Opiate-Addicted Babies Are The New Crack Babies of 2025-26
Hospitals around the country are confronting an unsettling consequence of the prescription-pain-pill epidemic: a surge in the number of babies born dependent on drugs such as oxycodone. Opiate-Addicted Babies Are The New Crack Babies of 2025-26
Hospitals in Florida and elsewhere are grappling with the latest fallout from the epidemic of prescription-drug abuse: babies born addicted to painkillers. The newborns present new challenges for hospitals.
Related Articles:
Freedom of Information Act Document Reveals Antidepressant Drugs Are Less Effective Than Placebos
Short Sellers Bet On Opioid Fallout Sinking Drug Companies’ Stocks
Fentanyl’s New Foe: A Quick Test Strip That Can Prevent Overdoses (#GotBitcoin?)
Pharmaceuticals Found In Our Drinking Water!
What Do You Get When Legal Drug Dealers Peddle “Heroin-in-a-Pill” To It’s “Clientele”?
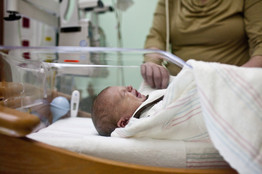
One recent morning a 12-day-old girl lay writhing in the neonatal intensive-care unit at Sarasota Memorial Hospital . Erin Weatherwax , a nurse, tried to console the newborn by holding her against her chest and patting the baby’s back.
She placed the girl in a motorized swing that made cricket sounds. But the infant continued to squirm, unable to sleep more than a few minutes at a time.
The baby suffered withdrawal from methadone, a drug used to treat painkiller addiction that her mother took during pregnancy. The hospital sated the baby’s physical cravings by giving her morphine as well as phenobarbital, a barbiturate used to treat seizures. Now she had to be weaned off those drugs.
Born Dependent on Opioids
Eight hours after Gabriel was born, he exhibited a variety of withdrawal symptoms, including stiffened muscles and excessive sucking.
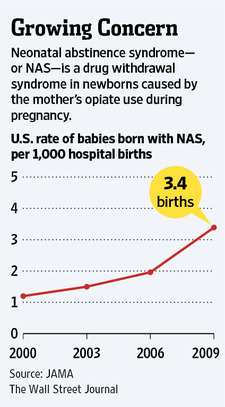
“It’s heartbreaking,” Ms. Weatherwax said. Between 2000 and 2009, the number of newborns showing symptoms of withdrawal from drugs called opioids–including painkillers like oxycodone and anti – addiction drugs such as methadone–tripled in the U.S., according to a study published earlier this year in the Journal of the American Medical Association.
In 2009, more than 13,000 babies in the U.S. were diagnosed with the condition, formally known as neonatal abstinence syndrome , the study said.
The newborns–reminiscent of the “crack babies” of the 1980s and 1990s born to women addicted to cocaine–present a host of challenges to hospitals. There is no standard way to treat their withdrawal, so doctors and nurses are improvising to figure out the most effective combination of drugs and dosages.
The babies require constant attention, and their stays in a neonatal intensive care unit, or NICU, can stretch for weeks, tying up hospital resources. Their treatment is costly–a mean of $53,400–according to the JAMA study, and Medicaid covers the tab for 78% of the babies. Hospital charges to care for such infants jumped to an estimated $720 million in 2009 from $190 million in 2000, the study said.
Hospitals in states such as Kentucky and West Virginia have reported a sharp rise in the number of opioid-dependent babies. In Florida, long the nation’s epicenter of illegal prescription-drug sales, the problem is acute, especially in a cluster of counties near Tampa Bay, including Sarasota.
Hospitals such as Spring Hill Regional Hospital, north of Tampa, said that as many as 30% of the babies in their NICUs suffer from opioid withdrawal.
Hospitals were ill-prepared for the drug-dependent infants. “This isn’t a problem I learned about in training,” said Terri Ashmeade, medical director of the NICU and chief of pediatrics at Tampa General Hospital.
Her unit, like others, relied at first on protocols for heroin withdrawal in babies, mainly using phenobarbital, she said. But the staff quickly found that withdrawal symptoms for today’s painkillers, which are powerful and long-acting, were much more severe.
The newborns cry incessantly, jerk their limbs and vomit. They can have such severe diarrhea that it burns the skin off their bottoms. Though treating them with the very opioids they are withdrawing from may seem jarring, doctors say the alternative could be worse: seizures and even death.
After years of trying different treatments, Tampa General settled on a uniform approach three months ago. Like many hospitals, it relies on a system that assigns points for different symptoms, and it initiates drug treatment if the numbers cross a certain threshold. (There is no blood test or other diagnostic to determine whether a baby is drug-dependent.)
Eight hours after he was born, Gabriel, a baby undergoing treatment recently at Tampa General’s NICU, exhibited a variety of symptoms, including stiffened muscles and excessive sucking.
So the hospital gave him methadone and, when the symptoms persisted, increased the doses until he reached the maximum. Two days later, he was still scoring high, so the hospital gave him clonidine, a drug used to treat withdrawal in adults.
At eight days, Gabriel was still taking the maximum dosage of methadone and close to the maximum of clonidine. He appeared mostly calm, but startled and trembled at times. It would likely take weeks more to wean him off the drugs, nurses said.
Sixty miles to the south, Sarasota Memorial is following a different protocol. While using the same scoring system, it starts babies on morphine, and if necessary, adds phenobarbital.
Hospitals have no choice but to experiment, given the paucity of research on what treatments are most effective. The American Academy of Pediatrics in February published new guidelines for neonatal abstinence syndrome–its first update since 1998. Though the paper cited a range of potential treatments, it didn’t recommend one particular protocol.
To try to come up with a standard regimen, a collaborative of Florida hospitals, including Sarasota Memorial, plans to compare various approaches.
Each NICU will rely on morphine and clonidine, but at different dosages, increased and decreased at different rates, said Mark Hudak , a neonatologist at Wolfson Children’s Hospital in Jacksonville, which is part of the group. The group hopes to assemble its findings some time next year.
One objective is to cut down the amount of time babies are spending in intensive care and assess whether they are being over – medicated, Mr. Hudak said.
Hospitals are grappling with another concern: They worry they aren’t catching all the affected babies. Not every mother is forthcoming about using prescription painkillers, which leaves it up to medical staff to look out for symptoms.
Most newborns are discharged within 48 to 72 hours, yet babies exposed to long-acting opioids like methadone can take five or more days to show signs of withdrawal.
“Some are going home and withdrawing,” said Tony Napolitano , medical director at Sarasota Memorial. And a mother with dependency issues may not be equipped to handle a highly irritable and sensitive newborn, he said.
Organizations like the Healthy Start Coalition of Hillsborough County, a nonprofit, are urging obstetricians to broach the subject of opioid use with their patients. Many don’t, often because they are unaware how widespread the problem is, said Executive Director Jane Murphy.
Because the phenomenon of opioid-exposed babies is so new, little is known about any long-term effects. Some studies suggest they are at greater risk of attention deficit hyperactivity disorder, but the findings aren’t conclusive.
Fears that the “crack babies” of decades past would develop severe physical, mental and emotional disabilities proved to be unfounded, research showed. But prescription-drug exposure ” seems to be affecting babies’ physiologies more than cocaine,” said Ms. Ashmeade, the Tampa General neonatologist.
What Do You Get When Legal Drug Dealers Peddle “Heroin-in-a-Pill” to it’s “Clientele”?
Jaclyn Kinkade , a 23-year-old doctor’s-office receptionist and occasional model, was a casualty of America’s No. 1 drug menace when she overdosed and died, alone, in a tumbledown clapboard house in Dunnellon, Fla.
The drugs that killed her didn’t come from the Colombian jungles or an Afghan poppy field.
Two of the three drugs found in her system were sold to Ms. Kinkade, legally, at Walgreen Co. and CVS Caremark shops, the two biggest U.S. pharmacies.
Both prescription drugs found in her body were made in the U.S.–the oxycodone in Elizabeth, N.J., by a company being acquired by generic-drug giant Watson Pharmaceuticals Inc., and the methadone in Hobart, N.Y., by Covidien Ltd., another major manufacturer. Every stage of their distribution was government-regulated. In addition, Ms. Kinkade had small amounts of methamphetamine in her system when she died.
