Medical Tourism AKA The Globalization Of Healthcare
Medical tourism refers to people traveling to a country other than their own to obtain medical treatment. Medical Tourism AKA The Globalization Of Healthcare
In the past this usually referred to those who traveled from less-developed countries to major medical centers in highly developed countries for treatment unavailable at home.
However, in recent years it may equally refer to those from developed countries who travel to developing countries for lower priced medical treatments. The motivation may be also for medical services unavailable or illegal in the home country.
Related:
The Skin’s Circadian Rhythm: Skin Hydration Ebbs And Flows By The Clock
The Complete Guide To The Science Of Circadian Rhythms
Ultimate Resource For News, Breakthroughs And Innovations In Healthcare
Chrono-Pharmacology Reveals That “When” You Take Your Medication Can Make A Life-Saving Difference
10 Innovations Of 2022 That Allow Patients To Take Back Control
The Benefits of Grounding or Earthing For Improved Health (Dramatically Reduces Inflammation)
As Suicide Rates Rise, Scientists Find New Warning Signs
Next Target for Hackers in 2022 Medical Data and Wireless Medical Devices
China Approves Use of Rhino, Tiger Parts For Medical Treatment And Research
Jarlsberg Cheese Offers Significant Bone & Heart-Health Benefits Thanks To Vitamin K2, Says Study
Medical tourism most often is for surgeries (cosmetic or otherwise) or similar treatments, though people also travel for dental tourism or fertility tourism. People with rare conditions may travel to countries where the treatment is better understood.
However, almost all types of health care are available, including psychiatry, alternative medicine, convalescent care, and even burial services.
Health tourism is a wider term for travel that focus on medical treatments and the use of healthcare services. It covers a wide field of health-oriented, tourism ranging from preventive and health-conductive treatment to rehabilitational and curative forms of travel. Wellness tourism is a related field.
The first recorded instance of people travelling for medical treatment dates back thousands of years to when Greek pilgrims traveled from the eastern Mediterranean to a small area in the Saronic Gulf called Epidauria. This territory was the sanctuary of the healing god Asklepios.
Spa towns and sanitaria were early forms of medical tourism. In 18th-century Europe patients visited spas because they were places with supposedly health-giving mineral waters, treating diseases from gout to liver disorders and bronchitis.
Description
Factors that have led to the increasing popularity of medical travel include the high cost of health care, long wait times for certain procedures, the ease and affordability of international travel, and improvements in both technology and standards of care in many countries.
The avoidance of waiting times is the leading factor for medical tourism from the UK, whereas in the US, the main reason is cheaper prices abroad.
Many surgery procedures performed in medical tourism destinations cost a fraction of the price they do in other countries. For example, in the United States, a liver transplant that may cost $300,000 USD, would generally cost about $91,000 USD in Taiwan.
A large draw to medical travel is convenience and speed. Countries that operate public health-care systems often have long wait times for certain operations, for example, an estimated 782,936 Canadian patients spent an average waiting time of 9.4 weeks on medical waiting lists in 2005.
Canada has also set waiting time benchmarks for non urgent medical procedures, including a 26-week waiting period for a hip replacement and a 16-week wait for cataract surgery.
In First World countries such as the United States, medical tourism has large growth prospects and potentially destabilizing implications.
A forecast by Deloitte Consulting published in August 2008 projected that medical tourism originating in the US could jump by a factor of ten over the next decade.
An estimated 750,000 Americans went abroad for health care in 2007, and the report estimated that 1.5 million would seek health care outside the US in 2008. The growth in medical tourism has the potential to cost US health care providers billions of dollars in lost revenue.
Health care has become so expensive in the United States that a growing number of Americans (and their employers) are finding it more cost efficient to fly across the globe for certain medical procedures.
The savings are so great — and the quality high enough — that a handful of American insurance companies are now encouraging the practice and covering the travel and treatment costs.
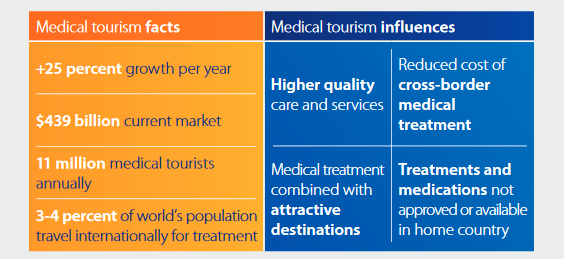
“Medical tourism” was valued at about $439 billion last year in a new report by Visa and Oxford Economics, which projected that it could grow 25 percent a year over the next decade. This year, an estimated 1.4 million Americans will leave the country for a medical procedure, according to Patients Beyond Borders.
