a blood circulation disorder that long Covid patients are frequently diagnosed with.
The medication can improve the blood circulation of patients, he says. Then, they are able to start a graded exercise program. He acknowledges that the introduction of exercise, even incrementally, is controversial because some say it risks triggering the post-exertional malaise that worsens the fatigue.
Yet he says that trying to gradually introduce exercise is important because pacing alone can only manage symptoms, rather than improve the condition overall.
Gentle Rehab
Dr. Putrino at Mount Sinai says the most effective strategy depends on what is causing the fatigue. For some patients, he says, the culprit is a problem with cellular-energy dysfunction, and for them, an increase in physical activity will backfire.
Others, he says, are experiencing dysfunction in their autonomic nervous system. For those patients, a specific kind of rehabilitation involving gentle limb exercises can often help them improve and even recover, he says.
Many long Covid patients experience both of these problems. When that’s the case, patients must undergo very gradual rehab—starting with gentle limb stretches lying on the ground—without having the activity trigger post-exertional malaise, he says.
Mr. Todd, the former marathoner in New York, has used pacing techniques as well as incremental increases in physical activity to try to improve his fatigue and post-exertional malaise.
He says initially he could only handle working two days a week and they couldn’t be consecutive. He had to take frequent breaks and naps. Now, he’s worked up to four days a week and recently returned to the office one day a week.
He has a private office with a couch and will nap or rest when needed, which is usually after 45 minutes or less of working.
He has gradually increased his physical activity with the help of physical therapy and tries to walk 2 miles in the morning and evening when he has the energy.
He’s starting to introduce short jogging intervals. “I consider each day to have an ‘exertion’ budget where I have to make activity trade-offs every day in order to not overdo it,” he says.
Vestibular therapy to improve balance and dizziness, along with medications, have also helped as he can feel sick and dizzy after working at a computer too long.
Mr. Todd says he’s still only a little more than halfway back to his pre-Covid baseline when he did vigorous exercise five to six days a week, including runs or CrossFit workouts. Even tasks such as cleaning the bathroom can be challenging, and he breaks them up over several days.
“This is a life-changing disability,” says Mr. Todd.
Updated: 5-25-2022
A Heart-Failure Drug Tames Palpitations In Long-Covid Patients
Doctors don’t yet fully understand the cause but find a way to bring relief.
More than 200 symptoms can afflict those dealing with the aftereffects of Covid-19. An emerging approach to treating one of them—heart palpitations—highlights the successes scientists are having in addressing the symptoms, even if it may take years to understand how they’re caused.
About 11% of coronavirus patients report experiencing palpitations or an increased heart rate, according to a meta-analysis of long-Covid studies published in the journal Scientific Reports in August. The symptoms are suggestive of a broader condition called postural orthostatic tachycardia syndrome, or POTS, which affects more than 24 million Americans—a number that’s growing because of Covid.
POTS is more prevalent among women of childbearing age; often coincides with lightheadedness, brain fog, and gastric upset; and can eventually lead to chronic fatigue.
To normalize the rhythm of the heart for people with POTS, cardiologists are turning to the off-label use of a drug more commonly prescribed for heart-failure patients: Amgen Inc.’s Corlanor.
Pam Taub, a cardiologist and professor of medicine at the UC San Diego School of Medicine, says she’s prescribed Corlanor, which goes by the generic name ivabradine, along with specific exercises, to hundreds of patients with POTS, including many so-called Covid long-haulers.
“Within a month or two, patients will come back to me and say, ‘I feel better, my heart rate is now much lower,’ and then I start titrating them off the drug,” she says.
Ivabradine was effective at lowering the heart rate in POTS patients in a randomized, controlled clinical trial involving 22 people whose average age was 32 years, which Taub conducted just before the pandemic.
The results were published in the Journal of the American College of Cardiology in 2021. Mitchell Miglis, a clinical associate professor of neurology and neurological sciences at Stanford University, also prescribes the medication to treat POTS in patients with long Covid.
“It works just as well in post-Covid POTS as in non-Covid POTS,” he says. Miglis and colleagues showed in a study in April—based on an online survey of 2,314 adults with long Covid—that about two-thirds of patients have symptoms suggestive of an impaired autonomic nervous system, which controls heart rate, blood pressure, digestion, body temperature, and other “automatic” functions of the body.
POTS is the most common manifestation of autonomic dysfunction. Before Covid, the syndrome was often seen in patients recovering from influenza or another viral infection.
Patients with POTS typically experience a heart rate that increases by 30 or more beats per minute within 10 minutes of standing up after lying or sitting.
Noticeable heart pounding or palpitations are usually accompanied by poor blood circulation and a spectrum of symptoms including headaches, nausea, difficulty urinating, and a loss of sexual function.
“It doesn’t usually kill you, but you can be very miserable,” says Paul LeLorier, professor of clinical medicine and director of the electrophysiology service at Louisiana State University Health Sciences Center in New Orleans. “Some people describe it as being perpetually hungover or having had 50 Red Bulls.”
The difficulty of focusing and concentrating that often coincides with POTS can disrupt employment or education, while fatigue can frustrate patients’ rehabilitation through physical therapy and exercise, LeLorier says.
Although many patients with long Covid recover from their symptoms within a few months, those with POTS lasting six months or more begin to resemble patients experiencing myalgic encephalomyelitis/chronic fatigue syndrome, or ME/CFS, a more disabling condition that leaves at least 1 in 4 sufferers bed- or housebound for long periods, says Akiko Iwasaki, a professor of immunobiology and molecular, cellular, and developmental biology at Yale.
“Once you get to that level, we should really be considering long Covid a form of ME/CFS,” she says.
It’s important to identify the signs of POTS early and intervene before patients “go into this downward spiral,” says Taub. Wearing compression garments, increasing salt intake, and gradual exercise done initially in a horizontal position, such as recumbent cycling and swimming, are mainstay treatments for POTS.
Heart medications known as beta blockers and calcium channel blockers have also been used, though these can lower blood pressure and make patients feel worse, Taub says. Ivabradine is an alternative that selectively slows the firing rate of the heart’s sinus node, which regulates the speed at which the organ pumps blood.
Scientists have yet to pinpoint exactly how Covid causes persistent or long-haul symptoms in at least 10% of survivors. “This is such a complex disease,” Taub says. “The best approach is to say, ‘OK, what are the things that we can treat?’ ”
Updated: 5-28-2022
Long Covid Found In 20% Of US Cases
About 1 in 5 US adults have health problems from Covid that stick around long after they first test positive, according to a report from the Centers for Disease Control and Prevention published this week.
Experts from the CDC detailed how, after an initial bout of Covid, a growing number of people age 18 and older continued to report symptoms that may be caused by the virus.
The agency used electronic health records from March 2020 through November 2021 to analyze patients who reported certain symptoms one month to a year after having Covid.
And as Covid cases continue to increase in some parts of the US, including several regions that now fall into the CDC’s “high risk” category, the number of people with long Covid is likely to only increase, the report notes.
The study didn’t assess the incidence of post-Covid symptoms in kids, an estimated half a million of whom are also suffering from lasting health problems and who can be harder to diagnose than adults.
For the 20% of adults whose symptoms can last weeks to months after a positive Covid test, researchers said the most common conditions were respiratory problems and muscle or joint pain.
There was also a notable risk of pulmonary embolism, a blood clot that can travel to the lungs, among the patients included in the study.
But people suffering from long Covid can have very different symptoms, too. In the study, just 26 conditions associated with long Covid were considered, but there have been over 200 different symptoms reported after Covid, ranging from neurological to cardiovascular.
Researchers also noted that symptoms were more likely to appear based on age. In the study, adults under 65 more frequently experienced an irregular heartbeat and muscle pain, while those older than 65 had a higher risk of kidney failure, blood clots, muscle disorders, type 2 diabetes and mental health problems. Almost half of those older adults also had neurocognitive issues, the study says.
The findings, health officials say, are consistent with other studies that estimate about 20% to 30% of people develop long Covid and can help increase awareness of the condition, as well as treatment.
But more research is still needed to determine what makes certain people more vulnerable to developing long Covid, the report says.
More resources are being devoted to studying long Covid now than earlier in the pandemic, and some progress is finally being made in treating certain symptoms. But still, experts remain largely in the dark about what causes it.
Updated: 6-15-2022
Long Covid Is Showing Up In The Employment Data
More Americans in and out of the labor force are having trouble remembering and concentrating, a common Covid-19 aftereffect.
The number of Americans applying for Social Security Disability Insurance rose sharply during the 2000s, a phenomenon that appears to have been driven more by the job market — which was pretty weak for most of the decade, especially for those without college degrees — than by people’s health.
Lately, the job market has been quite strong, with the number and rate of job openings at all-time highs. Yet SSDI applications are (slowly) rising again, in their first sustained increase since 2009.
Social Security field offices were closed to visitors from March 2020 until this April, which the Social Security Administration said led to a decline in disability claims. So some of what we’re seeing is just catchup.
But there is something else that might also be playing a role: the lingering effects of Covid-19 infections, aka Long Covid.
Given that you have to be unable to work for at least 12 months to qualify for Social Security disability and going on the program is a momentous step that effectively requires leaving the labor market, the still-new phenomenon that is Long Covid is probably not playing a big role (the Social Security Administration has said that only about 1% of recent claims mention Covid).
Still, the turnaround in disability applications is at least not incompatible with a rise in long-term health problems related to the disease — and it turns out there are stronger signs of Long Covid in other employment-related data.
I started looking for them in part because I was dubious of some of the direct estimates of the scope of the phenomenon. With blood tests showing 58% of Americans infected with Covid-19 through February, studies finding that 10% or 25% or 30% or 37% or 55% of those with the disease develop long-term symptoms imply that 20 million to 100 million of us have Long Covid.
An April attempt by the advocacy group Solve Long Covid Initiative to whittle that down to “disabling” cases still put the range at 7 million to 14 million, or 2.3% to 4.4% of US adults.
Given that labor-force-participation and employment rates in May were only about half a percentage point below where they were before the pandemic for prime-working-age adults (those aged 25 through 54), and above pre-pandemic levels for those aged 55 to 64, such estimates seem high.
Still, dig a little deeper into the monthly Current Population Survey from which these statistics are derived and it is apparent that something new is ailing millions of Americans, even though many are staying on the job despite it.
The Census Bureau, which conducts the 60,000-household CPS on behalf of the Bureau of Labor Statistics, asks about disabilities as well as employment.
The resulting estimate of the number of 16-and-older Americans with a disability is up by about two million since early 2020. It had been rising over the decade before then as the population aged, but not at nearly that fast a pace.