The U.S. spends about $15 billion a year fighting illegal drugs, often on foreign soil. But America’s deadliest drug epidemic begins and ends at home . More than 15,000 Americans now die annually after overdosing on prescription painkillers called opioids, according to the Centers for Disease Control and Prevention–more than from heroin, cocaine and all other illegal drugs combined.
Rising opioid abuse means that drug overdoses are now the single largest cause of accidental death in America. They surpassed traffic accidents in 2009, the most recent CDC data available.
Paradoxically, the legality of prescription painkillers makes their abuse harder to tackle. There is no Pablo Escobar to capture or kill. Authorities must contend with an influential lobby of industry representatives and doctors who argue against more restrictions, saying they would harm legitimate patients. And lawmakers have been reluctant to have the federal government track Americans’ prescriptions, leaving states to piece together a patchy, fragmented response.
Ms. Kinkade’s final days, and the path of the drugs that killed her, were reconstructed from medical and prescription records, police files and interviews. Many records were assembled by Ms. Kinkade’s father and stepmother.
Shuffling through the documents at their living-room table, Bruce Kinkade, a garage-door salesman, and his wife, Ann, said they don’t wish to absolve their daughter of responsibility. “We’re not naive and want to say she was a perfect angel,” said Ann Kinkade, Jaclyn’s stepmother.
Tracing the Path of Prescription Painkillers
Jaclyn Kinkade: A Family Photo of Jaclyn Kinkade As a Child With a Composite of The Prescription Records.
But the Kinkades say the companies and licensed professionals that supplied her with the drugs must also bear some responsibility. “Jackie didn’t wake up one day and say, ‘Hey, I’m going to be a drug addict today,'” Ann Kinkade said. “Jackie pretty much got sent there by a doctor, got hooked and continued to go back.”
There are few easy villains in prescription drug abuse. Companies, physicians and addicts alike are all pieces in a complex puzzle. For some time, regulators have been cracking down on doctors who prescribe to addicts for profit. Now, federal and state officials are starting to move up the supply chain to pursue pharmacies and distributors.
On Sept. 12, the Drug Enforcement Administration revoked the licenses of two Florida CVS stores, which it claims sold excessive amounts of oxycodone without ensuring the pills weren’t diverted to the black market. CVS is fighting the DEA’s order in administrative and federal courts.
Two days later, the agency served Walgreen with a suspension order halting sales of controlled substances from its Jupiter, Fla., distribution center, calling it an “imminent threat to public safety.”
The DEA’s regulatory action alleges that the facility–the state’s largest oxycodone distributor–” failed to maintain effective controls ” of its narcotic painkillers.
Walgreen said it is working with regulators and has tightened its procedures. CVS said it was committed to working with regulators “to reduce prescription drug abuse and diversion while ensuring access to appropriate, effective pain medication for our patients who need them.”
Participants in the drug-supply chain acknowledge the problems but point to others as the weak link.
Doctors involved say pharmacies should be able to tell if patients are secretly using several physicians to obtain more drugs. Druggists say they can’t second-guess a valid prescription. Manufacturers and distributors say they are simply delivering products ordered by health-care professionals.
What makes this drug scourge different from previous ones, such as heroin in the 1970s and cocaine in the 1980s, is that everyone in the distribution chain is identifiable . The DEA itself controls the supply spigot by setting drug companies’ production quotas for opioids like oxycodone and hydrocodone.

For years, opioids were reserved mainly for cancer or terminally ill patients because of fears over their safety and addictiveness. But over the past 15 years, many doctors have come to view them as an essential tool to manage chronic pain. Around the same time, drug makers began marketing patented, time-release formulations of the drugs, making it a lucrative category.
Today, a growing number of doctors say the pendulum has swung too far, with powerful narcotics being dispensed for even relatively minor complaints. Last year, pharmacies dispensed more than $9 billion in prescription opioid painkillers, more than twice the amount a decade earlier, according to IMS Health, a research firm.
The number of prescriptions has risen fourfold. The generic version of Vicodin, a blend of hydrocodone and acetaminophen, is now the most prescribed drug in the country.
Opioids come from the same narcotics family as heroin and can produce similar addictions, researchers say. “We’re basically talking about heroin pills,” said Andrew Kolodny, chairman of the psychiatry department at Maimonides Medical Center in New York.
Studies show that opioid addicts come from a surprisingly broad swath of the population: the middle-age, the elderly and, increasingly, young adults.
Many U.S. veterans returning from Iraq and Afghanistan with physical and mental injuries are also becoming dependent on prescription painkillers, researchers say.
In recent decades, researchers have come to view addiction as a disease, rather than just a personal failing. Some people are more predisposed to becoming addicted because of heredity, experience and other factors that have yet to be fully understood. But some drugs are simply more addictive than others.

Jaclyn Kinkade Before She Began Taking Drugs.
New research suggests that drugs like opioids cause long-lasting changes to the brain, rewiring some areas to crave more drugs while simultaneously damaging the parts that can control those cravings.
The drugs can damage the brain’s ability to feel pleasure, so regular users eventually need to take them not to get high or help with pain, but just to feel normal. Avoiding unpleasant withdrawal symptoms end up conditioning many drug users’ daily lives.
One of the most confounding aspects of this latest epidemic is that it blurs the lines between legal and illegal drug use. Some people first take drugs from their family medicine cabinets to get high, then go to doctors to get more. Others are originally prescribed the pills for legitimate reasons, then buy them on the street once they’re hooked.
Many, such as Ms. Kinkade, end up mixing legal and illegal drugs in ways that can prove lethal.
Ms. Kinkade was a lively, talkative woman with blond hair, a fear of caterpillars and a pit-bull terrier, Bentley, that traveled everywhere with her.
She was first prescribed an opioid on Oct. 27, 2006, by the doctor who employed her as a receptionist, prescription records show. According to medical records and an entry from her diary, she had been suffering back and neck pain.
Thomas Suits, her employer, prescribed 20 pills of Endocet, a drug containing oxycodone. “I’d never taken opioids before,” Ms. Kinkade wrote in a diary entry. “But I started the med routine and OMG I felt no pain.”

Jaclyn Kinkade On Vacation When She Was 21 Years Old. She Died Of An Accidental Drug Overdose About Two Years Later, At Age 23.
Dr. Suits didn’t recall prescribing the medication, said his wife, Irene Machel, a doctor who also works at the clinic. She declined to discuss the matter further.
Endo Health Solutions, which made the pills, declined to comment on Ms. Kinkade . “These types of stories are tragic and we obviously take them seriously,” said Endo spokesman Blaine Davis. “Our responsibility, as a company that is very dedicated to the field of pain management, is to educate both physicians and patients about appropriate use.”
Soon Ms. Kinkade was seeking more drugs. On Jan. 5, 2007, she saw Bruce Kammerman, a family practitioner at a clinic in Stuart, Fla., and came away with a generic blend of oxycodone and acetaminophen. A scan taken a month later showed no problems with her spine, according to the medical report.
Through his lawyer, Dr. Kammerman declined to say why he wrote the prescription. “That’s a sad case,” said his attorney, Lance Richard. “Maybe she didn’t have justifiable pain but she certainly came in and made complaints about it. At some point the doctor just has to go on the patient’s word.”
Dr. Kammerman was arrested in July at a pain clinic in Vero Beach, Fla., charged with drug trafficking, racketeering and illegally selling controlled substances. The DEA said in a news conference he was prescribing an average of 1,700 oxycodone tablets a day. Dr. Kammerman’s lawyer said his client has done nothing wrong and pleaded not guilty.

Jaclyn Kinkade In a Mug Shot on May 10, 2010, Two Months Before Her Death.
Ms. Kinkade broke up with her boyfriend. She began missing work. One day she was found curled up under her desk, crying. “She always used to be clean-cut, nice makeup,” said Susan Cochran, a former colleague. Then “she would come in in sweatpants and it was like: ‘Who is this person?'”
Ms. Kinkade changed jobs to work at a radiologist’s office. There, she had two other scans, in April and July 2008. Neither showed significant spine problems, according to the medical reports. Ms. Kinkade started seeking clinics that asked fewer questions. ” Family practitioners hate writing narcotics ,” she wrote in her diary. “Nowadays–I’ll just go str8 to pain docs.”