In addition to traveling in order to save money, some medical tourists plan trips because they want to have a treatment that’s not approved in the United States or because they’ll have a shorter wait by going abroad.
If You’re Considering Joining Them, Here’s What You Need To Know:
1. The Potential Savings Are Huge. For patients considering procedures that aren’t covered by insurance, traveling abroad for treatment can yield serious savings.
A knee replacement, for example, which would cost $35,000 to $60,000 in the United States, costs less than $23,000 in Costa Rica or India, including airfare and lodging for the patient and a companion, according to Indus Health, which helps employers offer medical tourism benefits to their workers.
Other popular procedures for travelers include In vitro fertilization, dental work and cosmetic surgery.
Hospitals overseas can often charge lower prices because their doctors are paid less, and they may not have to carry the same medical malpractice insurance as American doctors. And if most patients are paying with cash, they don’t have to worry about tiered pricing for preferred insurance companies.
2. There Are Still Serious Risks. In addition to trouble arising from language barriers and culture shock, the standard safety practices in the United States may not be used in international hospitals. You may be more likely to receive counterfeit medications or blood that hasn’t been properly screened than you would here, according to the Centers for Disease Control.
Jet lag can also leave you weaker going into surgery or impede your recovery when you get home. If something goes seriously wrong, it may be more difficult to bring a malpractice suit against international health care providers, and even if you can bring a suit there are much lower limits to how much you can sue for internationally.
You also may not have the same privacy protections afforded to you in the United States under HIPAA rules.
3. Consider Medical Complications Insurance. If your traditional insurance won’t cover the trip, you may need to purchase medical complications insurance, which will cover the cost of follow-up care and treatment if your procedure results in complications. Traditional travel insurance typically doesn’t offer such coverage.
4. Do Your Homework. Look for a hospital that’s used to handling international patients and that’s accredited by the American Association for Accreditation of Ambulatory Surgery Facilities or the Joint Commission International. You’ll want a doctor who speaks English and who went to medical school in a first-world country.
“The people who get into trouble are the ones that price shop and don’t pay attention to quality,” says Josef Woodman, chief executive officer of Patients Beyond Borders.
If that sounds like too much work, there are several medical tourism agencies now that will coordinate the trip and who have established relationships with specific doctors and hospitals.
You may pay slightly more for the procedure, but you’ll have someone you can call if any issues arrive during or after your treatment.
Check out online reviews and the Better Business Bureau to see whether an agency has a good reputation. The agencies often also sell complications insurance.
5. Plan For Your Recovery. Depending on your procedure, you may need to stay abroad for several weeks. Make sure that your hotel knows that you’ll be recovering from a medical treatment and can accommodate any special needs you might have.
Even if you’re feeling better, the CDC recommends that you not fly for at least 10 days after surgery due to the increased risk of blood clots. You should also avoid typical vacation activities like sunbathing, swimming or drinking alcohol.
Be sure to bring home all of your discharge papers from the hospital, as well as records for blood work, X-rays or other screenings.
“That way if you need follow-up care, you can bring those documents to a doctor who might have been reluctant to treat [and who] will have a roadmap and the confidence to go forward,” Woodman says.
6. Involve Your Doctor. You’ll want to consult with your current doctor before seeking treatment abroad. You may need her to provide medical records or consult with your international team, and you’ll also likely follow up with her for ongoing treatment or checkups after you return.
“Talk to your doctor before you leave about the surgeon you’ll be seeing, the devices used, the recovery time,” says Maria Burpee, senior vice president of special products with ArchimedicX, an international hospital search engine and booking tool. “Then they can go over it with you and make a plan with your doctor for follow up care.”
An authority at the Harvard Business School stated that “medical tourism is promoted much more heavily in the United Kingdom than in the United States”.
Additionally, some patients in some First World countries are finding that insurance either does not cover orthopedic surgery (such as knee or hip replacement) or limits the choice of the facility, surgeon, or prosthetics to be used.
Popular medical travel worldwide destinations include: Canada, Cuba, Costa Rica, Ecuador, India, Israel, Jordan, Malaysia, Mexico, Singapore, South Korea, Taiwan, Thailand, Turkey, United States.
Popular destinations for cosmetic surgery include: Argentina, Bolivia, Brazil, Colombia, Costa Rica, Cuba, Ecuador, Mexico, Turkey, Thailand and Ukraine.