These two million additional disabled Americans are divided almost equally between people who are in the labor force (that is, they’re employed or actively looking for a job) and people who aren’t. Since the latter group make up the great majority of the disabled, the increase in disability among those in the labor force has been much sharper in percentage terms.
That dip in disability in spring 2020 was likely not for real: Survey response rates plummeted in the early months of the pandemic, with lower-income households seeing the biggest drop, skewing the results.
What’s happened since spring 2021, though, has the look of being driven by actual changes in health status. More than a million additional Americans, representing a 19% increase from before the pandemic, are complaining of a disability while continuing to work.
What’s Ailing Them? The Six Questions That Census Bureau Survey Takers Ask To Determine Disability Are:
* Is Anyone [In Your Household] Deaf Or Does Anyone Have Serious Difficulty Hearing?
* Is Anyone Blind Or Does Anyone Have Serious Difficulty Seeing Even When Wearing Glasses?
* Because Of A Physical, Mental, Or Emotional Condition, Does Anyone Have Serious Difficulty Concentrating, Remembering, Or Making Decisions?
* Does Anyone Have Serious Difficulty Walking Or Climbing Stairs?
* Does Anyone Have Difficulty Dressing Or Bathing?
* Because Of A Physical, Mental, Or Emotional Condition, Does Anyone Have Difficulty Doing Errands Alone Such As Visiting A Doctor’s Office Or Shopping?
If The Answer To One Or More Of Those Is Yes, The Person Is Counted As Disabled. Here’s How The Responses Have Changed Over The Course Of The Pandemic:
We’re Having Some Trouble Concentrating
Change over the course of the Covid-19 pandemic* in the number of Americans 16 and older who have serious difficulty …
Having trouble concentrating, remembering or making decisions (I lopped off that last bit in the table to make it more readable) tracks well with the common Long Covid symptom known as “brain fog.”
Fatigue and difficulty breathing, two other top Long Covid symptoms, are less directly addressed by the disability questions, although they might be reflected in difficulty doing errands alone and walking or climbing stairs.
Hearing problems such as tinnitus have also been associated with Covid, although they aren’t near the top of the list of lingering symptoms.
The craziness of the past couple of years is another possible cause of all that brain fog, as well as of the kind of anxiety that might keep one from venturing out on errands. But another survey that the Census Bureau started conducting early in the pandemic points to a Covid connection.
Since January 2021, the online Household Pulse Survey has included a question about past Covid-19 diagnoses, and since April 2021 it has included questions similar to the first four disability queries in the CPS, albeit with multiple choice answers rather than yes-no.
The percentage of respondents reporting severe problems remembering or concentrating has gone up both among those who’ve definitely had Covid and those who probably haven’t, but it’s higher and the rise has been steeper among the first group.
On the basis of the Household Pulse responses, the Census Bureau estimated that during the survey period of April 27 through May 9 of this year, 5.1 million Americans aged 18 and older had (1) a previous Covid-19 diagnosis and (2) severe difficulty with remembering or concentrating.
A lot of those memory and concentration problems likely predated Covid, and big changes in response rates over time make it hard to compare estimates from the most recent Household Pulse surveys with those from spring 2021.
But my back-of-the-envelope estimate 1 from the Household Pulse results is that overall about 2.2 million more US adults are complaining of severe brain-fog-like problems now than in spring 2021. The CPS-based estimate, recorded in the table above, is that there are 1.2 million more than before the pandemic.
Neither of those is 20 million, or even seven million, but it’s a lot of people and the number could keep growing. This accounting may also miss many who are suffering from fatigue, breathing or other Long Covid complaints not captured so well by the surveys.
Neither the Household Pulse survey nor the CPS — including the set of pandemic-related questions added to it in May 2020 — addresses Long Covid much more directly than this.
Even the Survey of Working Arrangements and Attitudes organized by economists Jose Maria Barrero, Nicholas Bloom and Steven J. Davis, which has focused on some important Covid-related topics that government surveys have not, has so far avoided health questions out of concern that, as Bloom put it in an email, they were “maybe too sensitive to include in the survey.”
Barrero, Bloom and Davis did conclude recently that what they called “Long Social Distancing,” prompted in part by concerns about catching Covid-19, is depressing the 16-and-older US labor-force participation rate by about 2.5 percentage points, which adds up to more than six million people.
The Long Covid effect is probably smaller than that: In a January Brookings Institution report, jobs expert (and pizza-company executive) Katie Bach estimated on the basis of several studies that it was costing the US labor market about 1.6 million full-time equivalent workers, which seems to be in the same ballpark as what I found.
That’s still enough to have an impact, especially at a time when available jobs are more plentiful than people looking for them — as Bach put, it’s equivalent to about 15% of all unfilled US jobs.
And discussing this purely in terms of how it has affected employment and labor-force participation is probably a mistake.
My reading of the disability data is that the majority of people with Long Covid-like symptoms are still working, and I imagine that even most of those with debilitating cases would prefer not to check out of the labor force for good.
There do, however, seem to be a lot of Long Covid sufferers who could use some help. Which brings me back to Social Security Disability Insurance, a program that has long been criticized for disconnecting recipients from the labor market.
In 2010, economists David Autor and Mark Duggan proposed a new approach that would offer:
* Workplace accommodations, rehabilitation services, partial income support, and other services to workers who suffer work limitations, with the goal of enabling them to remain in employment;
* Financial incentives to employers to accommodate workers who become disabled and minimize movements of workers from their payrolls onto the SSDI system
With encouragement from Congress, the Social Security Administration has been undertaking some experiments along these lines. Long Covid seems like good reason to speed up the process.
Updated: 3-7-2022
Brain Shrinkage, Cognitive Decline Found Months After Mild Covid
* The Abnormalities Resemble Up To A Decade Of Brain Aging
* More Research Is Needed To Gauge Duration Of Virus’s Impact
Even a mild case of Covid-19 can damage the brain and addle thinking, scientists found in a study that highlights the illness’s alarming impact on mental function.
Researchers identified Covid-associated brain damage months after infection, including in the region linked to smell, and shrinkage in size equivalent to as much as a decade of normal aging. The changes were linked to cognitive decline in the study, which was published Monday in the journal Nature.
The findings represent striking evidence of the virus’s impact on the central nervous system. More research will be required to understand whether the evidence from the Wellcome Centre for Integrative Neuroimaging at the University of Oxford means Covid-19 will exacerbate the global burden of dementia — which cost an estimated $1.3 trillion in the year the pandemic began — and other neurodegenerative conditions.
“It is a very novel study with conclusive data,” said Avindra Nath, clinical director of the U.S. National Institute of Neurological Disorders and Stroke, who wasn’t involved in the research. “The findings are very intriguing, with important implications for the population at large.”
The SARS-CoV-2 virus is widely considered a respiratory pathogen that attacks the lungs. Taking a narrow view of it, however, misses myriad neurologic complications — including confusion, stroke, and neuromuscular disorders — that manifest during the acute phase of the illness.
Other effects like impaired concentration, headache, sensory disturbances, depression, and even psychosis may persist for months as part of a constellation of symptoms termed long Covid.
To investigate changes in the brain, neuroscientist Gwenaelle Douaud and colleagues leveraged the world’s largest magnetic resonance imaging database.
Initial MRI scans of the brains of 785 volunteers were taken before the pandemic began as part of U.K. Biobank research, which marries large-scale genomic and detailed clinical data for half a million people.
A subsequent scan was taken an average of 38 months later. By then, 401 participants had tested positive for Covid. The uninfected remainder served as a control group that was similar to the survivors in age, sex, and many risk factors, including blood pressure, obesity, smoking, socio-economic status and diabetes. The participants in the study, aged 51 to 81, were mostly Caucasian.
‘Quite Surprised’
“We were quite surprised to see some clear differences in how the brain had changed in the participants who have become infected,” Douaud said in an interview. Whether the effects persist, or can be partially reversed as neuronal networks repair, requires further investigation, she said. “The brain is ‘plastic’ and can heal itself.”
Among those infected an average of 4.5 months prior to their second scan, the researchers found a greater reduction in grey matter thickness in the regions of the brain associated with smell, known as the orbitofrontal cortex and parahippocampal gyrus.
The finding may help explain the impaired olfaction many Covid patients experience, as a result of either direct viral damage or inflammation spurred by the body’s immune response to the virus.
A loss of grey matter, which makes up the outer most layer of the brain, represents degeneration, said Leah Beauchamp, a neuropharmacologist at the Florey Institute of Neuroscience and Mental Health in Melbourne. “This is really concerning,” she said.
Updated: 1-4-2023
Essential Oils May Help Restore Sense of Smell After COVID
Personalized essential oils may help people recover their lost sense of smell due to COVID-19, according to a new study.
Called olfactory training, the process involves smelling the oils regularly to “challenge” the nerves responsible for sending smell messages to the brain, according to The Mayo Clinic. Those nerves are known to be able to heal and regrow in a process called neuroplasticity.
The study was published last week in JAMA Otolaryngology-Head & Neck Surgery. It included 275 people ages 18 to 71 who reported loss of smell due to COVID-19. Participants sniffed the oils for 15 seconds with a 30-second rest in between odors. The study lasted for 3 months.
A traditional olfactory training protocol uses four specific scents: rose, lemon, eucalyptus, and clove. One group in the new study used those scents, while another group sniffed four scents that they selected themselves from 24 scent options. A third control group did not participate in olfactory training. Additionally, a subset of people in the study were shown images of the scents they smelled.
While there were no “definitive” differences between the individual approaches, the researchers noted that there may be benefits for patients who get to both select their scents and see images of the scents.
In a companion commentary published with the study, Carol Yan, MD, of the University of California San Diego, said the improvements some patients saw may have been a placebo effect and should be considered for treatment plans of patients who lost their sense of smell due to COVID-19.
“Allowing patients to select their own odorants may improve cost-effectiveness and increase adherence, particularly if there was an issue of familiarity with 1 of the classic 4 odorants,” she wrote. “The addition of visual cues to [olfactory training] may improve engagement in some patients while increasing the burden on others. Ultimately, patients’ belief and satisfaction in their therapeutic plan can have substantial placebo-effect benefits that are not to be ignored.”
An estimated 700,000 people have lost their sense of smell due to COVID-19, the authors said. Most people regain their sense of smell within a year.
Smell Retraining Therapy And Long COVID
You can use smell retraining therapy (SRT) if you have loss of sense of smell due to long COVID.
What Is It?
Most people with long COVID gradually regain their sense of smell, though this can take months or even longer. Patience is key. You can use SRT at home (also called olfactory training). Studies show SRT is generally effective, though results vary from person to person.
SRT works by strengthening the nerves involved in our sense of smell.
Some people also lose their sense of taste. SRT can help you recover this sense, as well.
How Do I Do It?