During that period, she was prescribed large amounts of oxycodone, her records show, combined with anti-anxiety drugs and powerful muscle relaxants. Her parents grew increasingly alarmed. “Sometimes you’d be having a conversation with her and her head would just drop,” Mr. Kinkade said. “And she’d say: ‘Oh, I’m just tired; I was out late.'”
After reviewing her records, he said, “We estimated that at one point she was taking 13.4 pills per day, for nothing wrong with her.”
In May 2009, Mr. Kinkade and his wife asked a judge to have their daughter forcibly admitted to drug treatment under a Florida law. Their request was initially denied because she wasn’t a minor.
Angered by their efforts, Ms. Kinkade moved out of their home and drove across the state to her biological mother’s house. She crashed her car and was found wandering along the highway in a drug-induced daze, her parents said, searching for her pills.
Legal records show she was arrested several times for minor crimes such as possessing controlled drugs without a prescription and shoplifting small items, including makeup and cake topping. In each case, she was released and the charges dropped.

She started visiting a pain clinic in Tampa called Doctors Rx Us , where she was prescribed oxycodone, methadone, alprazolam and gabapentin, an antiseizure medication, according to records her parents collected. Housed in a rundown strip mall, the clinic today is called Palm Medical Group after a name change in 2011, according to its state records.
Ms. Kinkade was prescribed the drugs by two physicians at Doctors Rx Us: Richard Smith and William Crumbley. Dr. Crumbley was arrested in December and charged with operating a nonregistered pain clinic at another location. He has pleaded not guilty.
Dr. Smith and the clinic declined repeated interview requests. A lawyer for Dr. Crumbley said he was innocent of any wrongdoing.
On May 3, 2010, Ms. Kinkade stopped at a CVS in Crystal River, Fla., and picked up a prescription written by Dr. Smith for 90 tablets of 10mg methadone, along with 90 tablets of alprazolam, an antianxiety drug.
“Jaclyn Kinkade’s death is a terrible tragedy that highlights the need for a comprehensive national effort to prevent prescription drug abuse,” CVS said in a statement.
Information provided by the manufacturer suggests that the methadone dispensed to Ms. Kinkade was likely supplied to CVS by Cardinal Health Inc. Cardinal was the only distributor to have sold that particular drug to that CVS branch during that period, according to the manufacturer’s records. CVS and Cardinal declined to comment.
Last year, the DEA launched a probe of the Florida-based operations of Cardinal Health and CVS Caremark. The agency alleged they dispensed “extremely large amounts” of oxycodone with signs that the drugs were “diverted from legitimate channels.”
CVS said it has “responded to the DEA’s concerns, including implementing enhancements to our policies and procedures for filling controlled substance prescriptions.” Cardinal settled with the DEA in May, agreeing to suspend sales for two years at one of its key distribution facilities in Lakeland, Fla.
The methadone Ms. Kinkade picked up at the end of her life was made in Hobart, N.Y., by Mallinckrodt , a unit of health-care giant Covidien .
“Any death from abuse or misuse of prescription drugs is tragic,” Covidien said. “That’s why we believe that, as a nation, ending the abuse, diversion and misuse of powerful pain medications is necessary to ensure adequate treatment of pain and access to that treatment for legitimate pain patients.”
On May 10, 2010, Ms. Kinkade was stopped by police in Levy County, Fla., for having an expired registration. A drug-sniffing dog reacted to her car and she was arrested for possessing a generic form of Xanax without the correct prescription.
This time, her parents let her sit in jail for a couple of weeks while they organized a place for her in a rehabilitation program. They bailed her out May 25 and enrolled her in drug treatment.
Over the next month, Ms. Kinkade went to the treatment program during the day and seemed to improve, her parents said. Then, the evening of June 24, she climbed out the window at her parents’ house.
A few days later, on the other side of Florida, she met up with a boyfriend, according to a statement he later gave police. She returned to Doctors Rx Us, where Dr. Smith wrote a prescription for 90 tablets of 30mg oxycodone, according to prescription records. It would be her last.
The next day, Ms. Kinkade filled the prescription at a Walgreens in Beverly Hills, Fla. The oxycodone would have come from Walgreen’s Jupiter, Fla. , distribution center, a company spokesman said.
On Sept. 14, the DEA barred that facility from selling controlled substances, alleging that it failed to maintain effective controls to stop large amounts of oxycodone from reaching the black market.
“When [companies] choose to look the other way, patients suffer and drug dealers prosper,” Mark Trouville, the DEA special agent in charge, said at the time. Walgreen said in a statement it is cooperating with the DEA.
The oxycodone came from the New Jersey plant of Actavis, a Swiss pharmaceutical company. In April, Actavis was bought by Watson Pharmaceutical in a $5.8 billion deal awaiting regulatory approval.
An Actavis spokesman described Ms. Kinkade’s situation as a “tragic occurrence” and called for discussion on “how to prevent such cases in the future.”
A Watson spokesman cautioned against action that would make it harder to treat legitimate patients . He said the company supported educating patients about the drugs’ proper use.
The morning of July 4, Ms. Kinkade’s boyfriend found her sitting cross-legged and slumped in his room at a white, low-slung house tucked behind a trailer park. The medical examiner said she died from a drug cocktail including oxycodone, methadone and methamphetamine.
Ms. Kinkade’s physical decline made such an impression on the detective who investigated the case that, two years later, he still recalls the scene. In the living room, he noticed a poster of Ms. Kinkade modeling for a biker magazine.
“Wow, she’s a beautiful young lady,” Detective Matthew Taylor remembered thinking. “When I actually saw her, it was as different as night and day.”
Updated: 12-29-2025
A Surprising Treatment For Chronic Lower Back Pain: Cannabis
Two new drug trials find a THC-based cannabis extract could help with a condition that affects millions.
It’s the leading cause of disability and one of the most costly health challenges of our time: chronic lower back pain.
Yet effective and safe treatments are few and far between, leading patients to try everything from supplements to acupuncture to cannabis for relief.
Now, two new studies provide some of the most comprehensive evidence yet that THC—the psychoactive compound in cannabis that creates the high—in combination with other parts of the cannabis plant may provide safe and effective relief.
The two large, Phase 3 clinical trials demonstrated that the THC product is safe and more effective at reducing chronic lower back pain than placebo or opioids.
Unfortunately, the news, while promising, won’t provide immediate relief for the more than 70 million U.S. adults who suffer from chronic lower back pain.
The product tested is expected to be available in parts of Europe next year, while the path to approval in the U.S. will require another clinical trial.
Doctors say the studies may make healthcare providers more likely to prescribe federally approved medical cannabis for chronic lower back pain off-label. And consumers can try experimenting with products with similar combinations of cannabis compounds so long as they start with low doses of THC.
Meanwhile, the White House directed federal agencies to reclassify cannabis as a less-dangerous drug, a move that will likely further increase its popularity in states where cannabis is sold legally.
The studies were conducted by Vertanical, a German pharmaceutical company. It used a proprietary cannabis extract from a sativa strain, containing majority THC, as well as smaller amounts of other cannabinoids, such as CBD and CBG, and other compounds from the cannabis plant.
Ziva Cooper, director of the UCLA Center for Cannabis and Cannabinoids, said even though the commercial version of the product from the studies won’t be available in the U.S. anytime soon, physicians can use the results to help guide patients.
“I think these might be landmark studies that physicians can look to and might make them more comfortable prescribing dronabinol with chronic lower back pain,” says Cooper, who wasn’t involved with the study.
Dronabinol is a synthetic form of THC that is approved by the U.S. Food and Drug Administration to treat patients with AIDS-related anorexia and chemotherapy-induced nausea.
Some doctors are already doing that.
Dr. Kevin Hill, an associate psychiatry professor at Harvard Medical School and director of addiction psychiatry at Beth Israel Deaconess Medical Center, says he prescribes cannabis to treat pain in his practice but not as a first-line treatment.
The first of the cannabis studies, published in journal Nature Medicine earlier this year, included more than 800 chronic lower back pain patients. It found after 12 weeks of treatment that the patients taking the cannabis extract reported less pain than those taking a placebo.