According to the “Sociedad Boliviana de Cirugia Plastica y Reconstructiva”, more than 70% of middle and upper class women in the country have had some form of plastic surgery. Other destination countries include Belgium, Poland, Slovakia and South Africa.
Some people travel for assisted pregnancy, such as in-vitro fertilization, or surrogacy, or freezing embryos for retro-production.
However, perceptions of medical tourism are not always positive. In places like the US, which has high standards of quality, medical tourism is viewed as risky. In some parts of the world, wider political issues can influence where medical tourists will choose to seek out health care.
Health tourism providers have developed as intermediaries which unite potential medical tourists with provider hospitals and other organizations. Companies that focus on medical value travel typically provide nurse case managers to assist patients with pre- and post-travel medical issues. They may also help provide resources for follow-up care upon the patient’s return.
Circumvention tourism is also an area of medical tourism that has grown. Circumvention tourism is travel in order to access medical services that are legal in the destination country but illegal in the home country.
This can include travel for fertility treatments that aren’t yet approved in the home country, abortion, and doctor-assisted suicide. Abortion tourism can be found most commonly in Europe, where travel between countries is relatively simple.
Ireland and Poland, two European countries with highly restrictive abortion laws, have the highest rates of circumvention tourism. In Poland especially, it is estimated that each year nearly 7,000 women travel to the UK, where abortion services are free through the National Health Service.
There are also efforts being made by independent organizations and doctors, such as with Women on Waves, to help women circumvent draconian laws in order to access medical services. With Women on Waves, the organization uses a mobile clinic aboard a ship to provide medical abortions in international waters, where the law of the country whose flag is flown applies.
International Healthcare Accreditation
International healthcare accreditation is the process of certifying a level of quality for healthcare providers and programs across multiple countries.
International healthcare accreditation organizations certify a wide range of healthcare programs such as hospitals, primary care centers, medical transport, and ambulatory care services. There are a number of accreditation schemes available based in a number of different countries around the world.
The oldest international accrediting body is Accreditation Canada, formerly known as the Canadian Council on Health Services Accreditation, which accredited the Bermuda Hospital Board as soon as 1968. Since then, it has accredited hospitals and health service organizations in ten other countries.
JCI Gold Seal, An Example of International Hospital Standard Accreditation
In the United States, the accreditation group Joint Commission International (JCI) was formed in 1994 to provide international clients education and consulting services. Many international hospitals today see obtaining international accreditation as a way to attract American patients.
Joint Commission International is a relative of the Joint Commission in the United States. Both are US-style independent private sector not-for-profit organizations that develop nationally and internationally recognized procedures and standards to help improve patient care and safety.
They work with hospitals to help them meet Joint Commission standards for patient care and then accredit those hospitals meeting the standards.
A British scheme, QHA Trent Accreditation, is an active independent holistic accreditation scheme, as well as GCR.org which monitors the success metrics and standards of almost 500,000 medical clinics worldwide.
The different international healthcare accreditation schemes vary in quality, size, cost, intent and the skill and intensity of their marketing. They also vary in terms of cost to hospitals and healthcare institutions making use of them.
Increasingly, some hospitals are looking towards dual international accreditation, perhaps having both JCI to cover potential US clientele, and Accreditation Canada or QHA Trent. As a result of competition between clinics for American medical tourists, there have been initiatives to rank hospitals based on patient-reported metrics.
Risks
Medical tourism carries some risks that locally provided medical care either does not carry or carries to a much lesser degree.
Some countries, such as South Africa, or Thailand have very different infectious disease-related epidemiology to Europe and North America.
Exposure to diseases without having built up natural immunity can be a hazard for weakened individuals, specifically with respect to gastrointestinal diseases (e.g. hepatitis A, amoebic dysentery, paratyphoid) which could weaken progress and expose the patient to mosquito-transmitted diseases, influenza, and tuberculosis.
However, because in poor tropical nations diseases run the gamut, doctors seem to be more open to the possibility of considering any infectious disease, including HIV, TB, and typhoid, while there are cases in the West where patients were consistently misdiagnosed for years because such diseases are perceived to be “rare” in the West.
The quality of post-operative care can also vary dramatically, depending on the hospital and country, and may be different from US or European standards.
Also, traveling long distances soon after surgery can increase the risk of complications. Long flights and decreased mobility associated with window seats can predispose one towards developing deep vein thrombosis and potentially a pulmonary embolism.