Start with 4 scents. These 4 work well for most people: rose, eucalyptus, lemon, and clove. If there’s a scent you especially want to be able to smell, include it as one of your 4 scents.
Follow These Steps:
- Choose a scent and smell it for 15 seconds, while asking yourself to remember what it smells like.
- Rest for 10 seconds.
- Smell the next scent for 15 seconds.
- Rest for 10 seconds.
- Repeat until you’ve sampled all 4 scents.
- Do the 4-scents cycle, 2 times every day.
After 3 months, switch to 4 new scents. Use them with the same twice-daily method. Suggestions: menthol, thyme, tangerine, and jasmine.
After 3 more months (6 months after starting SRT), again switch to 4 new scents. Suggestions: green tea, bergamot, rosemary, and gardenia.
Many people use scented essential oils. You can purchase essential oils online or in health stores, grocery stores and some pharmacies. It’s also fine to use herbs, spices, teas, or similar products. You may already have some scented items in your kitchen or garden.
Related Articles:
Bitcoin Information & Resources (#GotBitcoin)
Students Take To The Streets For Day Of Action On Climate Change
Paying Off Unfunded Pension Liabilities Will Be A Low Priority After COVID-19 (#GotBitcoin)
Pension Funds And Insurance Firms Alive To Bitcoin Investment Proposal
Ley Lines: The Earth’s Energy Highways
Ultimate Resource On Biden Administration’s Student-Loan Forgiveness Program
Biden’s Student Loan Freeze Shows Path To Erase Billions Of Debt
The Number Of Americans Who Say They Were Rejected For A Loan Reaches Highest Rate In 5 Years
Mass Immigration Experiment Gives Canada An Edge In Global Race For Labor
Silver Lining of Coronavirus, Return of Animals, Clear Skies, Quiet Streets And Tranquil Shores
Meet The Women Who Track Down And Kill Poachers
Ultimate Resource On President Joe Biden’s $1.3 Trillion Infrastructure Program
Electric Vehicle Infrastructure Push Brings Cyber Concerns
Ultimate Resource For Biden’s Infrastructure Plans And It’s Impact On The Crypto-Currency Industry
The Future of Water Is (And Toilets) Recycled Sewage, You’ll Drink It And You’ll Like It😹😂🤣
The Key To Tracking Diseases And Other Ailments Should Start With Sewers
Kia Motors America Victim of Ransomware Attack Demanding $20M In Bitcoin, Report Claims
This Massive Phishing Campaign Delivers Password-Stealing Malware Disguised As Ransomware
A New Ransomware Enters The Fray: Epsilon Red
UK Cyber Chief Cameron Says Ransomware Key Online Threat
It Was Not Until Anonymous Payment Systems That Ransomware Became A Problem
REvil Ransomware Hits 200 Companies In MSP Supply-Chain Attack
Russia ‘Cozy Bear’ Breached GOP As Ransomware Attack Hit
US Fights Ransomware With Crypto Tracing, $10 Million Bounties
US Taps Amazon, Google, Microsoft, Others To Help Fight Ransomware, Cyber Threats
Google’s Chrome Browser Is Under Active Attack, Patch Now!!!!
Leaked Chainalysis Documents Reveal Company Is Advertising An IP-Scraping System To Law Enforcement
Hackers Breach Thousands of Security Cameras, Exposing Tesla, Jails, Hospitals
Major Hospital System Hit With Cyberattack, Potentially Largest In U.S. History
A Hospital Hit By Hackers, A Baby In Distress: The Case Of The First Alleged Ransomware Death
Major League Cricket Takes Off In US
America Is Wrapped In Miles of Toxic Lead Cables
What Is Dollar Cost Averaging Bitcoin?
The NASA Engineer Who Made The James Webb Space Telescope Work
The Webb Telescope Turns Big Bang Theory Upside-Down
Wagner Group: A State-Backed Russian Paramilitary Cartel
Debt Collectors’ Awkward Moment: Their Own Debt Is Now Sinking
Ultimate Resource On Brittney Griner Being Held In Russian Jail
Mocked As ‘Rubble’ By Biden, Russia’s Ruble Roars Back
Ultimate Resource On Russia’s Involvement With Bitcoin
What Is Structured Water: The Best Water For Muscular, Skin & Mood Disorders?
“Would Someone Please Buy US Treasury Bonds?” Janet Yellen #GotBitcoin
‘It Will Send BTC’ — On-Chain Analyst Says Bitcoin Hodlers Are Only Getting Stronger
HODLing Early Leads To Relationship Troubles? Redditors Share Their Stories
Governments Will Start To Hodl Bitcoin In 2021
Bitcoin’s Value Is All In The Eye Of The ‘Bithodler’
Ultimate Resource On Blue And Green Hydrogen As Alternative Energy
Ultimate Resource On Small And Mega-Battery Innovations And Facilities
Governments Turn Against Deep-Sea Mining In The Face Of Increase In Demand For Metals
How To Bulk: A Complete Workout And Nutrition Plan For Muscle Growth
What You Should Know About ‘529’ Education-Savings Accounts
Kia And Hyundai To Pay $200 Million To Settle Viral Car-Theft Suit
Stock Clearinghouse Leaked Sensitive Data, Trading Firm Says #GotBitcoin
Scarlette Bourne Joins Our List of 2023’s Most Influential Women
Surge In Celebrities And Others Contributing To Nonprofits Focusing On Blacks
Israel-Gaza Conflict Spurs Bitcoin Donations To Hamas
Signal Encrypted Messenger Now Accepts Donations In Bitcoin
Melinda Gates Welcomes The Philanthropists Of The Future
Who Gets How Much: Big Questions About Reparations For Slavery
California Lawmakers Vote To Create Reparations Task Force
US City To Pay Reparations To African-American Community With Tax On Marijuana Sales
Ultimate Resource On Australia’s Involvement With Bitcoin
Famous Former Bitcoin Critics Who Conceded In 2020-23
The Latest On FBI Warrantless Searches of Americans’ Communications #GotBitcoin
America’s Spies Are Losing Their Edge
Powell Got Punk’d By Putin’s Puppets
‘What Housewife Isn’t On Ozempic?’ How A Weight-Loss Craze Is Sweeping Across America
Snoop Dogg’s Net Worth Is Almost As High As He (Usually) Is
Is It Just Me Or Is America Having A Mental Breakdown? Joker
CFPB (Idiots) Says Staffer Sent 250,000 Consumers’ Data To Personal Account #GotBitcoin
Global Bitcoin Game Theory Is Now Playing Out
Operation Choke Point 2.0 Could Be Bitcoin’s Biggest Banking Crackdown And Regulatory Battle
The US Cracked A $3.4 Billion Crypto Heist—And Bitcoin’s Pseudo-Anonymity😹🤣😂
Twitter To Launch Bitcoin And Stock Trading In Partnership With eToro
Rich Chinese Splashing Out On Luxury In Singapore
Apple Sues NSO Group To Curb The Abuse Of State-Sponsored Spyware
Harvard Quietly Amasses California Vineyards—And The Water Underneath (#GotBitcoin)
US Says China Backed Hackers Who Targeted COVID-19 Vaccine Research
Ultimate Resource For Covid-19 Vaccine Passports
Companies Plan Firings For Anti-Vaxers And Giveaways For Covid-19 Vaccine Recipients
US Bank Lending Slumps By Most On Record In Final Weeks Of March And It’s Impact On Home Buyers
California Defies Doom With No. 1 U.S. Economy
California Wants Its Salton Sea Located In The Imperial Valley To Be ‘Lithium Valley’
Ultimate Resource For Nationwide Firsts Taking Place In California (#GotBitcoin)
Flight To Money Funds Is Adding To The Strains On Banks #GotBitcoin
The Fed Loses Money For The First Time In 107 Years – Why It Matters #GotBitcoin
African Safari Vacation Itinerary (2024 Proposal)
The Next Fountain-of-Youth Craze? Peptide Injections
This Ocean Monster Offers A Potential Climate Solution
What Are Credit Default Swaps, How Do They Work, And How They Go Wrong
Cyberattack Sends Quadrillion Dollars Derivative’s Trading Markets Back To The 1980s #GotBitcoin
What Is Dopamine Fasting? Meet The Dangerous Fad Among Silicon Valley’s Tech Geniuses
Bitcoin Community Leaders Join Longevity Movement
Sean Harribance Shares His Psychic Gifts With The Public
Scientists Achieve Real-Time Communication With Lucid Dreamers In Breakthrough
Does Getting Stoned Help You Get Toned? Gym Rats Embrace Marijuana
Marijuana In Africa Is Like The Gold Rush For America In The 1800s
The Perfect Wine And Weed To Get You Through The Coronavirus Pandemic Lockdown
Mike Tyson’s 420-Acre Weed Ranch Rakes In $500K A Month
What Sex Workers Want To Do With Bitcoin
“Is Bitcoin Reacting To The Chaos Or Is Bitcoin Causing The Chaos?” Max Keiser
How To Safely Store Deposits If You Have More Than $250,000
How To Host A Decentralized Website
Banks Lose Billions (Approx. $52 Billion) As Depositors Seek Higher Deposit Yields #GotBitcoin
Crypto User Recovers Long-Lost Private Keys To Access $4M In Bitcoin
Stripe Stops Processing Payments For Trump Campaign Website
Bitcoin Whales Are Profiting As ‘Weak Hands’ Sell BTC After Price Correction
Pentagon Sees Giant Cargo Cranes As Possible Chinese Spying Tools
Bitcoin’s Volatility Should Burn Investors. It Hasn’t
Bitcoin’s Latest Record Run Is Less Volatile Than The 2017 Boom
“Lettuce Hands” Refers To Investors Who Can’t Deal With The Volatility Of The Cryptocurrency Markets
The Bitcoiners Who Live Off The Grid
US Company Now Lets Travelers Pay For Passports With Bitcoin
After A Year Without Rowdy Tourists, European Cities Want To Keep It That Way
Director Barry Jenkins Is The Travel Nerd’s Travel Nerd
Four Stories Of How People Traveled During Covid
Who Is A Perpetual Traveler (AKA Digital Nomad) Under The US Tax Code
Tricks For Making A Vacation Feel Longer—And More Fulfilling
Travel Has Bounced Back From Coronavirus, But Tourists Stick Close To Home
Nurses Travel From Coronavirus Hot Spot To Hot Spot, From New York To Texas
How To Travel Luxuriously Post- Covid-19, From Private Jets To Hotel Buyouts
Ultimate Travel Resource Covering Business, Personal, Cruise, Flying, Etc.)
Does Bitcoin Boom Mean ‘Better Gold’ Or Bigger Bubble?