The effects continued for up to a year and were particularly pronounced in those with neuropathic and severe pain. Participants also reported improvements in sleep quality and physical function. When stopping the cannabis product, participants had no withdrawal symptoms.
A second study enrolled more than 380 patients and found cannabis was more effective at alleviating pain than opioids and resulted in less constipation.
Vertanical is applying to have a licensed drug product in Germany and several other European countries next year. It says it’s also in talks with the FDA to conduct another Phase 3 trial in the U.S.
Kevin Boehnke, an assistant professor of anesthesiology at the University of Michigan Medical School, says the two studies “are a big deal.”
THC is the cannabinoid most associated with dependence and getting high. But the research found that once people went through a three-week titration period, side effects—such as feeling a high—stabilize at a much lower frequency.
Despite the fact that the product used in the studies won’t be available in the U.S. anytime soon, Boehnke says the research is still informative for consumers. If deciding to try cannabis for lower back pain relief, start low and go slow, he says.
“Don’t overshoot, do it over a number of weeks,” he says.
In the studies, participants started taking 2.5 milligrams of THC twice a day. Patients increased doses every 3 days, capping out at about 10 milligrams twice a day.
Once patients reached an effective dose, it wasn’t increased. This is notable given the studies were three to six months, says Cooper.
In the study comparing opioids to cannabis, patients had to increase their dose of opioids while those taking the cannabis medication didn’t.
“We know that tolerance does develop to certain effects of THC,” says Cooper. “Here, patients didn’t need to increase their dose to relieve their pain, reducing the chances of unwanted side effects.”
Boehnke says cannabis can potentially be a good alternative to opioids. Still, people should be cautious of the potential for addiction, he says.
Studies show that chronic pain is the most common reason people take medical marijuana.
Nearly 26% of people with chronic pain reported managing it with cannabis over the past year and a quarter said they had taken it in the last 30 days, according to a 2023 Jama Network Open study.
More than half said their use of cannabis allowed them to decrease their use of opioids or over-the-counter pain medications.
That jibes with the findings of a recent JAMA Internal Medicine study that followed more than 200 patients with chronic pain over 18 months.
Researchers were looking to see if those patients taking cannabis reduced their use of opioids.
“We found that…controlling for confounding factors including time and mental health symptoms and pain, medical cannabis reduced opioid use consistently,” says Dr. Deepika Slawek, an associate professor of medicine at Montefiore Einstein in New York City and first author of that study.
But before you think THC is going to solve all your chronic back pain, keep in mind that the average differences in pain between the group that took the cannabis extract versus placebo was statistically significant but relatively small, notes Dr. Devan Kansagara, a professor of medicine at Oregon Health and Science University in Portland.
“Pain in general is a tough thing to move the needle on,” says Kansagara.
You Can Buy CBD And CBG Extracts For Lower Back Pain From Various Online Retailers That Specialize In Cannabinoid Products
Look for reputable brands that offer full-spectrum or broad-spectrum options, as these may provide enhanced relief for pain management.
Where To Buy CBD And CBG Extracts For Lower Back Pain
Online Retailers
Retailer Product Type Key Features
Aspen Green Muscle Relief Cooling Cream Full Spectrum CBD, Organic, Fast Absorption
Rare Cannabinoid Company CBG + CBD + THC Rapid Relief Gel Dispensary-Strength, Non-Sticky, Cooling Effect
Canna River Pain CBD Oil Tincture Broad Spectrum, Various Flavors, High Potency
Neurogan CBG Oil Tincture High Potency, Neuroprotective Effects
Extract Labs CBD Oil And Topicals Organic, Third-Party Tested, Various Formulations
Local Dispensaries
Check Local Dispensaries: Many states have dispensaries that sell CBD and CBG products. Look for those that offer products specifically for pain relief.
Health Stores: Some health food stores may carry CBD and CBG products. It’s best to call ahead to check availability.
Considerations
Product Type: Look for creams, oils, or tinctures that specifically mention pain relief.
THC Content: Ensure you understand the THC levels in the products, as some may contain psychoactive components.
Lab Testing: Choose products that have been third-party tested for quality and potency.
These options should help you find suitable CBD and CBG extracts for managing lower back pain.
Related Articles:
Bitcoin Information & Resources (#GotBitcoin)
Houston Software Executive Charged With Largest Tax Evasion Case In History Against An Individual
The Best Solo Miners. Feat. The NerdQaxe++
Bitcoin Bulls Take Over The Military
The Three High-Tech Steps That Can Lower Your Energy Bills
Sauerkraut, Kimchi And…Gut Nuts? Fermented Foods Are Having A Moment
America’s Car Repossessions Business Is Booming If You Have What It Takes!!
These AI Power Users Are Impressing Bosses And Leaving Co-Workers In The Dust
11 Most Famous Black Female Artists
Monty: Is Job-Hoarding Officially Over? AI: Yes
Why Every Family Needs A Code Word
Do You Have What It Takes To Be A $100k A Year Executive Housekeeper?
Ultimate And Complete Guide On Herbs For Culinary And Medicinal Uses
North Korea Is Open. Who’s Going? Apparently Everyone!
Bill Wilson, LSD And The Secret Psychedelic History Of Alcoholics Anonymous
Why America Will Lose The Mercantilist Game
The “Debasement Trade” Is Forcing Investors To Buy Bitcoin And Gold!!
ICE Tracking Apps Are Booming And Digital Resistance Teams Are Ready To Help
From Coders To CEOs: Who’s Earning In/And Accepting (Coffee Shops To Airlines) Bitcoin In 2025
Google Reveals AI Agent Payments Protocol Backed By Bitcoin And TradFi Industry Payment Providers
Vietnam Banks Close 86 Million And Thailand Banks Close 3 Million Customer Accounts
Americans Are Having Less Sex Than Ever
Mushroom Magic In The Kitchen (Recipes)
The Price Of Parenting. TL;DR, It Takes A Helluva Lot of Money
Ultimate Resource On Mushrooms From Foraging, Medicinal, Cultivation And More
Humans Can Echolocate Like Bats And Dolphins. We Explain How It Works
Our Arctic Vacation Itineraries (2026)
Goodbye Gentle Parenting, Hello ‘F—Around And Find Out’
The Many Health Benefits of Nitric Oxide
How To Eliminate Mouth Breathing In Children And Teenagers
We RFK’d The Fries And Food Dyes
Declining Dollar Hits Amazon Forcing It To Raise Prices
Red Yeast Rice VS Prescription Statin Drugs
European Commission Plans A “Reverse Robinhood” Via Savings And Investments Union (SIU)
Un Día Sin Mexicanos (“A Day Without A Mexican”) Is Today!
Is Perplexity AI A Bloomberg Terminal Killer? Not Even Close!
Compounding Pharmacies Explained: Safety, Regulations And More
Sell Stock In Yourself Or Some Of Your Home Equity For Bitcoin
North Korea Infiltrates U.S. Remote Jobs—With The Help of Everyday Americans
America’s Leading Alien Hunters Depend On AI To Speed Their Search
Bitcoin’s Nouveau Riche Executives And Wealthy Investors In Search Of Ways To Protect Themselves
How Anthocyanins Shield Us From Microplastics
Origins Of Toxic Algae (Domoic Acid) Killing Sea Lions, Birds And Dolphins In Southern California
The Human Brain And It’s Ability To Time-Travel
Wall Street’s New Tariff Safe Haven: Biotech Companies Adopting Bitcoin Treasury Strategy
How Natural “Short Sleepers” Thrive On 4 Hours Of Sleep Per Night Thanks To A Gene Mutation
Nine Unknown Benefits of Sleep Including Penal And Clitoral Erections
Elite Athletes Try A New Training Tactic: More Vitamin D3
Bitcoin Industry On A Winning Streak As Sec. Drops Lawsuit After Lawsuit!!
FOIA Files: Elon Musk’s DOGE Wants A Heads Up On FOIA Requests
When Russia Came To Defend The United States
Ultimate Resource Covering DOGE AKA The Department of Government Efficiency
Your Money Is Currently Lawful. However, That Is Subject To Change #GotBitcoin #BitcoinFixesThis
Is The United Nations Going Bankrupt?