Other vacation activities can be problematic as well — for example, scars may become darker and more noticeable if they are sunburned while healing.
Also, health facilities treating medical tourists may lack an adequate complaints policy to deal appropriately and fairly with complaints made by dissatisfied patients.
Differences in healthcare provider standards around the world have been recognised by the World Health Organization, and in 2004 it launched the World Alliance for Patient Safety.
This body assists hospitals and government around the world in setting patient safety policy and practices that can become particularly relevant when providing medical tourism services.
If there are complications, the patient may need to stay in the foreign country for longer than planned or if they have returned home, will not have easy access for follow up care.
Patients sometimes travel to another country to obtain medical procedures that doctors in their home country refuse to perform because they believed that the risks of the procedure outweigh the benefits.
Such patients may have difficulty getting insurance (whether public or private) to cover follow up medical costs should the feared complications indeed arise.
Legal Issues
Receiving medical care abroad may subject medical tourists to unfamiliar legal issues. The limited nature of litigation in various countries is a reason for accessbility of care overseas.
While some countries currently presenting themselves as attractive medical tourism destinations provide some form of legal remedies for medical malpractice, these legal avenues may be unappealing to the medical tourist.
Should problems arise, patients might not be covered by adequate personal insurance or might be unable to seek compensation via malpractice lawsuits.
Hospitals and/or doctors in some countries may be unable to pay the financial damages awarded by a court to a patient who has sued them, owing to the hospital and/or the doctor not possessing appropriate insurance cover and/or medical indemnity.
Issues can also arise for patients who seek out services that are illegal in their home country. In this case, some countries have the jurisdiction to prosecute their citizen once they have returned home, or in extreme cases extraterritorially arrest and prosecute.
In Ireland, especially, in the 1980s-90s there were cases of young rape victims who were banned from traveling to Europe to get legal abortions. Ultimately, Ireland’s Supreme Court overturned the ban; they and many other countries have since created “right to travel” amendments.
Ethical Issues
There can be major ethical issues around medical tourism. For example, the illegal purchase of organs and tissues for transplantation had been methodically documented and studied in countries such as India, China, Colombia and the Philippines. The Declaration of Istanbul distinguishes between ethically problematic “transplant tourism” and “travel for transplantation”.
Medical tourism may raise broader ethical issues for the countries in which it is promoted. For example, in India, some argue that a “policy of ‘medical tourism for the classes and health missions for the masses’ will lead to a deepening of the inequities” already embedded in the health care system.
In Thailand, in 2008 it was stated that, “Doctors in Thailand have become so busy with foreigners that Thai patients are having trouble getting care”.
Medical tourism centered on new technologies, such as stem cell treatments, is often criticized on grounds of fraud, blatant lack of scientific rationale and patient safety.
However, when pioneering advanced technologies, such as providing ‘unproven’ therapies to patients outside of regular clinical trials, it is often challenging to differentiate between acceptable medical innovation and unacceptable patient exploitation.
Employer-sponsored Health Care In The US
Some US employers have begun exploring medical travel programs as a way to cut employee health care costs. Such proposals have raised stormy debates between employers and trade unions representing workers, with one union stating that it deplored the “shocking new approach” of offering employees overseas treatment in return for a share of the company’s savings.
The unions also raise the issues of legal liability should something go wrong, and potential job losses in the US health care industry if treatment is outsourced.
Employers may offer incentives such as paying for air travel and waiving out-of-pocket expenses for care outside of the US. For example, in January 2008, Hannaford Bros., a supermarket chain based in Maine, began paying the entire medical bill for employees to travel to Singapore for hip and knee replacements, including travel for the patient and companion.
Medical travel packages can integrate with all types of health insurance, including limited benefit plans, preferred provider organizations and high deductible health plans.
In 2000, Blue Shield of California began the United States’ first cross-border health plan. Patients in California could travel to one of the three certified hospitals in Mexico for treatment under California Blue Shield.
In 2007, a subsidiary of BlueCross BlueShield of South Carolina, Companion Global Healthcare, teamed up with hospitals in Thailand, Singapore, Turkey, Ireland, Costa Rica and India.
A 2008 article in Fast Company discusses the globalization of healthcare and describes how various players in the US healthcare market have begun to explore it.
Resources:
Holistic Medicine Schools – Natural Healers
What Does Knee Surgery Cost? Few Know, and That’s a Problem (Healthcare Pricing)

Leave a Reply
You must be logged in to post a comment.