Bitcoin’s Slide Dents Price Momentum That Dwarfed Everything
Retail Has Arrived As Paypal Clears $242M In Crypto Sales Nearly Double The Previous Record
Jarlsberg Cheese Offers Significant Bone & Heart-Health Benefits Thanks To Vitamin K2, Says Study
Chrono-Pharmacology Reveals That “When” You Take Your Medication Can Make A Life-Saving Difference
Ultimate Resource For News, Breakthroughs And Innovations In Healthcare
Ultimate Resource For Cooks, Chefs And The Latest Food Trends
Ethereum Use Cases You Might Not Know
Will 1% Yield Force The Fed Into Curve Control?
Ultimate Resource On Hong Kong Vying For World’s Crypto Hub #GotBitcoin
France Moves To Ban Anonymous Crypto Accounts To Prevent Money Laundering
Numerous Times That US (And Other) Regulators Stepped Into Crypto
Where Does This 28% Bitcoin Price Drop Rank In History? Not Even In The Top 5
Traditional Investors View Bitcoin As If It Were A Technology Stock
3 Reasons Why Bitcoin Price Abruptly Dropped 6% After Reaching $15,800
As Bitcoin Approaches $25,000 It Breaks Correlation With Equities
UK Treasury Calls For Feedback On Approach To Cryptocurrency And Stablecoin Regulation
Bitcoin Rebounds While Leaving Everyone In Dark On True Worth
Slow-Twitch vs. Fast-Twitch Muscle Fibers
Biden, Obama Release Campaign Video Applauding Their Achievements
Joe Biden Tops Donald Trump In Polls And Leads In Fundraising (#GotBitcoin)
Trump Gets KPOP’d And Tic Toc’d As Teens Mobilized To Derail Trump’s Tulsa Rally
Schwab’s $200 Million Charge Puts Scrutiny On Robo-Advising
TikTok Is The Place To Go For Financial Advice If You’re A Young Adult
TikTok Is The Place To Go For Financial Advice If You’re A Young Adult
American Shoppers Just Can’t Pass Up A Bargain And Department Stores Pay The Price #GotBitcoin
Motley Fool Adding $5M In Bitcoin To Its ‘10X Portfolio’ — Has A $500K Price Target
Mad Money’s Jim Cramer Invests 1% Of Net Worth In Bitcoin Says, “Gold Is Dangerous”
Ultimate Resource For Financial Advisers By Financial Advisers On Crypto
Anti-ESG Movement Reveals How Blackrock Pulls-off World’s Largest Ponzi Scheme
The Bitcoin Ordinals Protocol Has Caused A Resurgence In Bitcoin Development And Interest
Bitcoin Takes ‘Lion’s Share’ As Institutional Inflows Hit 7-Month High
Bitcoin’s Future Depends On A Handful of Mysterious Coders
Billionaire Hedge Fund Investor Stanley Druckenmiller Says He Owns Bitcoin In CNBC Interview
Bitcoin Billionaire Chamath Palihapitiya Opts Out Of Run For California Governor
Billionaire Took Psychedelics, Got Bitcoin And Is Now Into SPACs
Billionaire’s Bitcoin Dream Shapes His Business Empire In Norway
Trading Firm Of Richest Crypto Billionaire Reveals Buying ‘A Lot More’ Bitcoin Below $30K
Simple Tips To Ensure Your Digital Surveillance Works As It Should
Big (4) Audit Firms Blasted By PCAOB And Gary Gensler, Head Of SEC (#GotBitcoin)
What Crypto Users Need Know About Changes At The SEC
The Ultimate Resource For The Bitcoin Miner And The Mining Industry (Page#2) #GotBitcoin
How Cryptocurrency Can Help In Paying Universal Basic Income (#GotBitcoin)
Gautam Adani Was Briefly World’s Richest Man Only To Be Brought Down By An American Short-Seller
Global Crypto Industry Pledges Aid To Turkey Following Deadly Earthquakes
Money Supply Growth Went Negative Again In December Another Sign Of Recession #GotBitcoin
Here Is How To Tell The Difference Between Bitcoin And Ethereum
Crypto Investors Can Purchase Bankruptcy ‘Put Options’ To Protect Funds On Binance, Coinbase, Kraken
Bitcoin Developers Must Face UK Trial Over Lost Cryptoassets
Google Issues Warning For 2 Billion Chrome Users
How A Lawsuit Against The IRS Is Trying To Expand Privacy For Crypto Users
IRS Uses Cellphone Location Data To Find Suspects
IRS Failed To Collect $2.4 Billion In Taxes From Millionaires
Treasury Calls For Crypto Transfers Over $10,000 To Be Reported To IRS
Can The IRS Be Trusted With Your Data?
US Ransomware Attack Suspect Hails From A Small Ukrainian Town
Alibaba Admits It Was Slow To Report Software Bug After Beijing Rebuke
Japan Defense Ministry Finds Security Threat In Hack
Raoul Pal Believes Institutions Have Finished Taking Profits As Year Winds Up
Yosemite Is Forcing Native American Homeowners To Leave Without Compensation. Here’s Why
What Is Dollar Cost Averaging Bitcoin?
Ultimate Resource On Bitcoin Unit Bias
Best Travel Credit Cards of 2022-2023
A Guarded Generation: How Millennials View Money And Investing (#GotBitcoin)
Bitcoin Enthusiast And CEO Brian Armstrong Buys Los Angeles Home For $133 Million
Nasdaq-Listed Blockchain Firm BTCS To Offer Dividend In Bitcoin; Shares Surge
Ultimate Resource On Kazakhstan As Second In Bitcoin Mining Hash Rate In The World After US
Ultimate Resource On Solana Outages And DDoS Attacks
How Jessica Simpson Almost Lost Her Name And Her Billion Dollar Empire
Sidney Poitier, Actor Who Made Oscars History, Dies At 94
Green Comet Will Be Visible As It Passes By Earth For First Time In 50,000 Years
FTX (SBF) Got Approval From F.D.I.C., State Regulators And Federal Reserve To Buy Tiny Bank!!!
Joe Rogan: I Have A Lot Of Hope For Bitcoin
Teen Cyber Prodigy Stumbled Onto Flaw Letting Him Hijack Teslas
Spyware Finally Got Scary Enough To Freak Lawmakers Out—After It Spied On Them
The First Nuclear-Powered Bitcoin Mine Is Here. Maybe It Can Clean Up Energy FUD
The World’s Best Crypto Policies: How They Do It In 37 Nations
Tonga To Copy El Salvador’s Bill Making Bitcoin Legal Tender, Says Former MP
Wordle Is The New “Lingo” Turning Fans Into Argumentative Strategy Nerds
Prospering In The Pandemic, Some Feel Financial Guilt And Gratitude
Is Art Therapy The Path To Mental Well-Being?
New York, California, New Jersey, And Alabama Move To Ban ‘Forever Chemicals’ In Firefighting Foam
The Mystery Of The Wasting House-Cats
What Pet Owners Should Know About Chronic Kidney Disease In Dogs And Cats
Pets Score Company Perks As The ‘New Dependents’
Why Is My Cat Rubbing His Face In Ants?
Natural Cure For Hyperthyroidism In Cats Including How To Switch Him/Her To A Raw Food Diet
Ultimate Resource For Cat Lovers
FDA Approves First-Ever Arthritis Pain Management Drug For Cats
Ultimate Resource On Duke of York’s Prince Andrew And His Sex Scandal
Walmart Filings Reveal Plans To Create Cryptocurrency, NFTs
Bitcoin’s Dominance of Crypto Payments Is Starting To Erode
T-Mobile Says Hackers Stole Data On About 37 Million Customers
Jack Dorsey Announces Bitcoin Legal Defense Fund
More Than 100 Millionaires Signed An Open Letter Asking To Be Taxed More Heavily
Federal Regulator Says Credit Unions Can Partner With Crypto Providers
What’s Behind The Fascination With Smash-And-Grab Shoplifting?
Train Robberies Are A Problem In Los Angeles, And No One Agrees On How To Stop Them
US Stocks Historically Deliver Strong Gains In Fed Hike Cycles (GotBitcoin)
Ian Alexander Jr., Only Child of Regina King, Dies At Age 26
Amazon Ends Its Charity Donation Program Amazonsmile After Other Cost-Cutting Efforts
Indexing Is Coming To Crypto Funds Via Decentralized Exchanges
Doctors Show Implicit Bias Towards Black Patients
Darkmail Pushes Privacy Into The Hands Of NSA-Weary Customers
3D Printing Make Anything From Candy Bars To Hand Guns
Stealing The Blood Of The Young May Make You More Youthful
Henrietta Lacks And Her Remarkable Cells Will Finally See Some Payback
AL_A Wins Approval For World’s First Magnetized Fusion Power Plant
Want To Be Rich? Bitcoin’s Limited Supply Cap Means You Only Need 0.01 BTC
Smart Money Is Buying Bitcoin Dip. Stocks, Not So Much
McDonald’s Jumps On Bitcoin Memewagon, Crypto Twitter Responds
America COMPETES Act Would Be Disastrous For Bitcoin Cryptocurrency And More
Lyn Alden On Bitcoin, Inflation And The Potential Coming Energy Shock
Inflation And A Tale of Cantillionaires
El Salvador Plans Bill To Adopt Bitcoin As Legal Tender
Miami Mayor Says City Employees Should Be Able To Take Their Salaries In Bitcoin
Vast Troves of Classified Info Undermine National Security, Spy Chief Says
BREAKING: Arizona State Senator Introduces Bill To Make Bitcoin Legal Tender
San Francisco’s Historic Surveillance Law May Get Watered Down
How Bitcoin Contributions Funded A $1.4M Solar Installation In Zimbabwe
California Lawmaker Says National Privacy Law Is a Priority
The Pandemic Turbocharged Online Privacy Concerns
How To Protect Your Online Privacy While Working From Home
Researchers Use GPU Fingerprinting To Track Users Online
Japan’s $1 Trillion Crypto Market May Ease Onerous Listing Rules
Ultimate Resource On A Weak / Strong Dollar’s Impact On Bitcoin
Fed Money Printer Goes Into Reverse (Quantitative Tightening): What Does It Mean For Crypto?