Bitcoin Industry Founders Should Stop Chasing Narratives And Start Creating Them
Consumer Finance Watchdog Finalizes ‘Open Banking’ Rules Aimed At Driving Competition
US Government Crypto Wallets Hacked For $20M — Arkham Intelligence
Coinbase Files FOIAs Against US Regulators Probing Banks’ Bitcoin Crackdown
The Botanist Daring To Ask: What If Plants Have Intelligence?
Theoretical Physicist Sylvester James Gates
FOIA Request Reveals SEC’s Gensler, Lawmakers Target Of Violent Threats
Ultimate Resource For Prediction Markets Covering Politics, Pop Culture, Sports And More
September (AKA Rektember) Is Once Again A Tough Month For Stocks AND Bitcoin
Ultimate Resource For Cloning humans. Biological, Ethical, And Social Considerations
FOIA Reveals Aurora Borealis Imperiled US Infrastructure From Power Grids To Satellites (5-10-2024)
Ultimate Resource Covering How “Silent Payments” Are Bringing New Privacy Protections To Bitcoin
Nostr Allows Bitcoiners To Build-Out A Decentralized, CENSORSHIP-RESISTANT Social-Media!!
Joe Rogan: I Have A Lot Of Hope For Bitcoin
Teen Cyber Prodigy Stumbled Onto Flaw Letting Him Hijack Teslas
Spyware Finally Got Scary Enough To Freak Lawmakers Out—After It Spied On Them
The First Nuclear-Powered Bitcoin Mine Is Here. Maybe It Can Clean Up Energy FUD
The World’s Best Bitcoin Policies: How They Do It In 37 Nations
Tonga To Copy El Salvador’s Bill Making Bitcoin Legal Tender, Says Former MP
Wordle Is The New “Lingo” Turning Fans Into Argumentative Strategy Nerds
Prospering In The Pandemic, Some Feel Financial Guilt And Gratitude
Is Art Therapy The Path To Mental Well-Being?
New York, California, New Jersey, And Alabama Move To Ban ‘Forever Chemicals’ In Firefighting Foam
The Mystery Of The Wasting House-Cats
What Pet Owners Should Know About Chronic Kidney Disease In Dogs And Cats
Pets Score Company Perks As The ‘New Dependents’
Why Is My Cat Rubbing His Face In Ants?
Natural Cure For Hyperthyroidism In Cats Including How To Switch Him/Her To A Raw Food Diet
Ultimate Resource For Cat Lovers
FDA Approves First-Ever Arthritis Pain Management Drug For Cats
Ultimate Resource On Duke of York’s Prince Andrew And His Sex Scandal
Walmart Filings Reveal Plans To Create Cryptocurrency, NFTs
Bitcoin’s Dominance of Crypto Payments Is Starting To Erode
T-Mobile Says Hackers Stole Data On About 37 Million Customers
Jack Dorsey Announces Bitcoin Legal Defense Fund
More Than 100 Millionaires Signed An Open Letter Asking To Be Taxed More Heavily
Federal Regulator Says Credit Unions Can Partner With Bitcoin Providers
What’s Behind The Fascination With Smash-And-Grab Shoplifting?
Train Robberies Are A Problem In Los Angeles, And No One Agrees On How To Stop Them
US Stocks Historically Deliver Strong Gains In Fed Hike Cycles (GotBitcoin)
Ian Alexander Jr., Only Child of Regina King, Dies At Age 26
Amazon Ends Its Charity Donation Program Amazonsmile After Other Cost-Cutting Efforts
BTC Panics, Then Jeers at DOJ Announcement of ‘Major Action’ Against Tiny Chinese Exchange Bitzlato
Indexing Is Coming To BTC Funds Via Decentralized Exchanges
Doctors Show Implicit Bias Towards Black Patients
Darkmail Pushes Privacy Into The Hands Of NSA-Weary Customers
3D Printing Make Anything From Candy Bars To Hand Guns
Stealing The Blood Of The Young May Make You More Youthful
Henrietta Lacks And Her Remarkable Cells Will Finally See Some Payback
AL_A Wins Approval For World’s First Magnetized Fusion Power Plant
Want To Be Rich? Bitcoin’s Limited Supply Cap Means You Only Need 0.01 BTC
Smart Money Is Buying Bitcoin Dip. Stocks, Not So Much
McDonald’s Jumps On Bitcoin Memewagon, Crypto Twitter Responds
America COMPETES Act Would Be Disastrous For Bitcoin Inustry (LOL) And More
Lyn Alden On Bitcoin, Inflation And The Potential Coming Energy Shock
Inflation And A Tale of Cantillionaires
El Salvador Plans Bill To Adopt Bitcoin As Legal Tender
Miami Mayor Says City Employees Should Be Able To Take Their Salaries In Bitcoin
Vast Troves of Classified Info Undermine National Security, Spy Chief Says
BREAKING: Arizona State Senator Introduces Bill To Make Bitcoin Legal Tender
San Francisco’s Historic Surveillance Law May Get Watered Down
How Bitcoin Contributions Funded A $1.4M Solar Installation In Zimbabwe
California Lawmaker Says National Privacy Law Is a Priority
The Pandemic Turbocharged Online Privacy Concerns
How To Protect Your Online Privacy While Working From Home
Researchers Use GPU Fingerprinting To Track Users Online
Japan’s $1 Trillion Bitcoin Industry May Ease Onerous Listing Rules
Ultimate Resource On A Weak / Strong Dollar’s Impact On Bitcoin
Fed Money Printer Goes Into Reverse (Quantitative Tightening): What Does It Mean For Crypto?
BTC Market Is Closer To A Bottom Than Stocks (#GotBitcoin)
When World’s Central Banks Get It Wrong, Guess Who Pays The Price??? (#GotBitcoin)
“Better Days Ahead With Crypto Deleveraging Coming To An End” — Joker
Bitcoin Funds Have Seen Record Investment Inflow In Recent Weeks
Bitcoin’s Epic Run Is Winning More Attention On Wall Street
Ultimate Resource For Bitcoin Industry Mergers And Acquisitions (M&A) (#GotBitcoin)
Why Wall Street Is Literally Salivating Over Bitcoin
Nasdaq-Listed MicroStrategy And Others Wary Of Looming Dollar Inflation, Turns To Bitcoin And Gold
Bitcoin For Corporations | Michael Saylor | Bitcoin Corporate Strategy
Ultimate Resource On Myanmar’s Involvement With Bitcoin Industry
‘I Cry Every Day’: Olympic Athletes Slam Food, COVID Tests And Conditions In Beijing
Does Your Baby’s Food Contain Toxic Metals? Here’s What Our Investigation Found
Ultimate Resource For Pro-Bitcoin Lobbying And Non-Profit Organizations
Ultimate Resource On BlockFi, Celsius And Nexo
Petition Calling For Resignation Of U.S. Securities/Exchange Commission Chair Gary Gensler
100 Million Americans Can Legally Bet on the Super Bowl. A Spot Bitcoin ETF? Forget About it!
Green Finance Isn’t Going Where It’s Needed
Shedding Some Light On The Murky World Of ESG Metrics
SEC Targets Greenwashers To Bring Law And Order To ESG
BlackRock (Assets Under Management $7.4 Trillion) CEO: Bitcoin Has Caught Our Attention
Canada’s Major Banks Go Offline In Mysterious (Bank Run?) Hours-Long Outage (#GotBitcoin)
On-Chain Data: A Framework To Evaluate Bitcoin
On Its 14th Birthday, Bitcoin’s 1,690,706,971% Gain Looks Kind of… Well Insane
The Most Important Health Metric Is Now At Your Fingertips
American Bargain Hunters Flock To A New Online Platform Forged In China
Why We Should Welcome Another Crypto Winter
Traders Prefer Gold, Fiat Safe Havens Over Bitcoin As Russia Goes To War
Music Distributor DistroKid Raises Money At $1.3 Billion Valuation
Nas Selling Rights To Two Songs Via Crypto Music Startup Royal
Ultimate Resource On Music Catalog Deals
Ultimate Resource On Music And NFTs And The Implications For The Entertainment Industry
Lead And Cadmium Could Be In Your Dark Chocolate
Catawba, Native-American Tribe Approves First Digital Economic Zone In The United States
The Miracle Of Blockchain’s Triple Entry Accounting
How And Why To Stimulate Your Vagus Nerve!
Housing Boom Brings A Shortage Of Land To Build New Homes
Biden Lays Out His Blueprint For Fair Housing
No Grave Dancing For Sam Zell Now. He’s Paying Up For Hot Properties
Cracks In The Housing Market Are Starting To Show
Ever-Growing Needs Strain U.S. Food Bank Operations
Food Pantry Helps Columbia Students Struggling To Pay Bills
Food Insecurity Driven By Climate Change Has Central Americans Fleeing To The U.S.
Housing Insecurity Is Now A Concern In Addition To Food Insecurity
Families Face Massive Food Insecurity Levels
US Troops Going Hungry (Food Insecurity) Is A National Disgrace
Everything You Should Know About Community Fridges, From Volunteering To Starting Your Own
Russia’s Independent Journalists Including Those Who Revealed The Pandora Papers Need Your Help
10 Women Who Used Crypto To Make A Difference In 2021
Happy International Women’s Day! Leaders Share Their Experiences In Crypto
Dollar On Course For Worst Performance In Over A Decade (#GotBitcoin)
Juice The Stock Market And Destroy The Dollar!! (#GotBitcoin)
Unusual Side Hustles You May Not Have Thought Of
Ultimate Resource On Global Inflation And Rising Interest Rates (#GotBitcoin)
The Fed Is Setting The Stage For Hyper-Inflation Of The Dollar (#GotBitcoin)
An Antidote To Inflation? ‘Buy Nothing’ Groups Gain Popularity
Why Is Bitcoin Dropping If It’s An ‘Inflation Hedge’?
Lyn Alden Talks Bitcoin, Inflation And The Potential Coming Energy Shock
Ultimate Resource On How Black Families Can Fight Against Rising Inflation (#GotBitcoin)
What The Fed’s Rate Hike Means For Inflation, Housing, Crypto And Stocks
Egyptians Buy Bitcoin Despite Prohibitive New Banking Laws
Archaeologists Uncover Five Tombs In Egypt’s Saqqara Necropolis
History of Alchemy From Ancient Egypt To Modern Times
Former World Bank Chief Didn’t Act On Warnings Of Sexual Harassment
Does Your Hospital or Doctor Have A Financial Relationship With Big Pharma?
Ultimate Resource Covering The Crisis Taking Place In The Nickel Market
Apple Along With Meta And Secret Service Agents Fooled By Law Enforcement Impersonators
Handy Tech That Can Support Your Fitness Goals
How To Naturally Increase Your White Blood Cell Count
Ultimate Source For Russians Oligarchs And The Impact Of Sanctions On Them
Ultimate Source For Bitcoin Price Manipulation By Wall Street
Russia, Sri Lanka And Lebanon’s Defaults Could Be The First Of Many (#GotBitcoin)
Will Community Group Buying Work In The US?
Building And Running Businesses In The ‘Spirit Of Bitcoin’
What Is The Mysterious Liver Disease Hurting (And Killing) Children?
Citigroup Trader Is Scapegoat For Flash Crash In European Stocks (#GotBitcoin)
Bird Flu Outbreak Approaches Worst Ever In U.S. With 37 Million Animals Dead
Financial Inequality Grouped By Race For Blacks, Whites And Hispanics
How Black Businesses Can Prosper From Targeting A Trillion-Dollar Black Culture Market (#GotBitcoin)
Ultimate Resource For Central Bank Digital Currencies (#GotBitcoin) Page#2
Meet The Crypto Angel Investor Running For Congress In Nevada (#GotBitcoin?)
Introducing BTCPay Vault – Use Any Hardware Wallet With BTCPay And Its Full Node (#GotBitcoin?)
How Not To Lose Your Coins In 2020: Alternative Recovery Methods (#GotBitcoin?)
H.R.5635 – Virtual Currency Tax Fairness Act of 2020 ($200.00 Limit) 116th Congress (2019-2020)
Adam Back On Satoshi Emails, Privacy Concerns And Bitcoin’s Early Days
The Prospect of Using Bitcoin To Build A New International Monetary System Is Getting Real
How To Raise Funds For Australia Wildfire Relief Efforts (Using Bitcoin And/Or Fiat )
Former Regulator Known As ‘Crypto Dad’ To Launch Digital-Dollar Think Tank (#GotBitcoin?)
Currency ‘Cold War’ Takes Center Stage At Pre-Davos Crypto Confab (#GotBitcoin?)
A Blockchain-Secured Home Security Camera Won Innovation Awards At CES 2020 Las Vegas
Bitcoin’s Had A Sensational 11 Years (#GotBitcoin?)
Sergey Nazarov And The Creation Of A Decentralized Network Of Oracles
Google Suspends MetaMask From Its Play App Store, Citing “Deceptive Services”
Christmas Shopping: Where To Buy With Crypto This Festive Season
At 8,990,000% Gains, Bitcoin Dwarfs All Other Investments This Decade
Coinbase CEO Armstrong Wins Patent For Tech Allowing Users To Email Bitcoin
Bitcoin Has Got Society To Think About The Nature Of Money
How DeFi Goes Mainstream In 2020: Focus On Usability (#GotBitcoin?)
Dissidents And Activists Have A Lot To Gain From Bitcoin, If Only They Knew It (#GotBitcoin?)
At A Refugee Camp In Iraq, A 16-Year-Old Syrian Is Teaching Crypto Basics
Bitclub Scheme Busted In The US, Promising High Returns From Mining
Bitcoin Advertised On French National TV
Germany: New Proposed Law Would Legalize Banks Holding Bitcoin
How To Earn And Spend Bitcoin On Black Friday 2019
The Ultimate List of Bitcoin Developments And Accomplishments
Charities Put A Bitcoin Twist On Giving Tuesday
Family Offices Finally Accept The Benefits of Investing In Bitcoin
An Army Of Bitcoin Devs Is Battle-Testing Upgrades To Privacy And Scaling
Bitcoin ‘Carry Trade’ Can Net Annual Gains With Little Risk, Says PlanB
Max Keiser: Bitcoin’s ‘Self-Settlement’ Is A Revolution Against Dollar
Blockchain Can And Will Replace The IRS
China Seizes The Blockchain Opportunity. How Should The US Respond? (#GotBitcoin?)
Jack Dorsey: You Can Buy A Fraction Of Berkshire Stock Or ‘Stack Sats’
Bitcoin Price Skyrockets $500 In Minutes As Bakkt BTC Contracts Hit Highs
Bitcoin’s Irreversibility Challenges International Private Law: Legal Scholar
Bitcoin Has Already Reached 40% Of Average Fiat Currency Lifespan
Yes, Even Bitcoin HODLers Can Lose Money In The Long-Term: Here’s How (#GotBitcoin?)
Unicef To Accept Donations In Bitcoin (#GotBitcoin?)
Former Prosecutor Asked To “Shut Down Bitcoin” And Is Now Face Of Crypto VC Investing (#GotBitcoin?)
Switzerland’s ‘Crypto Valley’ Is Bringing Blockchain To Zurich
Next Bitcoin Halving May Not Lead To Bull Market, Says Bitmain CEO
Bitcoin Developer Amir Taaki, “We Can Crash National Economies” (#GotBitcoin?)
Veteran Crypto And Stocks Trader Shares 6 Ways To Invest And Get Rich
Is Chainlink Blazing A Trail Independent Of Bitcoin?
Nearly $10 Billion In BTC Is Held In Wallets Of 8 Crypto Exchanges (#GotBitcoin?)
SEC Enters Settlement Talks With Alleged Fraudulent Firm Veritaseum (#GotBitcoin?)
Blockstream’s Samson Mow: Bitcoin’s Block Size Already ‘Too Big’
Attorneys Seek Bank Of Ireland Execs’ Testimony Against OneCoin Scammer (#GotBitcoin?)
OpenLibra Plans To Launch Permissionless Fork Of Facebook’s Stablecoin (#GotBitcoin?)
Tiny $217 Options Trade On Bitcoin Blockchain Could Be Wall Street’s Death Knell (#GotBitcoin?)