Crypto Market Is Closer To A Bottom Than Stocks (#GotBitcoin)
When World’s Central Banks Get It Wrong, Guess Who Pays The Price😂😹🤣 (#GotBitcoin)
“Better Days Ahead With Crypto Deleveraging Coming To An End” — Joker
Crypto Funds Have Seen Record Investment Inflow In Recent Weeks
Bitcoin’s Epic Run Is Winning More Attention On Wall Street
Ultimate Resource For Crypto Mergers And Acquisitions (M&A) (#GotBitcoin)
Why Wall Street Is Literally Salivating Over Bitcoin
Nasdaq-Listed MicroStrategy And Others Wary Of Looming Dollar Inflation, Turns To Bitcoin And Gold
Bitcoin For Corporations | Michael Saylor | Bitcoin Corporate Strategy
Ultimate Resource On Myanmar’s Involvement With Crypto-Currencies
‘I Cry Every Day’: Olympic Athletes Slam Food, COVID Tests And Conditions In Beijing
Does Your Baby’s Food Contain Toxic Metals? Here’s What Our Investigation Found
Ultimate Resource For Pro-Crypto Lobbying And Non-Profit Organizations
Ultimate Resource On BlockFi, Celsius And Nexo
Petition Calling For Resignation Of U.S. Securities/Exchange Commission Chair Gary Gensler
100 Million Americans Can Legally Bet on the Super Bowl. A Spot Bitcoin ETF? Forget About it!
Green Finance Isn’t Going Where It’s Needed
Shedding Some Light On The Murky World Of ESG Metrics
SEC Targets Greenwashers To Bring Law And Order To ESG
BlackRock (Assets Under Management $7.4 Trillion) CEO: Bitcoin Has Caught Our Attention
Canada’s Major Banks Go Offline In Mysterious (Bank Run?) Hours-Long Outage (#GotBitcoin)
On-Chain Data: A Framework To Evaluate Bitcoin
On Its 14th Birthday, Bitcoin’s 1,690,706,971% Gain Looks Kind of… Well Insane
The Most Important Health Metric Is Now At Your Fingertips
American Bargain Hunters Flock To A New Online Platform Forged In China
Why We Should Welcome Another Crypto Winter
Traders Prefer Gold, Fiat Safe Havens Over Bitcoin As Russia Goes To War
Music Distributor DistroKid Raises Money At $1.3 Billion Valuation
Nas Selling Rights To Two Songs Via Crypto Music Startup Royal
Ultimate Resource On Music Catalog Deals
Ultimate Resource On Music And NFTs And The Implications For The Entertainment Industry
Lead And Cadmium Could Be In Your Dark Chocolate
Catawba, Native-American Tribe Approves First Digital Economic Zone In The United States
The Miracle Of Blockchain’s Triple Entry Accounting
How And Why To Stimulate Your Vagus Nerve!
Housing Boom Brings A Shortage Of Land To Build New Homes
Biden Lays Out His Blueprint For Fair Housing
No Grave Dancing For Sam Zell Now. He’s Paying Up For Hot Properties
Cracks In The Housing Market Are Starting To Show
Ever-Growing Needs Strain U.S. Food Bank Operations
Food Pantry Helps Columbia Students Struggling To Pay Bills
Food Insecurity Driven By Climate Change Has Central Americans Fleeing To The U.S.
Housing Insecurity Is Now A Concern In Addition To Food Insecurity
Families Face Massive Food Insecurity Levels
US Troops Going Hungry (Food Insecurity) Is A National Disgrace
Everything You Should Know About Community Fridges, From Volunteering To Starting Your Own
Russia’s Independent Journalists Including Those Who Revealed The Pandora Papers Need Your Help
10 Women Who Used Crypto To Make A Difference In 2021
Happy International Women’s Day! Leaders Share Their Experiences In Crypto
Dollar On Course For Worst Performance In Over A Decade (#GotBitcoin)
Juice The Stock Market And Destroy The Dollar!! (#GotBitcoin)
Unusual Side Hustles You May Not Have Thought Of
Ultimate Resource On Global Inflation And Rising Interest Rates (#GotBitcoin)
The Fed Is Setting The Stage For Hyper-Inflation Of The Dollar (#GotBitcoin)
An Antidote To Inflation? ‘Buy Nothing’ Groups Gain Popularity
Why Is Bitcoin Dropping If It’s An ‘Inflation Hedge’?
Lyn Alden Talks Bitcoin, Inflation And The Potential Coming Energy Shock
Ultimate Resource On How Black Families Can Fight Against Rising Inflation (#GotBitcoin)
What The Fed’s Rate Hike Means For Inflation, Housing, Crypto And Stocks
Egyptians Buy Bitcoin Despite Prohibitive New Banking Laws
Archaeologists Uncover Five Tombs In Egypt’s Saqqara Necropolis
History of Alchemy From Ancient Egypt To Modern Times
Former World Bank Chief Didn’t Act On Warnings Of Sexual Harassment
Does Your Hospital or Doctor Have A Financial Relationship With Big Pharma?
Ultimate Resource Covering The Crisis Taking Place In The Nickel Market
Apple Along With Meta And Secret Service Agents Fooled By Law Enforcement Impersonators
Handy Tech That Can Support Your Fitness Goals
How To Naturally Increase Your White Blood Cell Count
Ultimate Source For Russians Oligarchs And The Impact Of Sanctions On Them
Ultimate Source For Bitcoin Price Manipulation By Wall Street
Russia, Sri Lanka And Lebanon’s Defaults Could Be The First Of Many (#GotBitcoin)
Will Community Group Buying Work In The US?
Building And Running Businesses In The ‘Spirit Of Bitcoin’
What Is The Mysterious Liver Disease Hurting (And Killing) Children?
Citigroup Trader Is Scapegoat For Flash Crash In European Stocks (#GotBitcoin)
Bird Flu Outbreak Approaches Worst Ever In U.S. With 37 Million Animals Dead
Financial Inequality Grouped By Race For Blacks, Whites And Hispanics
How Black Businesses Can Prosper From Targeting A Trillion-Dollar Black Culture Market (#GotBitcoin)
Ultimate Resource For Central Bank Digital Currencies (#GotBitcoin) Page#2
Meet The Crypto Angel Investor Running For Congress In Nevada (#GotBitcoin?)
Introducing BTCPay Vault – Use Any Hardware Wallet With BTCPay And Its Full Node (#GotBitcoin?)
How Not To Lose Your Coins In 2020: Alternative Recovery Methods (#GotBitcoin?)
H.R.5635 – Virtual Currency Tax Fairness Act of 2020 ($200.00 Limit) 116th Congress (2019-2020)
Adam Back On Satoshi Emails, Privacy Concerns And Bitcoin’s Early Days
The Prospect of Using Bitcoin To Build A New International Monetary System Is Getting Real
How To Raise Funds For Australia Wildfire Relief Efforts (Using Bitcoin And/Or Fiat )
Former Regulator Known As ‘Crypto Dad’ To Launch Digital-Dollar Think Tank (#GotBitcoin?)
Currency ‘Cold War’ Takes Center Stage At Pre-Davos Crypto Confab (#GotBitcoin?)
A Blockchain-Secured Home Security Camera Won Innovation Awards At CES 2020 Las Vegas
Bitcoin’s Had A Sensational 11 Years (#GotBitcoin?)
Sergey Nazarov And The Creation Of A Decentralized Network Of Oracles
Google Suspends MetaMask From Its Play App Store, Citing “Deceptive Services”
Christmas Shopping: Where To Buy With Crypto This Festive Season
At 8,990,000% Gains, Bitcoin Dwarfs All Other Investments This Decade
Coinbase CEO Armstrong Wins Patent For Tech Allowing Users To Email Bitcoin
Bitcoin Has Got Society To Think About The Nature Of Money
How DeFi Goes Mainstream In 2020: Focus On Usability (#GotBitcoin?)
Dissidents And Activists Have A Lot To Gain From Bitcoin, If Only They Knew It (#GotBitcoin?)
At A Refugee Camp In Iraq, A 16-Year-Old Syrian Is Teaching Crypto Basics
Bitclub Scheme Busted In The US, Promising High Returns From Mining
Bitcoin Advertised On French National TV
Germany: New Proposed Law Would Legalize Banks Holding Bitcoin
How To Earn And Spend Bitcoin On Black Friday 2019
The Ultimate List of Bitcoin Developments And Accomplishments
Charities Put A Bitcoin Twist On Giving Tuesday
Family Offices Finally Accept The Benefits of Investing In Bitcoin
An Army Of Bitcoin Devs Is Battle-Testing Upgrades To Privacy And Scaling
Bitcoin ‘Carry Trade’ Can Net Annual Gains With Little Risk, Says PlanB
Max Keiser: Bitcoin’s ‘Self-Settlement’ Is A Revolution Against Dollar
Blockchain Can And Will Replace The IRS
China Seizes The Blockchain Opportunity. How Should The US Respond? (#GotBitcoin?)
Jack Dorsey: You Can Buy A Fraction Of Berkshire Stock Or ‘Stack Sats’
Bitcoin Price Skyrockets $500 In Minutes As Bakkt BTC Contracts Hit Highs
Bitcoin’s Irreversibility Challenges International Private Law: Legal Scholar
Bitcoin Has Already Reached 40% Of Average Fiat Currency Lifespan
Yes, Even Bitcoin HODLers Can Lose Money In The Long-Term: Here’s How (#GotBitcoin?)
Unicef To Accept Donations In Bitcoin (#GotBitcoin?)
Former Prosecutor Asked To “Shut Down Bitcoin” And Is Now Face Of Crypto VC Investing (#GotBitcoin?)
Switzerland’s ‘Crypto Valley’ Is Bringing Blockchain To Zurich
Next Bitcoin Halving May Not Lead To Bull Market, Says Bitmain CEO
Bitcoin Developer Amir Taaki, “We Can Crash National Economies” (#GotBitcoin?)
Veteran Crypto And Stocks Trader Shares 6 Ways To Invest And Get Rich
Is Chainlink Blazing A Trail Independent Of Bitcoin?
Nearly $10 Billion In BTC Is Held In Wallets Of 8 Crypto Exchanges (#GotBitcoin?)
SEC Enters Settlement Talks With Alleged Fraudulent Firm Veritaseum (#GotBitcoin?)
Blockstream’s Samson Mow: Bitcoin’s Block Size Already ‘Too Big’
Attorneys Seek Bank Of Ireland Execs’ Testimony Against OneCoin Scammer (#GotBitcoin?)
OpenLibra Plans To Launch Permissionless Fork Of Facebook’s Stablecoin (#GotBitcoin?)
Tiny $217 Options Trade On Bitcoin Blockchain Could Be Wall Street’s Death Knell (#GotBitcoin?)
Class Action Accuses Tether And Bitfinex Of Market Manipulation (#GotBitcoin?)
Sharia Goldbugs: How ISIS Created A Currency For World Domination (#GotBitcoin?)
Bitcoin Eyes Demand As Hong Kong Protestors Announce Bank Run (#GotBitcoin?)
How To Securely Transfer Crypto To Your Heirs
‘Gold-Backed’ Crypto Token Promoter Karatbars Investigated By Florida Regulators (#GotBitcoin?)