Class Action Accuses Tether And Bitfinex Of Market Manipulation (#GotBitcoin?)
Sharia Goldbugs: How ISIS Created A Currency For World Domination (#GotBitcoin?)
Bitcoin Eyes Demand As Hong Kong Protestors Announce Bank Run (#GotBitcoin?)
How To Securely Transfer Crypto To Your Heirs
‘Gold-Backed’ Crypto Token Promoter Karatbars Investigated By Florida Regulators (#GotBitcoin?)
Crypto News From The Spanish-Speaking World (#GotBitcoin?)
Financial Services Giant Morningstar To Offer Ratings For Crypto Assets (#GotBitcoin?)
‘Gold-Backed’ Crypto Token Promoter Karatbars Investigated By Florida Regulators (#GotBitcoin?)
The Original Sins Of Cryptocurrencies (#GotBitcoin?)
Bitcoin Is The Fraud? JPMorgan Metals Desk Fixed Gold Prices For Years (#GotBitcoin?)
Israeli Startup That Allows Offline Crypto Transactions Secures $4M (#GotBitcoin?)
[PSA] Non-genuine Trezor One Devices Spotted (#GotBitcoin?)
Bitcoin Stronger Than Ever But No One Seems To Care: Google Trends (#GotBitcoin?)
First-Ever SEC-Qualified Token Offering In US Raises $23 Million (#GotBitcoin?)
You Can Now Prove A Whole Blockchain With One Math Problem – Really
Crypto Mining Supply Fails To Meet Market Demand In Q2: TokenInsight
$2 Billion Lost In Mt. Gox Bitcoin Hack Can Be Recovered, Lawyer Claims (#GotBitcoin?)
Fed Chair Says Agency Monitoring Crypto But Not Developing Its Own (#GotBitcoin?)
Wesley Snipes Is Launching A Tokenized $25 Million Movie Fund (#GotBitcoin?)
Mystery 94K BTC Transaction Becomes Richest Non-Exchange Address (#GotBitcoin?)
A Crypto Fix For A Broken International Monetary System (#GotBitcoin?)
Four Out Of Five Top Bitcoin QR Code Generators Are Scams: Report (#GotBitcoin?)
Waves Platform And The Abyss To Jointly Launch Blockchain-Based Games Marketplace (#GotBitcoin?)
Bitmain Ramps Up Power And Efficiency With New Bitcoin Mining Machine (#GotBitcoin?)
Ledger Live Now Supports Over 1,250 Ethereum-Based ERC-20 Tokens (#GotBitcoin?)
Miss Finland: Bitcoin’s Risk Keeps Most Women Away From Cryptocurrency (#GotBitcoin?)
Artist Akon Loves BTC And Says, “It’s Controlled By The People” (#GotBitcoin?)
Ledger Live Now Supports Over 1,250 Ethereum-Based ERC-20 Tokens (#GotBitcoin?)
Co-Founder Of LinkedIn Presents Crypto Rap Video: Hamilton Vs. Satoshi (#GotBitcoin?)
Crypto Insurance Market To Grow, Lloyd’s Of London And Aon To Lead (#GotBitcoin?)
No ‘AltSeason’ Until Bitcoin Breaks $20K, Says Hedge Fund Manager (#GotBitcoin?)
NSA Working To Develop Quantum-Resistant Cryptocurrency: Report (#GotBitcoin?)
Custody Provider Legacy Trust Launches Crypto Pension Plan (#GotBitcoin?)
Vaneck, SolidX To Offer Limited Bitcoin ETF For Institutions Via Exemption (#GotBitcoin?)
Russell Okung: From NFL Superstar To Bitcoin Educator In 2 Years (#GotBitcoin?)
Bitcoin Miners Made $14 Billion To Date Securing The Network (#GotBitcoin?)
Why Does Amazon Want To Hire Blockchain Experts For Its Ads Division?
Argentina’s Economy Is In A Technical Default (#GotBitcoin?)
Blockchain-Based Fractional Ownership Used To Sell High-End Art (#GotBitcoin?)
Portugal Tax Authority: Bitcoin Trading And Payments Are Tax-Free (#GotBitcoin?)
Bitcoin ‘Failed Safe Haven Test’ After 7% Drop, Peter Schiff Gloats (#GotBitcoin?)
Bitcoin Dev Reveals Multisig UI Teaser For Hardware Wallets, Full Nodes (#GotBitcoin?)
Bitcoin Price: $10K Holds For Now As 50% Of CME Futures Set To Expire (#GotBitcoin?)
Bitcoin Realized Market Cap Hits $100 Billion For The First Time (#GotBitcoin?)
Stablecoins Begin To Look Beyond The Dollar (#GotBitcoin?)
Bank Of England Governor: Libra-Like Currency Could Replace US Dollar (#GotBitcoin?)
Binance Reveals ‘Venus’ — Its Own Project To Rival Facebook’s Libra (#GotBitcoin?)
The Real Benefits Of Blockchain Are Here. They’re Being Ignored (#GotBitcoin?)
CommBank Develops Blockchain Market To Boost Biodiversity (#GotBitcoin?)
SEC Approves Blockchain Tech Startup Securitize To Record Stock Transfers (#GotBitcoin?)
SegWit Creator Introduces New Language For Bitcoin Smart Contracts (#GotBitcoin?)
You Can Now Earn Bitcoin Rewards For Postmates Purchases (#GotBitcoin?)
Bitcoin Price ‘Will Struggle’ In Big Financial Crisis, Says Investor (#GotBitcoin?)
Fidelity Charitable Received Over $100M In Crypto Donations Since 2015 (#GotBitcoin?)
Would Blockchain Better Protect User Data Than FaceApp? Experts Answer (#GotBitcoin?)
Just The Existence Of Bitcoin Impacts Monetary Policy (#GotBitcoin?)
What Are The Biggest Alleged Crypto Heists And How Much Was Stolen? (#GotBitcoin?)
IRS To Cryptocurrency Owners: Come Clean, Or Else!
Coinbase Accidentally Saves Unencrypted Passwords Of 3,420 Customers (#GotBitcoin?)
Bitcoin Is A ‘Chaos Hedge, Or Schmuck Insurance‘ (#GotBitcoin?)
Bakkt Announces September 23 Launch Of Futures And Custody
Coinbase CEO: Institutions Depositing $200-400M Into Crypto Per Week (#GotBitcoin?)
Researchers Find Monero Mining Malware That Hides From Task Manager (#GotBitcoin?)
Crypto Dusting Attack Affects Nearly 300,000 Addresses (#GotBitcoin?)
A Case For Bitcoin As Recession Hedge In A Diversified Investment Portfolio (#GotBitcoin?)
SEC Guidance Gives Ammo To Lawsuit Claiming XRP Is Unregistered Security (#GotBitcoin?)
15 Countries To Develop Crypto Transaction Tracking System: Report (#GotBitcoin?)
US Department Of Commerce Offering 6-Figure Salary To Crypto Expert (#GotBitcoin?)
Mastercard Is Building A Team To Develop Crypto, Wallet Projects (#GotBitcoin?)
Canadian Bitcoin Educator Scams The Scammer And Donates Proceeds (#GotBitcoin?)
Amazon Wants To Build A Blockchain For Ads, New Job Listing Shows (#GotBitcoin?)
Shield Bitcoin Wallets From Theft Via Time Delay (#GotBitcoin?)
Blockstream Launches Bitcoin Mining Farm With Fidelity As Early Customer (#GotBitcoin?)
Commerzbank Tests Blockchain Machine To Machine Payments With Daimler (#GotBitcoin?)
Man Takes Bitcoin Miner Seller To Tribunal Over Electricity Bill And Wins (#GotBitcoin?)
Bitcoin’s Computing Power Sets Record As Over 100K New Miners Go Online (#GotBitcoin?)
Walmart Coin And Libra Perform Major Public Relations For Bitcoin (#GotBitcoin?)
Judge Says Buying Bitcoin Via Credit Card Not Necessarily A Cash Advance (#GotBitcoin?)
Poll: If You’re A Stockowner Or Crypto-Currency Holder. What Will You Do When The Recession Comes?
1 In 5 Crypto Holders Are Women, New Report Reveals (#GotBitcoin?)
Beating Bakkt, Ledgerx Is First To Launch ‘Physical’ Bitcoin Futures In Us (#GotBitcoin?)