Crypto News From The Spanish-Speaking World (#GotBitcoin?)
Financial Services Giant Morningstar To Offer Ratings For Crypto Assets (#GotBitcoin?)
‘Gold-Backed’ Crypto Token Promoter Karatbars Investigated By Florida Regulators (#GotBitcoin?)
The Original Sins Of Cryptocurrencies (#GotBitcoin?)
Bitcoin Is The Fraud? JPMorgan Metals Desk Fixed Gold Prices For Years (#GotBitcoin?)
Israeli Startup That Allows Offline Crypto Transactions Secures $4M (#GotBitcoin?)
[PSA] Non-genuine Trezor One Devices Spotted (#GotBitcoin?)
Bitcoin Stronger Than Ever But No One Seems To Care: Google Trends (#GotBitcoin?)
First-Ever SEC-Qualified Token Offering In US Raises $23 Million (#GotBitcoin?)
You Can Now Prove A Whole Blockchain With One Math Problem – Really
Crypto Mining Supply Fails To Meet Market Demand In Q2: TokenInsight
$2 Billion Lost In Mt. Gox Bitcoin Hack Can Be Recovered, Lawyer Claims (#GotBitcoin?)
Fed Chair Says Agency Monitoring Crypto But Not Developing Its Own (#GotBitcoin?)
Wesley Snipes Is Launching A Tokenized $25 Million Movie Fund (#GotBitcoin?)
Mystery 94K BTC Transaction Becomes Richest Non-Exchange Address (#GotBitcoin?)
A Crypto Fix For A Broken International Monetary System (#GotBitcoin?)
Four Out Of Five Top Bitcoin QR Code Generators Are Scams: Report (#GotBitcoin?)
Waves Platform And The Abyss To Jointly Launch Blockchain-Based Games Marketplace (#GotBitcoin?)
Bitmain Ramps Up Power And Efficiency With New Bitcoin Mining Machine (#GotBitcoin?)
Ledger Live Now Supports Over 1,250 Ethereum-Based ERC-20 Tokens (#GotBitcoin?)
Miss Finland: Bitcoin’s Risk Keeps Most Women Away From Cryptocurrency (#GotBitcoin?)
Artist Akon Loves BTC And Says, “It’s Controlled By The People” (#GotBitcoin?)
Ledger Live Now Supports Over 1,250 Ethereum-Based ERC-20 Tokens (#GotBitcoin?)
Co-Founder Of LinkedIn Presents Crypto Rap Video: Hamilton Vs. Satoshi (#GotBitcoin?)
Crypto Insurance Market To Grow, Lloyd’s Of London And Aon To Lead (#GotBitcoin?)
No ‘AltSeason’ Until Bitcoin Breaks $20K, Says Hedge Fund Manager (#GotBitcoin?)
NSA Working To Develop Quantum-Resistant Cryptocurrency: Report (#GotBitcoin?)
Custody Provider Legacy Trust Launches Crypto Pension Plan (#GotBitcoin?)
Vaneck, SolidX To Offer Limited Bitcoin ETF For Institutions Via Exemption (#GotBitcoin?)
Russell Okung: From NFL Superstar To Bitcoin Educator In 2 Years (#GotBitcoin?)
Bitcoin Miners Made $14 Billion To Date Securing The Network (#GotBitcoin?)
Why Does Amazon Want To Hire Blockchain Experts For Its Ads Division?
Argentina’s Economy Is In A Technical Default (#GotBitcoin?)
Blockchain-Based Fractional Ownership Used To Sell High-End Art (#GotBitcoin?)
Portugal Tax Authority: Bitcoin Trading And Payments Are Tax-Free (#GotBitcoin?)
Bitcoin ‘Failed Safe Haven Test’ After 7% Drop, Peter Schiff Gloats (#GotBitcoin?)
Bitcoin Dev Reveals Multisig UI Teaser For Hardware Wallets, Full Nodes (#GotBitcoin?)
Bitcoin Price: $10K Holds For Now As 50% Of CME Futures Set To Expire (#GotBitcoin?)
Bitcoin Realized Market Cap Hits $100 Billion For The First Time (#GotBitcoin?)
Stablecoins Begin To Look Beyond The Dollar (#GotBitcoin?)
Bank Of England Governor: Libra-Like Currency Could Replace US Dollar (#GotBitcoin?)
Binance Reveals ‘Venus’ — Its Own Project To Rival Facebook’s Libra (#GotBitcoin?)
The Real Benefits Of Blockchain Are Here. They’re Being Ignored (#GotBitcoin?)
CommBank Develops Blockchain Market To Boost Biodiversity (#GotBitcoin?)
SEC Approves Blockchain Tech Startup Securitize To Record Stock Transfers (#GotBitcoin?)
SegWit Creator Introduces New Language For Bitcoin Smart Contracts (#GotBitcoin?)
You Can Now Earn Bitcoin Rewards For Postmates Purchases (#GotBitcoin?)
Bitcoin Price ‘Will Struggle’ In Big Financial Crisis, Says Investor (#GotBitcoin?)
Fidelity Charitable Received Over $100M In Crypto Donations Since 2015 (#GotBitcoin?)
Would Blockchain Better Protect User Data Than FaceApp? Experts Answer (#GotBitcoin?)
Just The Existence Of Bitcoin Impacts Monetary Policy (#GotBitcoin?)
What Are The Biggest Alleged Crypto Heists And How Much Was Stolen? (#GotBitcoin?)
IRS To Cryptocurrency Owners: Come Clean, Or Else!
Coinbase Accidentally Saves Unencrypted Passwords Of 3,420 Customers (#GotBitcoin?)
Bitcoin Is A ‘Chaos Hedge, Or Schmuck Insurance‘ (#GotBitcoin?)
Bakkt Announces September 23 Launch Of Futures And Custody
Coinbase CEO: Institutions Depositing $200-400M Into Crypto Per Week (#GotBitcoin?)
Researchers Find Monero Mining Malware That Hides From Task Manager (#GotBitcoin?)
Crypto Dusting Attack Affects Nearly 300,000 Addresses (#GotBitcoin?)
A Case For Bitcoin As Recession Hedge In A Diversified Investment Portfolio (#GotBitcoin?)
SEC Guidance Gives Ammo To Lawsuit Claiming XRP Is Unregistered Security (#GotBitcoin?)
15 Countries To Develop Crypto Transaction Tracking System: Report (#GotBitcoin?)
US Department Of Commerce Offering 6-Figure Salary To Crypto Expert (#GotBitcoin?)
Mastercard Is Building A Team To Develop Crypto, Wallet Projects (#GotBitcoin?)
Canadian Bitcoin Educator Scams The Scammer And Donates Proceeds (#GotBitcoin?)
Amazon Wants To Build A Blockchain For Ads, New Job Listing Shows (#GotBitcoin?)
Shield Bitcoin Wallets From Theft Via Time Delay (#GotBitcoin?)
Blockstream Launches Bitcoin Mining Farm With Fidelity As Early Customer (#GotBitcoin?)
Commerzbank Tests Blockchain Machine To Machine Payments With Daimler (#GotBitcoin?)
Man Takes Bitcoin Miner Seller To Tribunal Over Electricity Bill And Wins (#GotBitcoin?)
Bitcoin’s Computing Power Sets Record As Over 100K New Miners Go Online (#GotBitcoin?)
Walmart Coin And Libra Perform Major Public Relations For Bitcoin (#GotBitcoin?)
Judge Says Buying Bitcoin Via Credit Card Not Necessarily A Cash Advance (#GotBitcoin?)
Poll: If You’re A Stockowner Or Crypto-Currency Holder. What Will You Do When The Recession Comes?
1 In 5 Crypto Holders Are Women, New Report Reveals (#GotBitcoin?)
Beating Bakkt, Ledgerx Is First To Launch ‘Physical’ Bitcoin Futures In Us (#GotBitcoin?)
Facebook Warns Investors That Libra Stablecoin May Never Launch (#GotBitcoin?)
Government Money Printing Is ‘Rocket Fuel’ For Bitcoin (#GotBitcoin?)
Bitcoin-Friendly Square Cash App Stock Price Up 56% In 2019 (#GotBitcoin?)
Safeway Shoppers Can Now Get Bitcoin Back As Change At 894 US Stores (#GotBitcoin?)
TD Ameritrade CEO: There’s ‘Heightened Interest Again’ With Bitcoin (#GotBitcoin?)
Venezuela Sets New Bitcoin Volume Record Thanks To 10,000,000% Inflation (#GotBitcoin?)
Newegg Adds Bitcoin Payment Option To 73 More Countries (#GotBitcoin?)
China’s Schizophrenic Relationship With Bitcoin (#GotBitcoin?)
More Companies Build Products Around Crypto Hardware Wallets (#GotBitcoin?)
Bakkt Is Scheduled To Start Testing Its Bitcoin Futures Contracts Today (#GotBitcoin?)
Bitcoin Network Now 8 Times More Powerful Than It Was At $20K Price (#GotBitcoin?)
Crypto Exchange BitMEX Under Investigation By CFTC: Bloomberg (#GotBitcoin?)
“Bitcoin An ‘Unstoppable Force,” Says US Congressman At Crypto Hearing (#GotBitcoin?)
Bitcoin Network Is Moving $3 Billion Daily, Up 210% Since April (#GotBitcoin?)
Cryptocurrency Startups Get Partial Green Light From Washington
Fundstrat’s Tom Lee: Bitcoin Pullback Is Healthy, Fewer Searches Аre Good (#GotBitcoin?)
Bitcoin Lightning Nodes Are Snatching Funds From Bad Actors (#GotBitcoin?)
The Provident Bank Now Offers Deposit Services For Crypto-Related Entities (#GotBitcoin?)
Bitcoin Could Help Stop News Censorship From Space (#GotBitcoin?)
US Sanctions On Iran Crypto Mining — Inevitable Or Impossible? (#GotBitcoin?)
US Lawmaker Reintroduces ‘Safe Harbor’ Crypto Tax Bill In Congress (#GotBitcoin?)
EU Central Bank Won’t Add Bitcoin To Reserves — Says It’s Not A Currency (#GotBitcoin?)
The Miami Dolphins Now Accept Bitcoin And Litecoin Crypt-Currency Payments (#GotBitcoin?)
Trump Bashes Bitcoin And Alt-Right Is Mad As Hell (#GotBitcoin?)
Goldman Sachs Ramps Up Development Of New Secret Crypto Project (#GotBitcoin?)
Blockchain And AI Bond, Explained (#GotBitcoin?)
Grayscale Bitcoin Trust Outperformed Indexes In First Half Of 2019 (#GotBitcoin?)
XRP Is The Worst Performing Major Crypto Of 2019 (GotBitcoin?)
Bitcoin Back Near $12K As BTC Shorters Lose $44 Million In One Morning (#GotBitcoin?)
As Deutsche Bank Axes 18K Jobs, Bitcoin Offers A ‘Plan ฿”: VanEck Exec (#GotBitcoin?)
Argentina Drives Global LocalBitcoins Volume To Highest Since November (#GotBitcoin?)
‘I Would Buy’ Bitcoin If Growth Continues — Investment Legend Mobius (#GotBitcoin?)
Lawmakers Push For New Bitcoin Rules (#GotBitcoin?)
Facebook’s Libra Is Bad For African Americans (#GotBitcoin?)
Crypto Firm Charity Announces Alliance To Support Feminine Health (#GotBitcoin?)
Canadian Startup Wants To Upgrade Millions Of ATMs To Sell Bitcoin (#GotBitcoin?)
Trump Says US ‘Should Match’ China’s Money Printing Game (#GotBitcoin?)
Casa Launches Lightning Node Mobile App For Bitcoin Newbies (#GotBitcoin?)
Bitcoin Rally Fuels Market In Crypto Derivatives (#GotBitcoin?)
World’s First Zero-Fiat ‘Bitcoin Bond’ Now Available On Bloomberg Terminal (#GotBitcoin?)
Buying Bitcoin Has Been Profitable 98.2% Of The Days Since Creation (#GotBitcoin?)
Another Crypto Exchange Receives License For Crypto Futures
From ‘Ponzi’ To ‘We’re Working On It’ — BIS Chief Reverses Stance On Crypto (#GotBitcoin?)
These Are The Cities Googling ‘Bitcoin’ As Interest Hits 17-Month High (#GotBitcoin?)
Venezuelan Explains How Bitcoin Saves His Family (#GotBitcoin?)
Quantum Computing Vs. Blockchain: Impact On Cryptography
This Fund Is Riding Bitcoin To Top (#GotBitcoin?)
Bitcoin’s Surge Leaves Smaller Digital Currencies In The Dust (#GotBitcoin?)
Bitcoin Exchange Hits $1 Trillion In Trading Volume (#GotBitcoin?)
Bitcoin Breaks $200 Billion Market Cap For The First Time In 17 Months (#GotBitcoin?)
You Can Now Make State Tax Payments In Bitcoin (#GotBitcoin?)
Religious Organizations Make Ideal Places To Mine Bitcoin (#GotBitcoin?)
Goldman Sacs And JP Morgan Chase Finally Concede To Crypto-Currencies (#GotBitcoin?)
Bitcoin Heading For Fifth Month Of Gains Despite Price Correction (#GotBitcoin?)
Breez Reveals Lightning-Powered Bitcoin Payments App For IPhone (#GotBitcoin?)
Big Four Auditing Firm PwC Releases Cryptocurrency Auditing Software (#GotBitcoin?)