Facebook Warns Investors That Libra Stablecoin May Never Launch (#GotBitcoin?)
Government Money Printing Is ‘Rocket Fuel’ For Bitcoin (#GotBitcoin?)
Bitcoin-Friendly Square Cash App Stock Price Up 56% In 2019 (#GotBitcoin?)
Safeway Shoppers Can Now Get Bitcoin Back As Change At 894 US Stores (#GotBitcoin?)
TD Ameritrade CEO: There’s ‘Heightened Interest Again’ With Bitcoin (#GotBitcoin?)
Venezuela Sets New Bitcoin Volume Record Thanks To 10,000,000% Inflation (#GotBitcoin?)
Newegg Adds Bitcoin Payment Option To 73 More Countries (#GotBitcoin?)
China’s Schizophrenic Relationship With Bitcoin (#GotBitcoin?)
More Companies Build Products Around Crypto Hardware Wallets (#GotBitcoin?)
Bakkt Is Scheduled To Start Testing Its Bitcoin Futures Contracts Today (#GotBitcoin?)
Bitcoin Network Now 8 Times More Powerful Than It Was At $20K Price (#GotBitcoin?)
Crypto Exchange BitMEX Under Investigation By CFTC: Bloomberg (#GotBitcoin?)
“Bitcoin An ‘Unstoppable Force,” Says US Congressman At Crypto Hearing (#GotBitcoin?)
Bitcoin Network Is Moving $3 Billion Daily, Up 210% Since April (#GotBitcoin?)
Cryptocurrency Startups Get Partial Green Light From Washington
Fundstrat’s Tom Lee: Bitcoin Pullback Is Healthy, Fewer Searches Аre Good (#GotBitcoin?)
Bitcoin Lightning Nodes Are Snatching Funds From Bad Actors (#GotBitcoin?)
The Provident Bank Now Offers Deposit Services For Crypto-Related Entities (#GotBitcoin?)
Bitcoin Could Help Stop News Censorship From Space (#GotBitcoin?)
US Sanctions On Iran Crypto Mining — Inevitable Or Impossible? (#GotBitcoin?)
US Lawmaker Reintroduces ‘Safe Harbor’ Crypto Tax Bill In Congress (#GotBitcoin?)
EU Central Bank Won’t Add Bitcoin To Reserves — Says It’s Not A Currency (#GotBitcoin?)
The Miami Dolphins Now Accept Bitcoin And Litecoin Crypt-Currency Payments (#GotBitcoin?)
Trump Bashes Bitcoin And Alt-Right Is Mad As Hell (#GotBitcoin?)
Goldman Sachs Ramps Up Development Of New Secret Crypto Project (#GotBitcoin?)
Blockchain And AI Bond, Explained (#GotBitcoin?)
Grayscale Bitcoin Trust Outperformed Indexes In First Half Of 2019 (#GotBitcoin?)
XRP Is The Worst Performing Major Crypto Of 2019 (GotBitcoin?)
Bitcoin Back Near $12K As BTC Shorters Lose $44 Million In One Morning (#GotBitcoin?)
As Deutsche Bank Axes 18K Jobs, Bitcoin Offers A ‘Plan ฿”: VanEck Exec (#GotBitcoin?)
Argentina Drives Global LocalBitcoins Volume To Highest Since November (#GotBitcoin?)
‘I Would Buy’ Bitcoin If Growth Continues — Investment Legend Mobius (#GotBitcoin?)
Lawmakers Push For New Bitcoin Rules (#GotBitcoin?)
Facebook’s Libra Is Bad For African Americans (#GotBitcoin?)
Crypto Firm Charity Announces Alliance To Support Feminine Health (#GotBitcoin?)
Canadian Startup Wants To Upgrade Millions Of ATMs To Sell Bitcoin (#GotBitcoin?)
Trump Says US ‘Should Match’ China’s Money Printing Game (#GotBitcoin?)
Casa Launches Lightning Node Mobile App For Bitcoin Newbies (#GotBitcoin?)
Bitcoin Rally Fuels Market In Crypto Derivatives (#GotBitcoin?)
World’s First Zero-Fiat ‘Bitcoin Bond’ Now Available On Bloomberg Terminal (#GotBitcoin?)
Buying Bitcoin Has Been Profitable 98.2% Of The Days Since Creation (#GotBitcoin?)
Another Crypto Exchange Receives License For Crypto Futures
From ‘Ponzi’ To ‘We’re Working On It’ — BIS Chief Reverses Stance On Crypto (#GotBitcoin?)
These Are The Cities Googling ‘Bitcoin’ As Interest Hits 17-Month High (#GotBitcoin?)
Venezuelan Explains How Bitcoin Saves His Family (#GotBitcoin?)
Quantum Computing Vs. Blockchain: Impact On Cryptography
This Fund Is Riding Bitcoin To Top (#GotBitcoin?)
Bitcoin’s Surge Leaves Smaller Digital Currencies In The Dust (#GotBitcoin?)
Bitcoin Exchange Hits $1 Trillion In Trading Volume (#GotBitcoin?)
Bitcoin Breaks $200 Billion Market Cap For The First Time In 17 Months (#GotBitcoin?)
You Can Now Make State Tax Payments In Bitcoin (#GotBitcoin?)
Religious Organizations Make Ideal Places To Mine Bitcoin (#GotBitcoin?)
Goldman Sacs And JP Morgan Chase Finally Concede To Crypto-Currencies (#GotBitcoin?)
Bitcoin Heading For Fifth Month Of Gains Despite Price Correction (#GotBitcoin?)
Breez Reveals Lightning-Powered Bitcoin Payments App For IPhone (#GotBitcoin?)
Big Four Auditing Firm PwC Releases Cryptocurrency Auditing Software (#GotBitcoin?)
Amazon-Owned Twitch Quietly Brings Back Bitcoin Payments (#GotBitcoin?)
JPMorgan Will Pilot ‘JPM Coin’ Stablecoin By End Of 2019: Report (#GotBitcoin?)
Is There A Big Short In Bitcoin? (#GotBitcoin?)
Coinbase Hit With Outage As Bitcoin Price Drops $1.8K In 15 Minutes
Samourai Wallet Releases Privacy-Enhancing CoinJoin Feature (#GotBitcoin?)
There Are Now More Than 5,000 Bitcoin ATMs Around The World (#GotBitcoin?)
You Can Now Get Bitcoin Rewards When Booking At Hotels.Com (#GotBitcoin?)
North America’s Largest Solar Bitcoin Mining Farm Coming To California (#GotBitcoin?)
Bitcoin On Track For Best Second Quarter Price Gain On Record (#GotBitcoin?)
Bitcoin Hash Rate Climbs To New Record High Boosting Network Security (#GotBitcoin?)
Bitcoin Exceeds 1Million Active Addresses While Coinbase Custodies $1.3B In Assets
Why Bitcoin’s Price Suddenly Surged Back $5K (#GotBitcoin?)
Zebpay Becomes First Exchange To Add Lightning Payments For All Users (#GotBitcoin?)
Coinbase’s New Customer Incentive: Interest Payments, With A Crypto Twist (#GotBitcoin?)
The Best Bitcoin Debit (Cashback) Cards Of 2019 (#GotBitcoin?)
Real Estate Brokerages Now Accepting Bitcoin (#GotBitcoin?)
Ernst & Young Introduces Tax Tool For Reporting Cryptocurrencies (#GotBitcoin?)
Recession Is Looming, or Not. Here’s How To Know (#GotBitcoin?)
How Will Bitcoin Behave During A Recession? (#GotBitcoin?)
Many U.S. Financial Officers Think a Recession Will Hit Next Year (#GotBitcoin?)
Definite Signs of An Imminent Recession (#GotBitcoin?)
What A Recession Could Mean for Women’s Unemployment (#GotBitcoin?)
Investors Run Out of Options As Bitcoin, Stocks, Bonds, Oil Cave To Recession Fears (#GotBitcoin?)
Goldman Is Looking To Reduce “Marcus” Lending Goal On Credit (Recession) Caution (#GotBitcoin?)


Leave a Reply
You must be logged in to post a comment.