Amazon-Owned Twitch Quietly Brings Back Bitcoin Payments (#GotBitcoin?)
JPMorgan Will Pilot ‘JPM Coin’ Stablecoin By End Of 2019: Report (#GotBitcoin?)
Is There A Big Short In Bitcoin? (#GotBitcoin?)
Coinbase Hit With Outage As Bitcoin Price Drops $1.8K In 15 Minutes
Samourai Wallet Releases Privacy-Enhancing CoinJoin Feature (#GotBitcoin?)
There Are Now More Than 5,000 Bitcoin ATMs Around The World (#GotBitcoin?)
You Can Now Get Bitcoin Rewards When Booking At Hotels.Com (#GotBitcoin?)
North America’s Largest Solar Bitcoin Mining Farm Coming To California (#GotBitcoin?)
Bitcoin On Track For Best Second Quarter Price Gain On Record (#GotBitcoin?)
Bitcoin Hash Rate Climbs To New Record High Boosting Network Security (#GotBitcoin?)
Bitcoin Exceeds 1Million Active Addresses While Coinbase Custodies $1.3B In Assets
Why Bitcoin’s Price Suddenly Surged Back $5K (#GotBitcoin?)
Zebpay Becomes First Exchange To Add Lightning Payments For All Users (#GotBitcoin?)
Coinbase’s New Customer Incentive: Interest Payments, With A Crypto Twist (#GotBitcoin?)
The Best Bitcoin Debit (Cashback) Cards Of 2019 (#GotBitcoin?)
Real Estate Brokerages Now Accepting Bitcoin (#GotBitcoin?)
Ernst & Young Introduces Tax Tool For Reporting Cryptocurrencies (#GotBitcoin?)
Recession Is Looming, or Not. Here’s How To Know (#GotBitcoin?)
How Will Bitcoin Behave During A Recession? (#GotBitcoin?)
Many U.S. Financial Officers Think a Recession Will Hit Next Year (#GotBitcoin?)
Definite Signs of An Imminent Recession (#GotBitcoin?)
What A Recession Could Mean for Women’s Unemployment (#GotBitcoin?)
Investors Run Out of Options As Bitcoin, Stocks, Bonds, Oil Cave To Recession Fears (#GotBitcoin?)
Goldman Is Looking To Reduce “Marcus” Lending Goal On Credit (Recession) Caution (#GotBitcoin?)

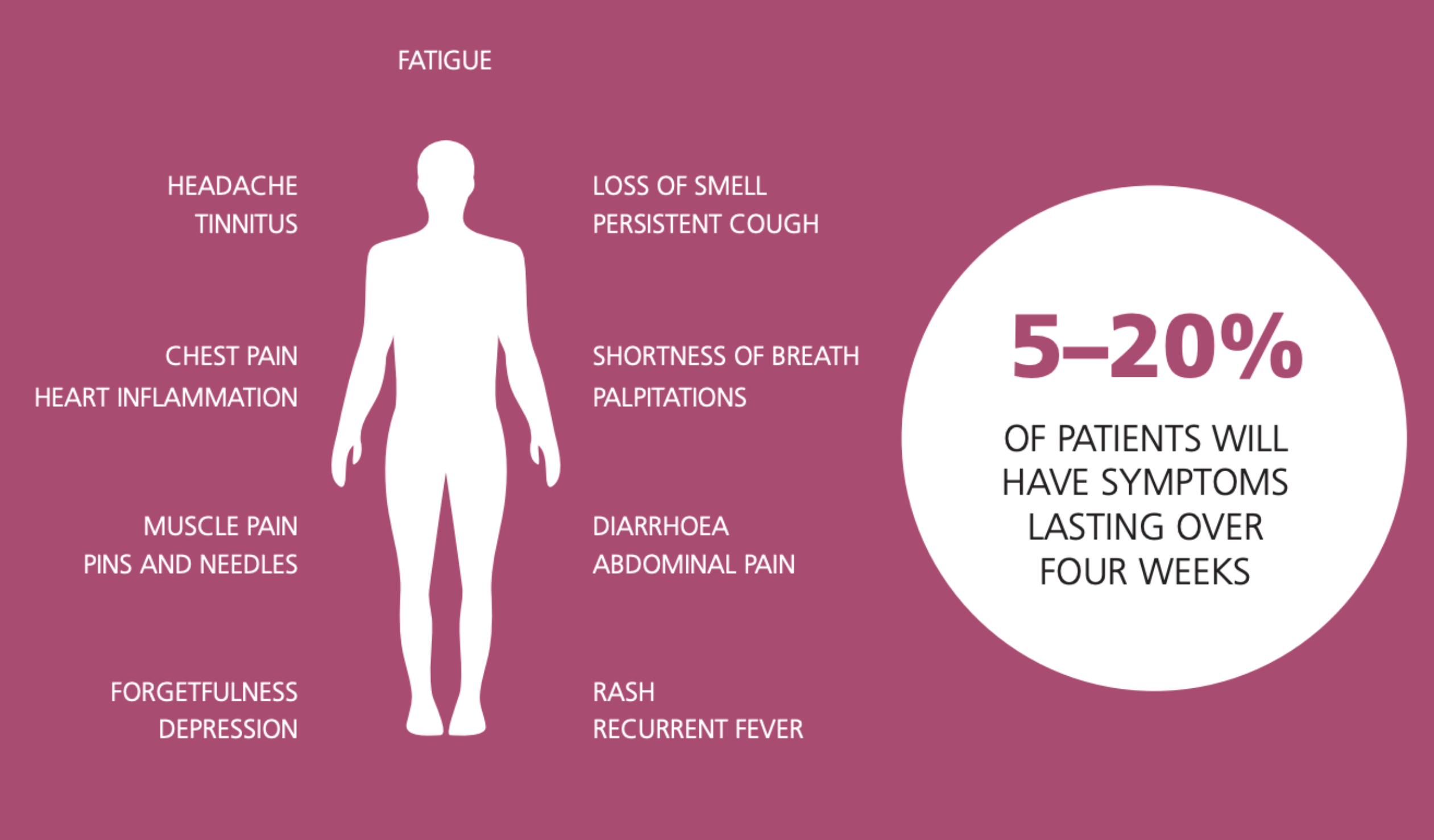
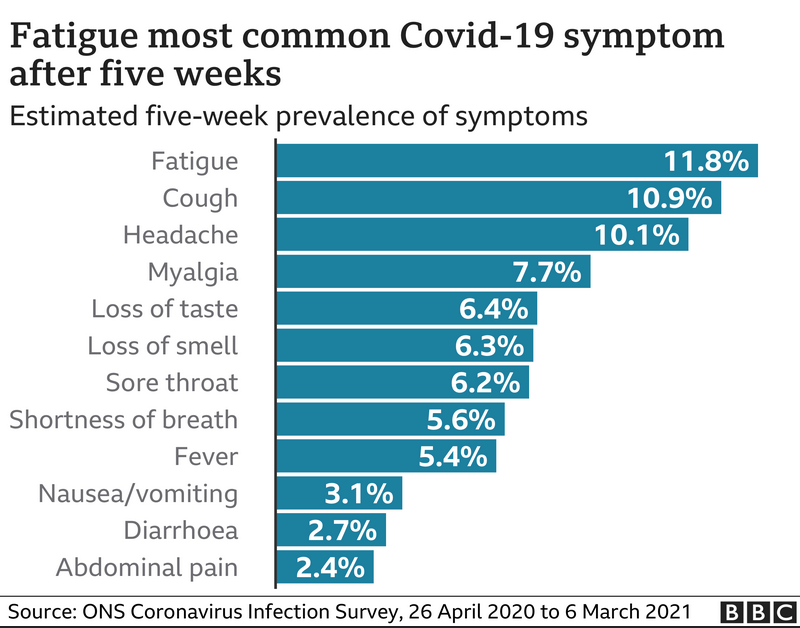
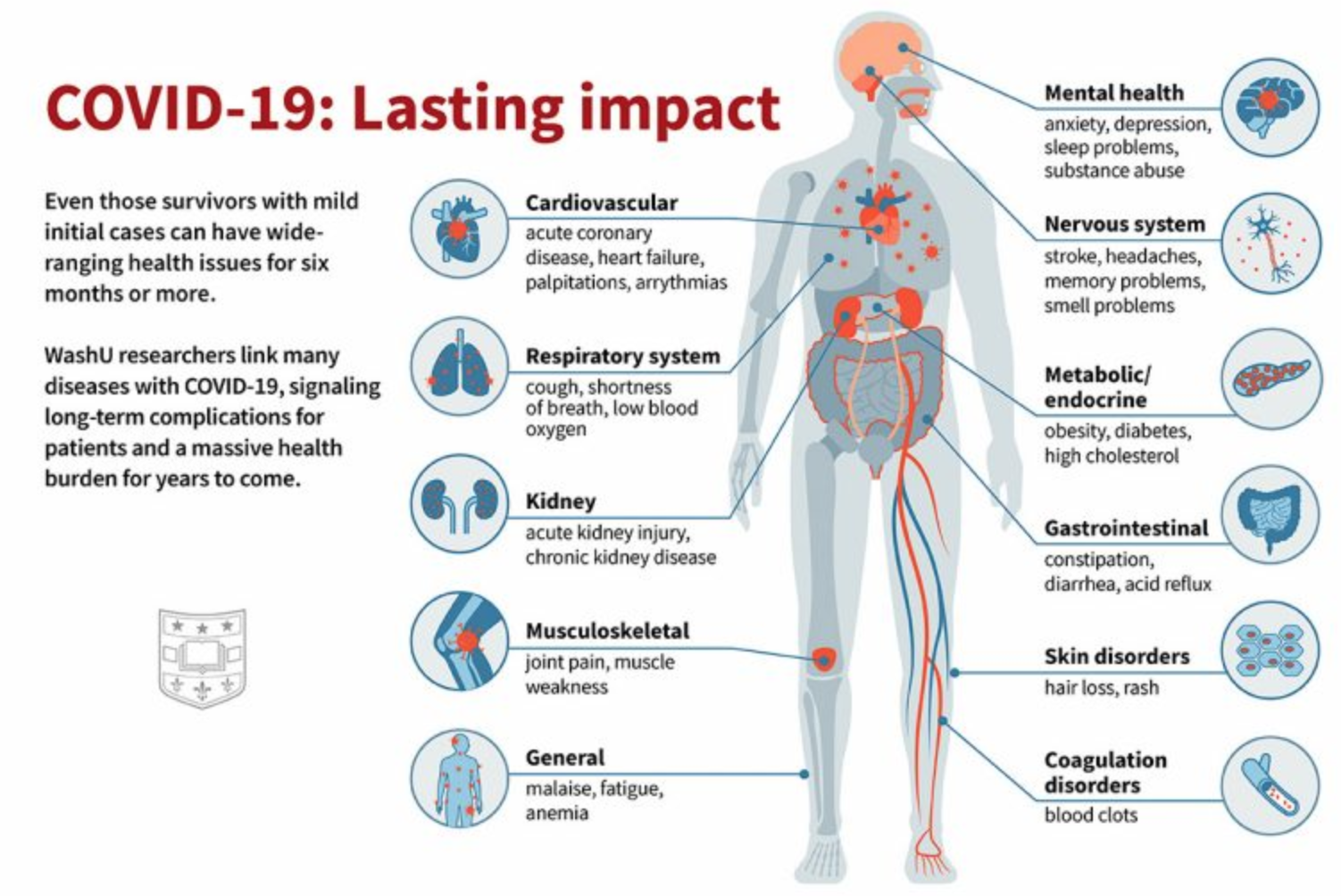
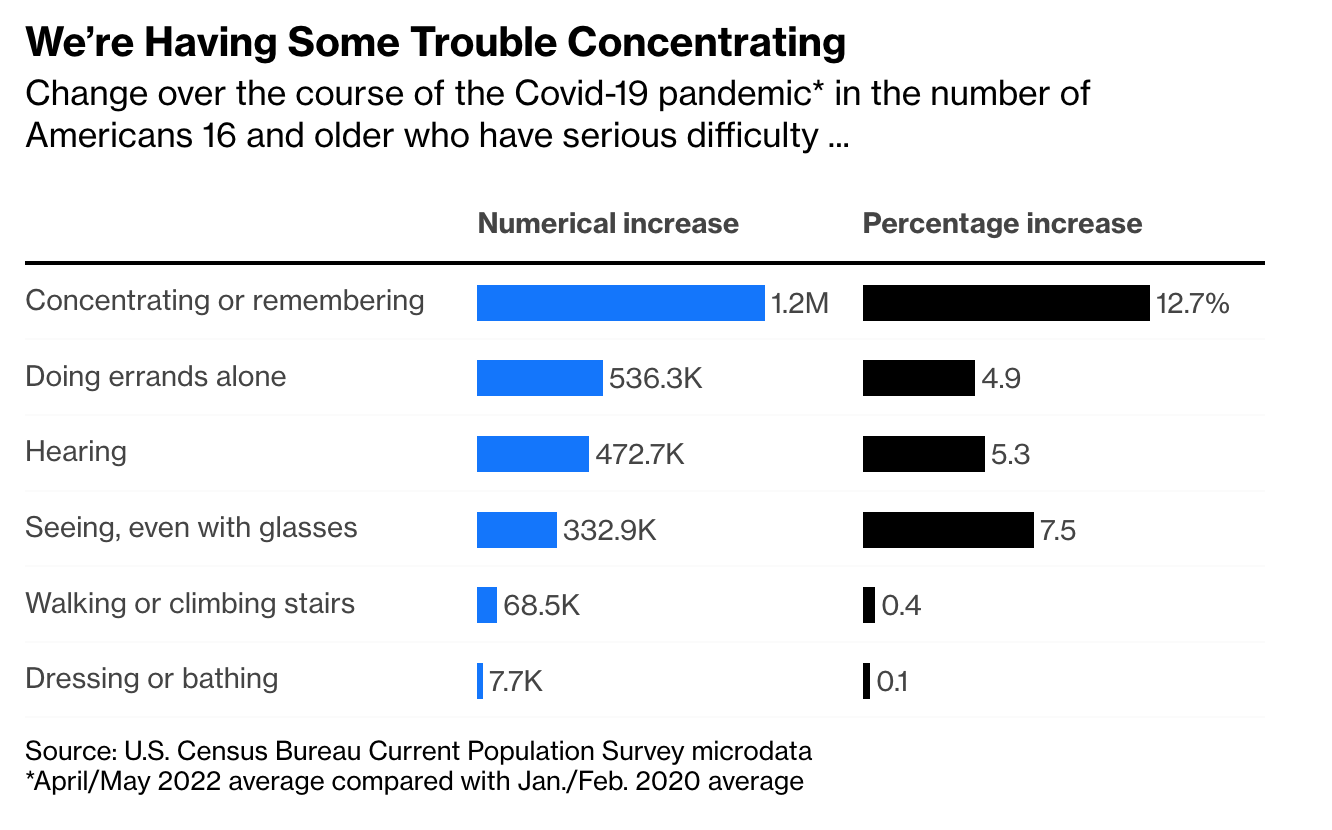
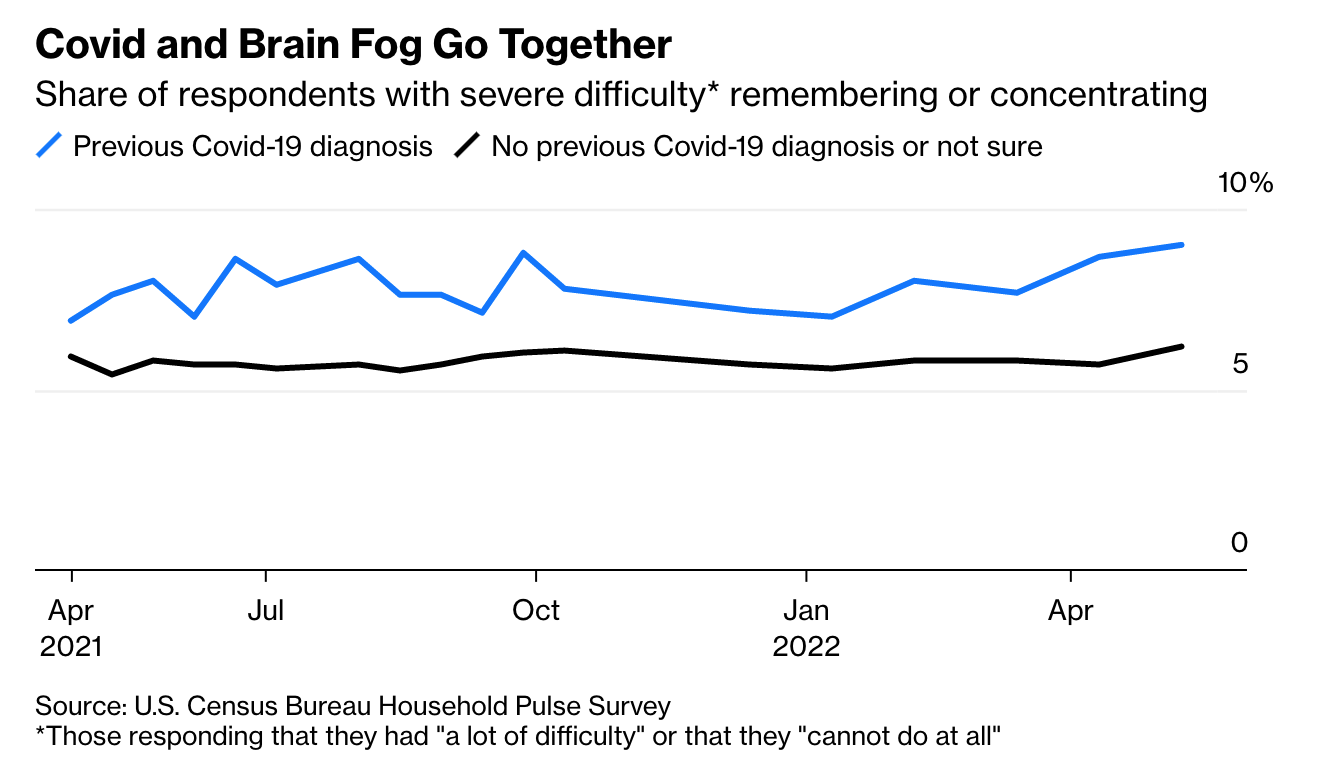
Leave a Reply
You must be logged in to post a comment.